Insomnia
Poor sleep
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 23 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
As many as one in three people can have some difficulty with sleeping. However, there are many things you can do to help yourself. This leaflet aims to show you some of them. For example, simple things like winding down before bedtime, avoiding certain foods and drinks, and a bedtime routine can help.
EDITORS NOTES
Dr Krishna Vakharia, 24th November 2023
There is a new oral medication that NICE has recommended called daridorexant. This can only be used under certain conditions. Your doctor will discuss if it is suitable for you. For further information take a look at the further reading section.
In this article:
What is insomnia?
Continue reading below
What is insomnia?
Insomnia means poor sleep. About one third of adults do not get as much sleep as they would like. Poor sleep can mean:
Not being able to get off to sleep.
Waking up too early.
Waking for long periods in the night.
Not feeling refreshed after a night's sleep.
If you have poor sleep, particularly over a long period of time, it can severely affect your life, as it can cause:
Tiredness (fatigue) and loss of energy in the daytime.
Poor concentration.
Loss of interest in usual activities.
Irritability.
Depression and anxiety.
Inability to do things as well or as much as usual - for example, work, social activities, exercise. Errors might occur at work or whilst driving, which could have serious consequences.
A worse quality of life.
What is a normal amount of sleep?
Back to contentsDifferent people need different amounts of sleep. Children need more sleep than adults. For adults, the minimum we need is about 6 hours per night. On average, most adults need between 6 and 9 hours of sleep to feel refreshed.
Most people establish a pattern that is normal for them in their early adult life. However, as you become older, it is normal to sleep less. For most people it takes less than thirty minutes to fall asleep.
So, everyone is different. What is important is that the amount of sleep that you get should be sufficient for you, and that you usually feel refreshed and not sleepy during the daytime. Therefore, the strict medical definition of insomnia is: 'Difficulty in getting to sleep, difficulty staying asleep, early wakening, or non-restorative sleep despite adequate time and opportunity to sleep, resulting in impaired daytime functioning, such as poor concentration, mood disturbance, and daytime tiredness.'
Further ways to promote sleep in more difficult cases include relaxation techniques, regular exercise and certain psychological therapies.
Sleeping tablets are not the best way to help with sleep problems because they don't fix the cause of insomnia, you can get addicted to them, and they often stop working if you take them regularly.
Continue reading below
Understanding normal sleep
Back to contentsA normal night's sleep has three main parts:
Quiet sleep. This is divided into stages 1-4. Each stage becomes more deep. Quiet sleep is sometimes called deep sleep.
Rapid eye movement (REM) sleep. REM sleep occurs when the brain is very active but the body is limp, apart from the eyes which move rapidly. Most dreaming occurs during REM sleep.
Short periods of waking for 1-2 minutes.
Each night, about 4-5 periods of quiet sleep alternate with 4-5 periods of REM sleep. In addition, several short periods of waking for 1-2 minutes occur about every two hours or so, but occur more frequently towards the end of the night's sleep. The graph below shows a typical normal pattern of sleep in a young adult.
Hypnogram
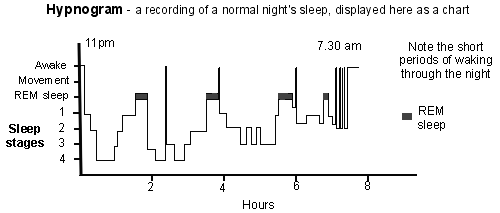
Normally, you do not remember the times that you wake if they last less than two minutes. If you are distracted during the wakeful times (for example, a partner snoring, traffic noise, etc) then the wakeful times tend to last longer and you are more likely to remember them.
What causes insomnia?
Back to contentsPoor sleep may develop for no apparent reason. However, there are a number of possible causes which include the following:
Concern about wakefulness
You may remember the normal times of being awake in the night. You may feel that to wake in the night is not normal, and worry about getting back off to sleep. You may clock-watch and check the time each time you wake up.
This may make you irritated or anxious, and you are more likely to remember the times of wakefulness. You may then have an impression of having a bad night's sleep, even when the total amount of time asleep was normal.
