Left lower quadrant pain
Lower left abdominal pain
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 15 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Left lower quadrant (LLQ) pain is abdominal pain that is mainly in the lower half on the left-hand side. There are many causes of LLQ pain.
In this article:
Video picks for Abdominal pain
Key points
Left lower quadrant (LLQ) pain is pain on the left side of your abdomen (stomach), below your belly button.
Common causes include constipation, gastroenteritis, IBS, diverticulitis, and endometriosis. However, there are many other causes.
The treatment for LLQ pain depends on the cause but may include dietary changes, pain relief, and in severe cases surgery.
Continue reading below
Where is my left lower quadrant?
Look down at your abdomen and mentally divide the area from the bottom of your ribs down to your pubic hair into four quarters. The quarter on your left side below your belly button is your left lower quadrant (LLQ).
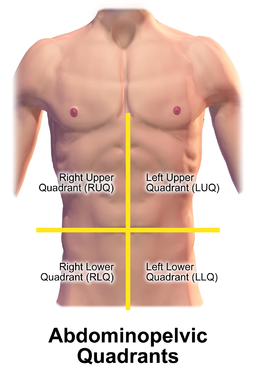
© By Blausen.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436
What organs are in my left lower quadrant?
The left lower quadrant contains organs including:
Small bowel (ileum).
Parts of the large bowel (colon).
Rectum.
Left ureter.
Left ovary and Fallopian tube in women.
The skin, nerves and blood vessels of that area.
Causes of left lower quadrant pain
Back to contentsThere are lots of causes of LLQ pain; they include:
Constipation.
Gastroenteritis and food poisoning.
Irritable bowel syndrome (IBS).
Diverticulitis.
Colon and rectal cancer.
Endometriosis.
Pelvic inflammatory disease.
Torsion of the testicle.
Constipation
Constipation can cause discomfort anywhere in your abdomen.
It is caused by poo backing up in the colon; the discomfort or pain is due to the colon being stretched.
You will often (but not always) be aware that you are not opening your bowels as often as usual.
Your poo will often be hard and pellet-like; sometimes it is painful to pass.
Occasionally (and mainly in children or older adults) there will be loose stools (diarrhoea) because the constipation is higher up and causing a blockage; the poo becomes watery and seeps around the edge of the blockage. This is called "overflow diarrhoea".
Gastroenteritis and food poisoning
Gastroenteritis, which is usually caused by a virus, is an infection which can cause pain anywhere in your abdomen.
It can also cause diarrhoea, make you feel sick (nausea) or be sick (vomit).
The pain often feels cramping and it may ease for a while each time some diarrhoea is passed.
Food poisoning may be caused by a virus or a bacteria, and has similar symptoms to gastroenteritis. If you think you have food poisoning, a poo test may be sent after 7 days of symptoms to look for particular bacteria.
Irritable bowel syndrome (IBS)
Irritable bowel syndrome (IBS) tends to cause crampy abdominal pains and bloating.
It comes and goes and may be associated with diarrhoea and/or constipation.
Diverticulitis
Diverticulitis in the last part of the large gut (sigmoid colon) is the most common cause of left lower quadrant (LLQ) pain in adults.
It usually comes with a temperature (fever) and a change in bowel habit (opening your bowels more or less often than usual for you).
Colon cancer and rectal cancer
Severe LLQ pain, bloating and not being able to open your bowels at all, not even to pass wind (flatus), are symptoms that suggest you may have a colon cancer that is blocking your bowel. You should seek urgent medical advice.
Colon cancer and rectal cancer (sometimes called colorectal cancer) are two of the more common cancers in the UK and can cause left lower quadrant (LLQ) pain.
Although colon cancer can affect any part of the large bowel (colon), it commonly affects the last part (descending colon and sigmoid colon) which is on the left-hand side. Rectal cancer affects the very last part of the large bowel (rectum) just before it ends at the anus.
You may notice changes in how often you open your bowels, a feeling of not fully emptying your rectum, unexplained weight loss or low energy levels, and the presence of blood in your poo (faeces).
Trapped inguinal or femoral hernia
A left inguinal or femoral hernia does not usually cause much pain but, if it becomes strangulated, it can cause pain in the groin and in the abdomen, usually on the side of the hernia but it may cause pain over the whole abdomen.
If it happens on the left-hand side, there will be a tender swelling in the left groin.
They occur when a piece of bowel or other tissue from inside the abdomen pushes through a weakness in the muscles of the abdominal wall near the left groin (where the left thigh meets your lower abdomen).
Continue reading below
Left lower quadrant pain causes in women
Back to contentsOvulation pain (mittelschmerz)
Ovulation is the point at which your ovary releases an egg - this is usually about halfway between two periods.
Mittelschmerz or ovulation pain is when women experience pain when this happens.
Between 1 and 2 in 5 women experience ovulation pain.
It can be severe and last a few minutes or more of a dull pain which lasts a few hours.
It will only be felt on one side, but can be right or left.
You may get similar pain on the same or other side of your abdomen at the same point in another cycle.
