Oral hygiene
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 18 Dec 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Oral hygiene means regularly brushing your teeth and cleaning between your teeth to keep your teeth and gums healthy. This helps to prevent tooth decay and gum disease.
In this article:
Video picks for Dental care and problems
Continue reading below
How to have good oral hygiene
Regular teeth brushing and cleaning between teeth helps to keep your teeth and gums healthy. These also help to prevent tooth decay and gum disease.
Other things that may help include:
Mouthwashes.
Dental floss or interdental brushes.
Tongue cleaning.
Eating a healthy diet, which includes limiting sugary drinks and foods.
If you smoke, stopping smoking.
Having a dental check-up at least once a year.
What's the best way to brush your teeth?
Back to contentsTeeth should be brushed twice a day, once just before bed and once first thing in the morning, before you have had anything to eat or drink.
Do not brush your teeth within thirty minutes of eating or drinking, particularly if you have eaten something sweet, as the brushing can rub the remains of the food into your teeth, rather than removing it.
Use a soft or medium toothbrush. The hard bristles of a firm toothbrush can damage gums.
Apply a small amount of a fluoride-containing toothpaste to your toothbrush and brush in a circular motion for two minutes.
Spit out the toothpaste but do not wash out your mouth with water, because the toothpaste which stays in contact with your teeth provides protection for several hours after you have brushed your teeth.
Sweet things should be eaten only at mealtimes. Chemicals in the saliva help to deal with any sugary residue and acid on your teeth. It takes about an hour after eating for the acidity in your mouth to return to normal, so if you are eating sweets and sweet snacks between meals your mouth may not get much chance to recover.
Children should be taught good oral hygiene as young as possible. Teeth can be brushed with a soft brush and a small amount of toothpaste twice a day as soon as they appear. See also the separate leaflet, How to protect your child's teeth.
Have regular dental checks at intervals recommended by your dentist (this is normally at least once a year). A dentist can detect a build-up of plaque and remove tartar (calculus). Early or mild gingivitis can be detected and treated to prevent the more severe periodontitis. A dentist can also advise about special coating of children's teeth to help prevent tooth decay.
Continue reading below
What is good oral hygiene?
Back to contentsIt is important to get into a regular habit of good oral hygiene - in particular, regular teeth brushing and cleaning between teeth.
Teeth brushing
Brush your teeth at least twice a day. Use a soft-tufted brush and a toothpaste that contains fluoride. The head of the brush should be small enough to get into all the areas of the mouth. Spend at least two minutes brushing, covering all areas (the inside, the outside and the biting areas of each tooth).
Pay particular attention to where the teeth meet the gum. Get a new toothbrush every 3-4 months. Studies suggest that powered toothbrushes with a rotation-oscillation action (where the brush rapidly changes direction of rotation) remove plaque and debris better than manual brushes.
Ideally, brush your teeth either just before eating, or at least half an hour after eating. The reason for this is to help prevent tooth erosion. Many foods contain acids - in particular, fizzy drinks (including fizzy water) and fruit juices.
After your teeth are exposed to acid, the enamel is a little softened. But, the action of calcium and other mineral salts in the saliva can help to counteract and reverse this softening. Therefore, do not brush teeth immediately after eating when the enamel tends to be at its softest. In particular, do not brush teeth straightaway after eating or drinking acid foods and drinks. It is best to wait at least half an hour after eating or drinking anything before brushing.
Brush children's teeth as soon as they erupt into the mouth. Use a smear of toothpaste for children aged less than 3 years and a pea-sized amount for children aged 3-6 years.
What about cleaning between teeth?
Clean between your teeth after brushing once a day, but ideally twice a day. This is to remove plaque from between teeth. Dental floss is commonly used to do this. However, some studies suggest that small interdental brushes may do a better job than floss. The aim is:
To clean the sides of the teeth where a toothbrush cannot reach.
To clear the spaces between teeth (the interdental spaces) of debris.
Some people who have not cleaned between their teeth before are surprised as to how much extra debris and food particles can be removed by doing this in addition to brushing.
If you are not sure how to clean between your teeth then ask your dentist or dental hygienist. Briefly: normal floss looks a bit like cotton thread. Cut off about 40 cm. Wind the ends round your middle fingers of each hand. Then grab the floss between the thumbs and first finger to obtain a tight 3-4 cm section which you can pull between teeth. Gently scrape the floss against the sides of each tooth from the gum outwards. Use a fresh piece of floss each time.
