Hyperlipidaemia
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 24 Jul 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:High cholesterolFamilial hypercholesterolaemiaStatins and other lipid-lowering medicines
Hyperlipidaemia means a high level of cholesterol or triglycerides in your blood.
At a glance
Hyperlipidaemia means having high levels of lipids (fats) in your blood.
Causes include being overweight, drinking too much alcohol, or inherited genes.
Other medical conditions or some medicines can also cause it.
It is often found during routine blood tests, for example, during an annual health check.
You can lower lipid levels through a healthy diet and sometimes medication.
In this article:
Video picks for High cholesterol
Continue reading below
What causes hyperlipidaemia?
Hyperlipidaemia is often found when people are overweight or have an unhealthy diet. It can also be the result of drinking too much alcohol. It can be something that you may have inherited through your family genes (known as primary hyperlipidaemia) and approximately 1 person in 500 will have this cause.
Other conditions
It may be because of another medical condition that you may have, such as diabetes, when it is known as secondary. Other causes include:
Medicine side-effects
Some prescribed medicines can affect your cholesterol level, including:
Thiazide diuretics (used to control blood pressure).
Ciclosporin (used after organ transplants).
Antiretroviral therapy (used to treat HIV infection).
Beta-blockers (used to control heart rate).
Atypical antipsychotics (used in some mental health problems).
Retinoic acid derivatives (used in some skin conditions).
How do I know if I have hyperlipidaemia?
Back to contentsHyperlipidaemia is often found during routine screening when your doctor is trying to assess your risk of having heart attacks or strokes. This may be as part of an annual health check if you are over 40 years of age, or if you have a close relative who had these problems at a young age.
Usually, the diagnosis is made after a blood test. It used to be the case that we always asked people to fast (not eat) for 8-12 hours before the blood test, but this is now usually not needed. The person who requests the blood test will tell you if you need to fast for it.
There are also changes that may be visible on your body if you have the inherited form of hyperlipidaemia:
Premature arcus senilis - this is a white or grey ring that is visible when your doctor looks at the front of your eyes.
Arcus senilis
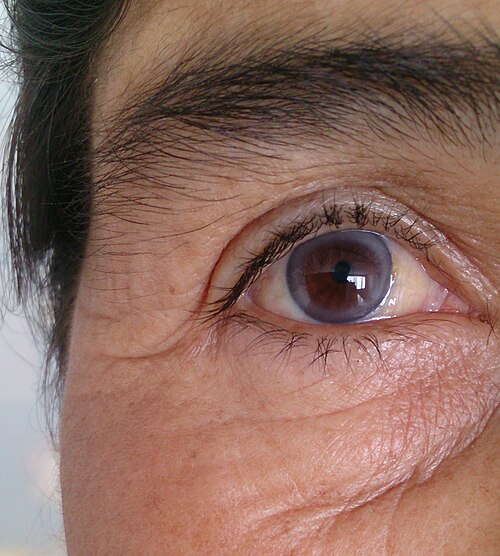
© Afrodriguezg, CC BY-SA 4.0, via Wikimedia Commons
Tendon xanthomata - these are hard nodules that you may find in the tendons of the knuckles and the Achilles (at the back of your ankle).
Xanthelasma - fatty deposits in the eyelids.
Xanthelasma_palpebrarum
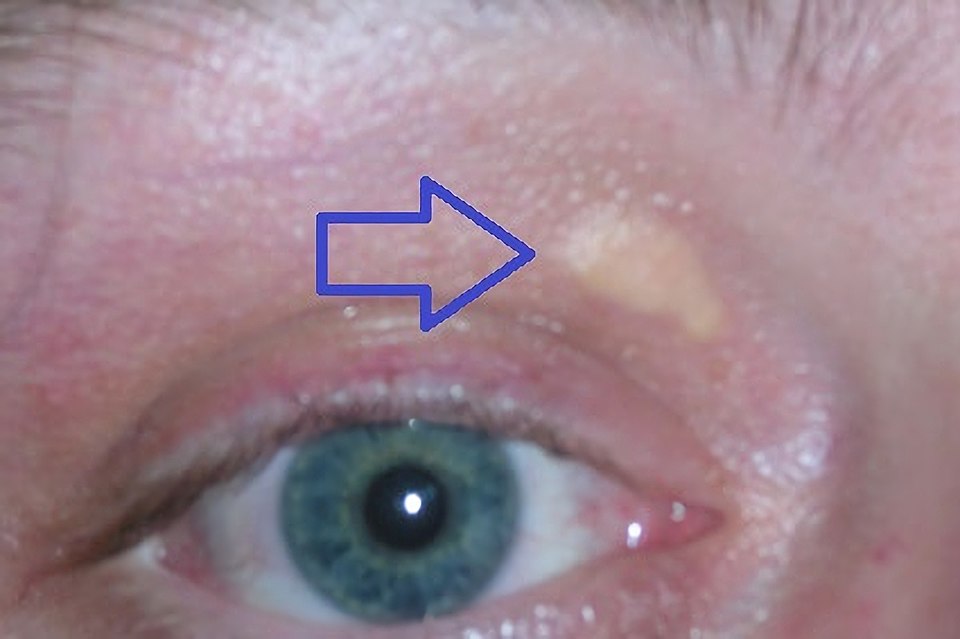
© Bobtheowl2 at the English Wikipedia, CC BY-SA 3.0 , via Wikimedia Commons
See the separate leaflet called Familial hypercholesterolaemia.
Continue reading below
What can I do to lower my lipid levels?
Back to contentsHyperlipidaemia can be treated both by eating a healthy diet and by taking a medicine to reduce your cholesterol level. It is also very important to lower any other risk factors for cardiovascular diseases, such as doing regular physical activity and not smoking. See the separate leaflet called Cardiovascular disease (Atheroma) for more information.
The decision as to whether you need medication is usually taken by your healthcare professional by putting your information into an online calculator. This uses a variety of factors to predict your risk of having a cardiovascular event such as a heart attack or stroke. If your risk is over 10% then you will usually be offered medication, however if you would like to first try diet and other lifestyle change then you can do that and arrange a re-test in 6-12 months. Some people are always offered medication, with no need to do a risk calculation. This includes those who have already been found to have arterial disease (for example, angina, heart attack, stroke), and those who have type 1 diabetes, chronic kidney disease, or a type of raised cholesterol which is inherited.
Diet
Changing from an unhealthy diet to a healthy diet can reduce a cholesterol level. However, dietary changes alone rarely lower a cholesterol level enough to change a person's risk of cardiovascular disease from a high-risk category to a lower-risk category. A healthy diet has other benefits too, apart from reducing the level of cholesterol. See also the separate leaflet called Healthy eating.
Medication
If you are at high risk of developing a cardiovascular disease then medication is usually advised along with advice to tackle any lifestyle issues, including diet. Medication can be used to lower your cholesterol or triglyceride level, usually with a statin medicine. Read more about statins and other lipid-lowering medicines for further details. Most medication is taken by mouth, but there is some newer medications (for example, evolocumab and incliseran) which are given by injection. They are usually prescribed by specialists rather than by GPs.
Patient picks for High cholesterol