Pelvic inflammatory disease
Pelvic inflammatory disease causes pain that is usually on both sides of the abdomen but can be in the (left lower quadrant) LLQ.
Pain is often worse during sex because the cervix (neck of the womb) is very tender.
You may also have abnormal bleeding, feel generally unwell and feverish, and have smelly vaginal discharge.
Twisted ovary
Twisted ovary (ovarian torsion) usually only occurs if a fluid-filled sac (cyst) has developed on the ovary.
Pain can be constant or intermittent.
Endometriosis
Endometriosis can sometimes cause constant lower abdominal pain, although usually it is worse just before, during and for a short while after a period.
Pain is usually across the lower part of the abdomen but it can be just on the left side.
Ectopic pregnancy
You should always see a doctor urgently if you think you might be pregnant and are experiencing LLQ pain. You could have an ectopic pregnancy.
Ectopic pregnancy is a pregnancy that is developing in the Fallopian tube instead of in your womb.
It can cause left lower quadrant pain that is sudden or gradually worsening, and may become severe.
Vaginal bleeding is common but may differ from a normal period (lighter/heavier, darker, or mistaken for a late period). Not everyone who has an ectopic pregnancy has bleeding.
Associated symptoms can include diarrhoea, pain on passing stool, dizziness, faintness, or feeling unwell
Shoulder-tip pain may occur due to internal bleeding irritating the diaphragm.
There is also a separate leaflet called Left Lower quadrant pain in pregnancy.
Ovarian cancer
Sometimes ovarian cancer presents with pain or a feeling of pressure in the lower half of the abdomen. This can be on one side or across the whole area.
Women with ovarian cancer may notice bloating.
Left lower quadrant pain causes in men
Back to contentsAny pain coming from the left side of the scrotum can cause pain in the left lower quadrant (LLQ) but usually the pain in the scrotum will be worse than the pain in the abdomen.
Torsion of the testicle
Torsion of the testicle (testis) is where the testicle twists and the blood supply is cut off.
It causes severe pain in the scrotum and severe lower quadrant pain, usually on one side.
The testicle is very tender.
This is a medical emergency and you should attend your nearest Emergency Department immediately.
Epididymo-orchitis
Epididymo-orchitis is an inflammation of the testicle and/or the tubes surrounding it (epididymis).
The affected side of the scrotum can swell and become red and tender.
Sometimes epididymo-orchitis causes less severe pain but is usually tender on examination.
Continue reading below
Other possible causes of left lower quadrant pain
Back to contentsInflammatory bowel disease (IBD): IBD (Crohn's disease and ulcerative colitis) cause the lining of the gut to become inflamed, and this can cause pain in the left lower quadrant (LLQ).
Sigmoid volvulus: This happens when the very last part of the large bowel, the sigmoid, twists on itself causing a blockage. This causes colicky pain and a severely bloated abdomen. It is dangerous and requires emergency surgery.
Kidney stones: A stone that passes into the ureter draining urine from your right kidney may cause pain that starts in your right loin and spreads to your groin and left lower quadrant (LLQ), or into your testicle if you are a man.
Shingles: A sharp or burning pain may be felt in the abdomen before a rash develops.
Abdominal aortic aneurysm: This can cause pain before it bursts. The pain is usually felt in your back or the middle of your abdomen but it can occasionally be felt in the left (or right) lower quadrant.
Referred pain: Pain from your back or hip may be felt around the front into the left (or right) lower quadrant.
Muscle sprains: This can cause pain in your abdomen when you use the pulled or strained muscle to move, cough or laugh.
When to see a doctor
Back to contentsIf you have a pain which doesn't settle, you will probably need to consult a health professional to help you figure out the cause.
Consult a doctor urgently if you:
Have very severe pain.
Have persistent sickness (vomiting).
Have recently lost weight without trying to do so.
Feel giddy, light-headed, faint or breathless.
Notice blood in your poo (faeces) or on the toilet paper.
Have a change from your usual bowel habit. This means you may open your bowels more or less often than usual, causing bouts of diarrhoea or constipation.
Could be pregnant (you should do a pregnancy test from a pharmacy first).
Have severe pain in your scrotum which started suddenly or over a short period of time.
Notice bloating which is getting worse.
How is left lower quadrant pain diagnosed?
Back to contentsYour doctor will usually be able to diagnose the cause of your left lower quadrant (LLQ) pain by talking to you to find out about the pain, and examining you.
They will examine your abdomen, including in the area you have the pain. They may sometimes need to examine your bottom (this does not happen in children except by specialists in very rare situations). You may also be asked to provide a sample of urine (pee), to rule out infection.
Women may need an internal examination to rule out or diagnose problems such as pelvic inflammatory disease. Men may need an examination of their scrotum and testicles.
You should always be offered a chaperone for an intimate examination.
Swabs might be taken from women to look for infections such as chlamydia - in men, these are usually tested for by a urine sample.
You may also need blood tests to:
Check the function of your liver and kidneys.
Rule out any inflammation or infection in your body.
Look for anaemia.
Check your blood sugar level.
Further tests
If your doctor is still unsure of the cause of pain, they may recommend further tests such as:
Further blood tests, for example for coeliac disease.