Temporary problems
Poor sleep is often temporary. This may be because of stress, a work or family problem, jet lag, a change of routine, a new baby, a strange bed, etc. Poor sleep in these situations usually improves in time.
Stress, anxiety or depression
You may find it difficult to switch off your anxieties about work, home or personal problems. Also, poor sleep is sometimes due to depression. Other symptoms of depression include a low mood, lethargy, poor concentration, tearfulness and persistent negative thoughts. Depression is common. Treatment of depression or anxiety often cures the poor sleep too.
Sleep apnoea
This sometimes occurs in people who snore, most commonly in obese people. In this condition the large airways narrow or collapse as you fall asleep. This not only causes snoring but also reduces the amount of oxygen that gets to the lungs.
This causes you to wake up to breathe properly. You may wake up many times each night which may result in daytime tiredness. See the separate leaflet called Sleep apnoea. Note: most people who snore do not have sleep apnoea and they do sleep well.
Other illnesses
Various illnesses keep some people awake. For example, illness causing pain, leg cramps, breathlessness, indigestion, cough, itch, hot flushes, mental health problems, etc.
Stimulants
These can interfere with sleep. There are three common culprits.
Alcohol - many people take an alcoholic drink to help sleep. Alcohol does help you get to sleep quicker, but then causes broken, poor-quality sleep and early morning wakefulness.
Caffeine - which is in tea, coffee, some soft drinks such as cola, and even chocolate. It is also in some painkiller tablets and other medicines (check the ingredients on the medicine packet). Caffeine is a stimulant and may cause poor sleep.
Nicotine (from smoking) is a stimulant, so it would help not to smoke.
Other recreational drugs
Other recreational drugs (for example, ecstasy, cocaine, cannabis and amphetamines) can affect sleep.
Prescribed medicines
Some medicines sometimes interfere with sleep. For example, 'water tablets' (diuretics), some antidepressants, steroids, beta-blockers, painkillers containing caffeine, and some cold remedies containing pseudoephedrine. Also, if you suddenly stop taking regular sleeping tablets or other sedative medicines, this can cause rebound poor sleep.
Screen time
There is some evidence that the time we spend looking at electronic screens can affect our sleep. It may be that certain types of light from e-readers and electronic tablets can disrupt control of our natural day-and-night cycle.
There are studies which suggest we may sleep better after reading a printed book or a particular kind of screen before bedtime. There are also some studies which show that in children and adolescents, more time using electronic devices in the daytime is linked to less good sleep at night. It's best to avoid using screens within an hour or two of bed. Try to keep devices like phones and laptops out of reach of the bed, or, ideally, outside the bedroom entirely.
Unrealistic expectations
Some people just need less sleep than others. If your sleep pattern has not changed, and you do not feel sleepy during the day, you are probably getting enough sleep. Older people and people who do little exercise tend to need less sleep. Some people think they should be able to nap during the day - and sleep eight hours at night!
A vicious cycle
Whatever the initial cause, worry about poor sleep and worry about feeling tired the next day are common reasons for the problem to become worse.
Sleep paralysis
Some people may also experience waking from sleep but then being unable to move or speak for a period of time. Some people experience the same problems when they are falling asleep. See the separate leaflet called Sleep paralysis.
Continue reading below
Insomnia classifications
Back to contentsThere are different definitions and classifications of poor sleep (insomnia) around, which can make things confusing. Doctors may classify insomnia into one of the following categories:
By type
Primary insomnia is insomnia that occurs when no illness or other secondary cause (comorbidity) is identified. Primary insomnia accounts for about one in five cases of long-term insomnia.
Secondary (or comorbid) insomnia occurs when insomnia is a symptom of, or is associated with, other conditions. These can be medical or mental health conditions, or drug or substance misuse (as discussed above).
By duration
Short-term if insomnia lasts days to weeks, and up to three months.
Long-term (or persistent) if insomnia lasts for three months or longer.
By a combination of factors
Some authorities use the term 'chronic insomnia disorder'. To have this diagnosis, you would:
Have problems sleeping for at least three nights a week for at least three months.