Some people prefer floss tape which slides between teeth more easily than normal floss. Also, some people use disposable plastic forks with a small length of floss between the two prongs. These may be easier to hold and manipulate. However, they are expensive. Some people use sticks, or small interdental brushes to clean the space between the teeth.
The gums may bleed a little when you first begin to clean between your teeth. This should settle in a few days. If it persists then see a dentist, as regular bleeding may indicate gum disease.
Food and drink
Sugars and sugary foods in the mouth are the main foods that germs thrive on to make acid which can contribute to tooth decay. Acid foods and drinks are also a main factor in tooth erosion. So, some tips:
Limit the amount of sugary foods and drinks that you have. In particular, don't snack on sugary foods.
Try to reduce the amount of acid in contact with your teeth. So, limit fizzy drinks (including fizzy water) and fruit juices as these tend to be acidic. Perhaps just limit yourself to one fizzy or fruit juice drink a day. Otherwise, choose drinks that are much less acidic, such as still water, and milk, tea, or coffee (without sugar).
Restrict fruit juice and smoothies at mealtimes. They are both high in natural sugars.. The current recommendation is for a maximum of a single 150 ml portion of fruit juice once a day with meals - this counts as one of your 'five a day'.
Avoid 'juice drinks' which usually contain high levels of added sugar. Overall their sugar content is often much higher than the level of natural sugar in fruit juice.
Drink any acid drinks, such as fizzy drinks and fruit juices, quickly. Don't swish them around your mouth or hold them in your mouth for any period of time. Drinking through a straw makes it less likely that the acid will come into prolonged contact with your teeth.
Opt for sugar-free snacks between meals - cheese, crackers, toast, carrot sticks or fruit. Even though fruit contains natural sugars, the other health benefits from eating fruit make it worthwhile.
Realistically, there will be occasions when you or your children do consume sugary treats or drinks outside of mealtimes. Try to limit these events to only once or twice a week and opt for things that can be consumed briskly. A cake or cookie eaten in a few minutes will cause less tooth weakening than a packet of sweets that are sucked or chewed for an hour.
Chew sugar-free gum after meals. The gum will help to rub plaque from the tooth surfaces and will also stimulate the flow of saliva.
Do not brush your teeth within an hour of being sick. This is because stomach acid will be part of the vomit. The acid may attack your tooth enamel and brushing may further damage it. It is better to immediately wash your mouth out with water.
What other things can I do?
Back to contentsThe measures above are usually sufficient. However:
Many people also use an antiseptic mouthwash each day to help prevent gum disease. In particular, for those who are unable to use a toothbrush, regular rinsing with an antiseptic mouthwash will help to clean the teeth.
Many people also clean their tongue after cleaning their teeth. You can do this with a toothbrush. You can also buy a special plastic tongue scraper from pharmacies.
If you smoke, you should aim to stop smoking. Smoking is a major risk factor for developing gum disease.
If children need medicines, wherever possible use sugar-free medicines.
Some people chew sugar-free gum after each meal. Chewing gum increases the flow of saliva. Saliva helps to flush the mouth to help clear any debris and acid remaining from the meal.
Continue reading below
Why is it important?
Back to contentsGood oral hygiene helps to prevent dental problems - mainly plaque and tartar (calculus) which are the main causes of gum disease and tooth decay(dental caries). Good oral hygiene may also help to prevent or delay dental erosion.
Dental plaque is a soft whitish deposit that forms on the surface of teeth. It forms when germs (bacteria) combine with food and saliva. Plaque contains many types of bacteria. You can remove plaque by good oral hygiene.
Tartar (calculus) is hardened calcified plaque. It sticks firmly to teeth. Generally, it can only be removed with special instruments by a dentist or a dental hygienist.
When you eat sweet food, the sugar that comes in contact with your teeth provides food for the bacteria in the plaque. They digest it and release acid which erodes into the surface of the tooth, eventually making a hole in the hard outer enamel layer and forming a cavity in the deeper layers of the tooth.
What common problems are related to poor oral hygiene?
Back to contentsVarious problems are associated with poor oral hygiene, depending on which area of the mouth is affected.
Tooth decay
When holes form in parts of the enamel of a tooth, it is known as dental caries. A main cause of caries is a build-up of plaque. The germs in the plaque react with sugars and starches in food to form acids. The acids are kept next to the teeth by the sticky plaque and dissolve the tooth enamel.
Once there is a hole in the hard enamel which protects the outside of the tooth, the decay process can cause cavities in the tooth structure. If you have tooth decay you may need fillings, crowns or inlays.
Tooth erosion
Tooth (dental) erosion is a common problem. It is the gradual erosion of tooth enamel by the action of acid on the teeth. This is different to damage caused by bacteria resulting in tooth decay and caries.