Heart health and blood vessels
Familial hypercholesterolaemia
Familial hypercholesterolaemia is inherited high cholesterol. It is a condition where you have a very high cholesterol level in your blood.
by Dr Colin Tidy, MRCGP

Heart health and blood vessels
High cholesterol
Cholesterol is a fat chemical (lipid) that is made in the cells in your body. Many different cells make cholesterol but cells in the liver make about a quarter of the total. You need some cholesterol to keep healthy.
by Dr Rosalyn Adleman, MRCGP
Frequently asked questions
What is the difference between primary and secondary hyperlipidaemia?
Primary hyperlipidaemia is inherited through family genes, affecting about 1 in 500 people. Secondary hyperlipidaemia is caused by another medical condition, such as diabetes, an underactive thyroid, or chronic kidney disease.
Can high blood pressure medications cause hyperlipidaemia?
Yes, some prescribed medicines can affect your cholesterol level, including certain types used to control blood pressure, such as thiazide diuretics and beta-blockers.
Are there any physical signs of hyperlipidaemia?
If you have the inherited form of hyperlipidaemia, there may be visible changes. These can include a white or grey ring around the iris of your eyes (premature arcus senilis), hard nodules in the tendons of your knuckles and Achilles (tendon xanthomata), and fatty deposits in your eyelids (xanthelasma).
Do I always need to fast before a blood test for hyperlipidaemia?
It used to be common practice to fast for 8-12 hours before a blood test for hyperlipidaemia, but this is usually not needed anymore. The person requesting your blood test will tell you if you specifically need to fast.
How do doctors decide if I need medication for hyperlipidaemia?
Your healthcare professional will typically use an online calculator that considers various factors to predict your risk of a cardiovascular event. If your risk is over 10%, medication is usually offered. However, some people are always offered medication without a risk calculation, such as those with existing arterial disease, type 1 diabetes, chronic kidney disease, or inherited forms of high cholesterol. If your risk permits, you may also choose to try diet and lifestyle changes first and then be re-tested.
Can I lower my lipid levels with diet alone?
While changing to a healthy diet can reduce cholesterol levels, dietary changes alone rarely lower cholesterol enough to shift a person from a high-risk category for cardiovascular disease to a lower-risk category. A healthy diet does, however, offer other benefits beyond cholesterol reduction.
What are some of the newer medications for hyperlipidaemia?
Besides statins, which are commonly taken by mouth, there are newer injectable medications like evolocumab and incliseran. These newer medications are typically prescribed by specialists rather than by general practitioners.
Further reading and references
- Cardiovascular disease: risk assessment and reduction, including lipid modification; NICE guidance (December 2023)
- Familial hypercholesterolaemia: identification and management; NICE Clinical Guideline (2008, last updated October 2019)
- Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk; European Society of Cardiology/European Atherosclerosis Society (2019)
- Lipid modification - CVD prevention; NICE CKS, March 2025 (UK access only).
- 2021 European Guidelines on cardiovascular disease prevention in clinical practice; European Society of Cardiology (2021)
- Hypercholesterolaemia - familial; NICE CKS, April 2024 (UK access only)
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 23 Jul 2028
24 Jul 2025 | Latest version
14 Oct 2011 | Originally published

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.