Be distressed or have problems functioning due to your sleeping problem.
Not have another condition which could affect sleep, ie mental or physical illnesses or another sleep disorder.
How can I sleep better?
Back to contentsAvoid caffeine, smoking and alcohol, especially in the hours before bedtime.
Avoid heavy meals or strenuous exercise shortly before going to bed.
Go to bed and get up at the same time each day.
Regular daytime exercise helps you feel more relaxed and tired at bedtime.
This section will discuss five topics which can help to promote better sleep:
Understanding some facts.
Sleep hygiene.
Relaxation techniques.
Daytime exercise.
Psychological treatments called cognitive and behavioural therapies.
In effect, these can be used in a step-wise fashion. You need only go on to the next step if the previous step is not very helpful, but each step requires a greater degree of effort.
Understanding some facts
It is often helpful to understand that short periods of waking each night are normal. Some people are reassured about this and so do not become anxious when they find themselves awake in the night.
Also, remember that worry about poor sleep can itself make things worse. Also, it is common to have a few bad nights if you have a period of stress, anxiety or worry. This is often just for a short time and a normal sleep pattern often resumes after a few days.
General tips for sleeping better (often called sleep hygiene)
The following are commonly advised to help promote sleep in people with sleep difficulties, and may be all that is necessary:
Reduce caffeine - do not have any food, medicines, or drinks that contain caffeine or other stimulants for six hours before bedtime (see above). Some people have found that cutting out caffeine completely through the day has helped.
Do not smoke within six hours before bedtime.
Do not drink alcohol within six hours before bedtime.
Do not have a heavy meal just before bedtime (although a light snack may be helpful).
Do not do any strenuous exercise within four hours of bedtime (but exercising earlier in the day is helpful).
Body rhythms - try to get into a routine of wakefulness during the day and sleepiness at night. The body becomes used to rhythms or routines. If you keep to a pattern, you are more likely to sleep well. Therefore:
No matter how tired you are, do not sleep or nap during the day.
It is best to go to bed only when sleepy-tired in the late evening.
Switch the light out as soon as you get into bed.
Always get up at the same time each day, seven days a week, however short the time asleep. Use an alarm to help with this. Resist the temptation to lie in - even after a poor night's sleep. Do not use weekends to catch up on sleep, as this may upset the natural body rhythm that you have got used to in the week.
The bedroom should be a quiet, relaxing place to sleep:
It should not be too hot, cold, or noisy.
Earplugs and eye shades may be useful if you are sleeping with a snoring or wakeful partner.
Make sure the bedroom is dark with good curtains to stop early morning sunlight.
Don't use the bedroom for activities such as work, eating or television.
Consider changing your bed if it is old, or not comfortable.
Hide your alarm clock under your bed. Many people will clock-watch and this does not help you to get off to sleep.
Mood and atmosphere - try to relax and wind down with a routine before going to bed. For example:
A stroll followed by a bath, some reading, and a warm drink (without caffeine) may be relaxing in the late evening.
Do not do anything mentally demanding within 90 minutes of going to bed - such as studying.
Go to bed when sleepy-tired.
Some people find playing soft music is helpful at bedtime. Try a player with a time switch that turns the music off after about 30 minutes.
If you cannot get off to sleep after 20-30 minutes - then get up. It's best not to just lie in bed, worrying about getting to sleep. Get up and do something you find relaxing until you feel sleepy, and then go back to bed.
Relaxation techniques
These aim to reduce your mental and physical arousal before going to bed. Relaxation techniques may help even if you are not anxious but find it hard to get off to sleep. There are a number of techniques.
For example, progressive muscular relaxation has been shown to help promote sleep. This technique consists of tensing and relaxing various muscle groups in sequence. For more information, see the leaflet called Relaxation exercises.
You can find a podcast or app that takes you through deep-breathing exercises, and other methods to help you relax. See Further Reading below.
Daytime exercise
Regular daytime exercise can help you to feel more relaxed and tired at bedtime. This may help you to sleep better. (However, you should not do exercise near to bedtime if you have insomnia.) If possible, do some exercise on most days.