Tooth erosion affects the entire surface of the tooth. In time, tooth erosion can cause thinned enamel, and eventually can expose the softer dentine underneath the enamel. Dentine is sensitive, so erosion can lead to your teeth being more sensitive to hot, cold or sweet foods and drink.
Gum disease
Tooth with gum disease
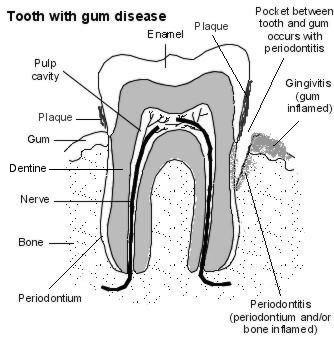
Gum disease (periodontal disease) means infection or inflammation of the tissues that surround the teeth. Most cases of gum disease are plaque-related. Plaque contains many different types of bacteria and a build-up of some types of bacteria is associated with developing gum disease.
Depending on the severity, gum disease is generally divided into two types - gingivitis and periodontitis:
Gingivitis means inflammation of the gums. There are various types. However, most cases of gingivitis are caused by plaque.
Periodontitis occurs if gingivitis becomes worse and progresses to involve the tissue that joins the teeth to the gums (the periodontal membrane).
Gum disease is the most common cause of tooth loss in adults. It is also a main cause of bad breath (halitosis). However, gum disease is often treatable.
Bad breath
Bad breath (halitosis) can be caused by poor oral hygiene. The smell is caused by the build-up of bacteria in the mouth.
What other conditions are related to having poor oral hygiene?
Back to contentsPoor oral hygiene is not just associated with problems in your mouth. There are a number of other conditions which have been linked to gum disease.
It is thought that germs entering the bloodstream from the mouth can travel elsewhere in the body, making infections more likely. Also, the inflammation response that happens when you have gingivitis or periodontitis can also trigger inflammation elsewhere. This can be associated with the development of some of the diseases below.
Oral hygiene, gum disease and heart disease
In addition to the benefits to your teeth, good mouth hygiene may have even further benefits. There is some evidence to suggest that poor oral hygiene is associated with an increased risk of developing heart diseases such as:
Heart attack and angina.
Other blood vessel-related problems (cardiovascular disease).
Other diseases which may be linked to poor oral hygiene
Links have also been drawn between poor oral hygiene and:
Diabetes - poor oral hygiene may be a trigger for diabetes to develop and may also make it more likely that complications of diabetes will occur.
Cancer, especially pancreatic and oropharyngeal.
Pregnancy problems such as preterm birth and low birth weight.
Further research is needed to clarify these possible links. But, in the meantime, it may be an additional reason to look after your teeth and gums.
Patient picks for Dental care and problems

Oral and dental care
Teeth straightening
Misaligned teeth can undermine your confidence, make you smile less and affect your personal and social life. Fortunately, there are many orthodontic teeth straightening solutions available that will leave you with beautifully straight teeth and confidence to smile more. Teeth straightening is almost exclusively carried out by private dentists and cost will vary depending on treatment and service provider.
by Toothpick

Oral and dental care
Knocked-out tooth
About one in four children in the UK will injure a front tooth at some stage. Tooth injuries also happen to some adults. Sometimes a tooth may be completely knocked out. This leaflet tells you what to do.
by Dr Jan Sambrook, MRCGP
Further reading and references
- de Oliveira C, Watt R, Hamer M; Toothbrushing, inflammation, and risk of cardiovascular disease: results from BMJ. 2010 May 27;340:c2451. doi: 10.1136/bmj.c2451.
- Slot DE, Dorfer CE, Van der Weijden GA; The efficacy of interdental brushes on plaque and parameters of periodontal inflammation: a systematic review. Int J Dent Hyg. 2008 Nov;6(4):253-64.
- Oral health promotion: general dental practice; NICE Guidance (December 2015)
- Yaacob M, Worthington HV, Deacon SA, et al; Powered versus manual toothbrushing for oral health. Cochrane Database Syst Rev. 2014 Jun 17;(6):CD002281. doi: 10.1002/14651858.CD002281.pub3.
- Halitosis; NICE CKS, September 2024 (UK access only)
- Isomura ET, Suna S, Kurakami H, et al; Not brushing teeth at night may increase the risk of cardiovascular disease. Sci Rep. 2023 Jun 28;13(1):10467. doi: 10.1038/s41598-023-37738-1.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Dec 2028
18 Dec 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.