Stool (poo) tests to look for blood or inflammation.
Ultrasound scan - this is particularly used to look at your ovaries and womb if you are a woman, testicles if you are a man, and the bladder and kidneys.
Computerised tomography (CT) scan - this is used to look for diverticula in the bowel, and also to look at your kidneys. Depending on where you live, your GP might be able to organise a CT scan for specific conditions.
Very occasionally, an X-ray may be used to look for constipation - this is mainly in young children where the diagnosis is unclear.
If the answers are still not clear, you may be referred for further tests including:
Colonoscopy - this is when a small camera (a scope) is used to check your large bowel.
Sigmoidoscopy - this is when a camera is used to check the lower part of your large bowel.
Magnetic resonance imaging (MRI) scan - this can be used to look at many of the organs in your abdomen.
Nobody will need all these tests, and some people may not need any.
Left lower quadrant pain treatment
Back to contentsThe treatment for left lower quadrant (LLQ) pain depends on the cause. See the relevant leaflet for the condition with which you have been diagnosed. Treatments for a few of the causes of LLQ pain are briefly discussed below.
Constipation. This can be avoided by eating plenty of fruit and vegetables, as well as other foods containing fibre. If your constipation is mild, adding these things to your diet might be enough to treat the constipation. You may be prescribed medication to treat your constipation. Nowadays this is usually with a liquid.
Gastroenteritis and food poisoning. Most people do not need any treatment for this. Small children and elderly adults may become very unwell and need fluids through a drip. It is usually best to avoid medications to try and stop the diarrhoea as this usually makes the symptoms last longer. If the diarrhoea continues for 7 days, a poo test might be done. If this shows a bacteria, then antibiotics might be suggested.
Irritable bowel syndrome. Some people can manage their pain from irritable bowel syndrome by changing their diet and avoiding any "trigger foods". You may be prescribed medication which reduces the spasming of your bowel. These can also be bought over the counter.
Diverticulitis. Diverticulitis causing pain and fever often needs antibiotics to treat it. It can usually be treated with antibiotics by mouth but some people need to be admitted to hospital for antibiotics into a vein.
Colon and rectal cancer. Bowel cancer is often treated with surgery or chemotherapy or both together. The treatment depends on where in the bowel the cancer is and how advanced it is when the cancer is found.
Endometriosis. Endometriosis is usually treated with hormones - for example, the oral contraceptive pill. Some women may need different hormonal treatments or surgery; both of these would be provided by a gynaecologist.
Pelvic inflammatory disease. This is treated with antibiotics.
Ectopic pregnancy. This is usually treated with emergency surgery but some women can be treated with a tablet called methotrexate if the pregnancy is very small. A blood test to measure the level of pregnancy hormone in your blood will usually help the doctors to decide which treatment is best for you.
Torsion of the testicle. This is treated with emergency surgery to untwist the testicle. The testicle is usually then "fixed" in place so that it cannot happen again.
What is the outlook?
Back to contentsThe outlook for left lower quadrant (LLQ) pain depends entirely on the cause of the pain. Some conditions settle very quickly on their own (for example, gastroenteritis), or with the help of antibiotics (for example, a kidney infection). Others can be cured with surgery, such as torsion of the testis.
Some are long-term conditions, such as Crohn's disease or coeliac disease. There is no cure for these conditions but there are treatments which will manage the symptoms.
Your doctor should be able to give you an idea of the outlook (prognosis) once a diagnosis has become clear.
Frequently asked questions
Back to contentsWhat causes lower left quadrant pain when breathing?
Left lower quadrant pain when taking a deep breath in will often be due to muscle pain. If it persists more than a few days and you are not aware of having pulled any muscles, or if it is getting worse rather than better, you should seek medical attention.
What causes lower left quadrant pain when coughing?
Left lower quadrant pain when taking a deep breath in will often be due to muscle pain. If it persists more than a few days and you are not aware of having pulled any muscles, or if it is getting worse rather than better, you should seek medical attention.
What causes lower left quadrant pain when walking?
Left lower quadrant pain when taking a deep breath in will often be due to muscle pain. It could also be due to pain from your hip being "referred" into your abdomen. This means that, although the pain is coming from your hip, your brain thinks it is coming from the abdomen.
Can kidney infection cause lower left quadrant pain?
A kidney infection can cause pain anywhere along your urinary tract (from your kidney, down your ureter, or in your bladder or your urethra). So this could be anywhere from your loin (just below your ribs), round the side and down to the left lower quadrant (LLQ). However, it would be unusual to have pain in the LLQ only, it would usually be associated with pain in the left loin as well.
Patient picks for Abdominal pain

Digestive health
Appendicitis
Appendicitis is inflammation of the appendix, a small pouch on the gut wall connected to the large intestine. It is a medical emergency as, left untreated, the appendix can burst or perforate.
by Dr Colin Tidy, MRCGP

Digestive health
Right upper quadrant pain
Right upper quadrant (RUQ) pain is pain located in the upper part of the abdomen on your right-hand side. There are many causes of RUQ pain.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Oct 2027
15 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.