Even a walk in the afternoon or early evening is better than nothing. However, ideally, you should aim for at least 30 minutes of moderate exercise on five or more days a week.
Moderate exercise means that you get warm and slightly out of breath. You do not need to go to a gym! Brisk walking, jogging, cycling, climbing stairs, heavy DIY, heavy gardening, dancing and heavy housework are all moderate-intensity physical exercises. See the separate leaflet called Exercise and physical activity.
Behavioural and cognitive therapies
If you have severe persistent poor sleep, your doctor may refer you to a psychologist or other health professional for psychological treatments. These are various therapies which help re-train your brain and the way you feel, think or behave.
Research studies have found that there is a good chance that behavioural and cognitive therapies will improve sleep in adults with insomnia. Increasingly, research has also shown that some of these therapies can be delivered digitally (ie through an app, online, etc).
There are various types of therapy and they include the following:
Stimulus-control therapy. This helps you to re-associate the bed and bedroom with sleep and to re-establish a consistent sleep/wake pattern.
Sleep restriction therapy. Very briefly, the principle of this treatment is that you limit the time that you spend in bed at night. As things improve, the time in bed is then lengthened. An example of the way that this may be done in practice is as follows:
First, you may be asked to find out how much you are actually sleeping each night. You can do this by keeping a sleep diary.
You may then be advised to restrict the amount of time that you spend in bed to the time that you actually sleep each night. For example, if you spend eight hours in bed each night but you sleep for only six hours then your allowed time in bed would be six hours. So, in this example, say you normally go to bed at 11 pm, get to sleep at 1 am and get up at 7 am. To restrict your time in bed to six hours, you may be advised to go to bed at 1 am but still get up at 7 am.
You then make weekly adjustments to the allowed time in bed, depending on the time spent asleep. (You need to keep on with the sleep diary.)
When 90% of the time spent in bed is spent asleep then the allowed time spent in bed is increased by 15 minutes, by going to bed 15 minutes earlier. In the above example, you would then go to bed at 12.45 am.
Adjustments are made each week until you are sleeping for a longer length most nights.
Relaxation training. This teaches you ways of reducing tension. For example, this may include the progressive muscle relaxation technique as described earlier, plus various other techniques described earlier.
Paradoxical intention. This involves staying passively awake, avoiding any intention to fall asleep. It is used for people who have trouble getting to sleep (but not maintaining sleep).
Biofeedback. With this technique, you are connected to electrical sensors which give you feedback by sounds and lights to show you what your body is doing. This is to help you control certain body functions (such as muscle tension).
Cognitive therapy. Cognitive therapy is often used in combination with a behavioural intervention (such as stimulus control, sleep restriction, or relaxation training); this is then called cognitive behavioural therapy (CBT).
See the separate article CBT for insomnia: how does it work? for more details.
Accessing sleep-focused therapy
There are various different ways to access sleep-focused therapy. What's available on the NHS varies a little depending on where you are.
Your GP may be able to refer you for sessions led by a psychotherapist or psychologist. These can be individual or group sessions, and may be in-person, over the phone, or via video call.
There are also online courses and apps. Sleepio is one example of an app that uses cognitive behavioural therapy for insomnia (CBT-I). Sleepio was recommended for use by the UK's National Institute for Health and Care Excellence (NICE) in 2022. In some areas of the UK it's available free on the NHS; in other places you may need to pay a subscription.
Other resources include:
Sleepstation (also available free on the NHS in some areas).
Calm, a meditation app (free trial, then paid).
Headspace, a guided meditation app (free trial, then paid).
Pzizz, an app that aims to help you relax and fall asleep quicker (free download, with in-app purchases and subscription).
See the separate article How to improve your sleep behaviour for more details.
What about sleeping tablets?
Back to contentsSleeping tablets are not usually advised for insomnia
The main types of sleeping tablets are in a class of medicines called benzodiazepines and a class called Z drugs. To read more about why these medicines may be prescribed, see the separate leaflet called Benzodiazepines and Z drugs.
In the past, sleeping tablets were commonly prescribed. However, they have been shown to have problems and are now not commonly prescribed.
If a sleeping tablet is prescribed, it is usually just a short course (a week or so) to get over a particularly bad patch.
Possible problems with sleeping tablets include:
Drowsiness the next day. You may not be safe to drive or to operate machinery.
Clumsiness and confusion in the night if you have to get up. For example, if you have had a sleeping tablet, you may fall over if you get up in the night to go to the toilet. (Older people who take sleeping tablets have an increased risk of falling and breaking their hip.)
Tolerance to sleeping tablets may develop if you take them regularly. This means that, in time, the usual dose has no effect. You then need a higher dose to help with sleep. In time, the higher dose then has no effect, and so on.
Some people become addicted to (dependent on) sleeping tablets and have withdrawal symptoms if the tablets are stopped suddenly.
Other medicines that may be used to help sleep include melatonin and some antihistamines.
Herbal remedies are used by some people to help with sleep. For example, valerian.
However, research studies have shown that there is very little evidence to show that these work. Therefore, they are not recommended.
Long-term use of sleeping tablets has been linked with serious health problems, such as an increased risk of dementia, and an increased risk of earlier death.
If you've been taking sleeping tablets for a long time, your doctor should regularly review them with you, including discussing the benefits and harms. If you want to stop, they are no longer helping, or they are becoming harmful, your doctor may suggest stopping them - usually in a gradual way and with support.
A final note
Back to contentsSee a doctor if you feel that illness or medication is causing poor sleep. Treating any underlying condition that is causing the problem, if possible, can help to promote sleep. In particular, depression and anxiety are common causes of poor sleep and can often be treated.
Patient picks for Sleep and insomnia

Healthy living
Sleepwalking
Sleepwalking usually occurs during a period of deep sleep and often occurs in the first few hours after falling asleep. Sleepwalking is more common in children than in adults. There is no specific treatment for sleepwalking. However, there is a lot of advice, such as regular bedtimes, that can help to reduce sleepwalking. The most important action is to make simple adjustments in the home to avoid accidents when sleepwalking. Most children will grow out of sleepwalking before becoming teenagers.
by Dr Colin Tidy, MRCGP

Healthy living
Sleeping tablets
Doctors avoid prescribing sleeping tablets if possible due to the problems they can cause and the concern that you could become dependent on them.
by Dr Colin Tidy, MRCGP
Further reading and references
- Buysse DJ, Germain A, Moul DE, et al; Efficacy of brief behavioral treatment for chronic insomnia in older adults. Arch Intern Med. 2011 May 23;171(10):887-95. Epub 2011 Jan 24.
- Buysse DJ; Insomnia. JAMA. 2013 Feb 20;309(7):706-16. doi: 10.1001/jama.2013.193.
- Luik AI, Kyle SD, Espie CA; Digital Cognitive Behavioral Therapy (dCBT) for Insomnia: a State-of-the-Science Review. Curr Sleep Med Rep. 2017;3(2):48-56. doi: 10.1007/s40675-017-0065-4. Epub 2017 May 8.
- Qaseem A, Kansagara D, Forciea MA, et al; Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2016 Jul 19;165(2):125-33. doi: 10.7326/M15-2175. Epub 2016 May 3.
- Wilson S, Anderson K, Baldwin D, et al; British Association for Psychopharmacology consensus statement on evidence-based treatment of insomnia, parasomnias and circadian rhythm disorders: An update. J Psychopharmacol. 2019 Aug;33(8):923-947. doi: 10.1177/0269881119855343. Epub 2019 Jul 4.
- Medicines associated with dependence or withdrawal symptoms: safe prescribing and withdrawal management for adults; NICE guidance (April 2022)
- Sleepio to treat insomnia and insomnia symptoms; NICE medical technologies guidance, May 2022
- Insomnia; NICE CKS, April 2024 (UK access only)
- Sleep Diary; The Sleep Charity.
- Sleepio app
- Sleepstation app
- Calm app
- Headspace app
- Pzizz app
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 22 Jun 2027
23 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.