Penis problems, itchy penis, and penis pain
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 10 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Premature ejaculationBalanitisPeyronie's diseasePenile cancerCircumcisionPhimosis and paraphimosis
There are a number of penis problems that can result in penis pain, an itchy penis or general penile discomfort. For example, different types of infection or inflammation can cause itch or pain in the penis, such as thrush, herpes, and eczema. Sometimes there are other symptoms, like bumps or ulcers on the penis, or discharge from the penis.
In this article:
Video picks for Penis problems
Continue reading below
What causes an itchy penis?
An itchy penis is often due to a fungal infection such as thrush. This is also known as candidiasis.
It can be a sign of diabetes mellitus but this most often has other symptoms too such as:
Tiredness.
Excessive thirst.
Needing to pee a lot.
Alternatively, penis itching can sometimes be a symptom of a condition called balanitis. This is the term used to describe inflammation at the head of the penis, which can also cause penis pain.
The tip of the penis may also be:
Red.
Sore.
In addition, you may notice pain when you:
Wee.
Have sex.
Sometimes there is bleeding or a smell coming from your foreskin, which usually develops over a few days.
Balanitis can be caused by poor hygiene and infections picked up during sexual activity or sexual intercourse, such as:
Crabs (public lice).
It can also be caused by infections not linked to sexual activity, such as thrush.
Our separate leaflet on Balanitis has more information.
An itchy foreskin can be caused by posthitis, which means inflammation of the foreskin. This has similar causes and treatment to balanitis.
Things that can result in penile skin itching and affect the shaft of the penis include:
Thrush.
Allergies.
Irritants.
More generalised skin problems such as psoriasis.
Other skin conditions that can make your penis itch include:
Contact dermatitis (where you come into contact with something you are allergic to, such as soaps or shampoo)
An itchy penis can also sometimes be a cause of a lower urinary tract infection in men (UTI), which can again be a source of penile discomfort and penis pain.
A doctor can often diagnose the condition just by its appearance, but sometimes tests are needed. The treatment depends on the cause.
What causes penis pain?
Back to contentsThere are several causes of penis pain which we discuss in more detail below. Causes of penis pain include:
An injury due to a fall or during sports.
Strenuous sexual activity.
Penile fracture - force applied to an erect penis that damages the fibrous part of the shaft. There is no bone in the penis.
Non-sexually transmitted infections, such as yeast infections leading to balanitis.
A paraphimosis, where the foreskin has been pulled back and gets stuck (this is a medical emergency).
Continue reading below
Peyronie's disease
Back to contentsIn this condition, thickened areas of scar tissue (fibrous plaques) appear along the shaft of the penis. As a result the penis can develop a bend or assume a deformed shape. The exact cause is unknown but there are several theories. With Peyronie's disease, painful erections and problems with penetration during sex are common.
In most cases tests are not needed, but occasionally a scan is suggested if a blood circulation problem affecting the penis is suspected. The medical treatment includes:
Medication that can be swallowed; or
Medicines applied directly to the surface of the penis; or
Injections into the areas of scarring.
Other treatment options are available. In most cases, the condition stays the same or becomes worse, but occasionally it gets better with time.
See the separate leaflet called Peyronie's disease for additional information.
Hypospadias
Back to contentsYour urethra is the tube running from your bladder down the length of your penis, which your urine comes out of. Hypospadias is a malformation of the urethra and penis that some babies are born with. It can cause difficulties with the urine flow. In later life, there may be erection problems.
There are a number of different forms. In mild cases, the urethra may just open lower down from its usual position. In severe forms, it can open right down at the base of the penis, by the scrotum. Other abnormalities of the foreskin or the underside of the penis may also occur.
Tests are not usually needed unless it is suspected that the abnormalities of the penis are part of a wider disorder (such as 'intersex syndrome'). Treatment may not be needed for milder cases, but many patients require some form of corrective surgery. This is particularly true if there are problems with the direction of urine flow or erection difficulties.
See the separate leaflet called Hypospadias for additional information.
Continue reading below
Discharge from the penis
Back to contentsDischarge from the penis is usually caused by inflammation of the urethra. The medical term is urethritis. You may notice a burning pain or urge to pass urine, but this doesn't always happen. Some men don't get any symptoms.
Usually, the cause is a sexually transmitted disease or infection. The common causes are:
Gonorrhoea.
Non-gonococcal urethritis (NGU).
It's more common in younger men, especially men who have sex with men.
As the name suggests, infections other than gonorrhoea can be a cause of NGU.
Chlamydia, a germ (bacterium) is a common cause of NGU. Irritants to the urethra can also be to blame, such as:
Soap.
Spermicides.
Putting a tube (catheter) in to drain the bladder.
Infections causing urethritis usually need treatment to clear. You may still be infectious, even if the symptoms have gone.
If you have a discharge from the penis get checked out by your GP, a sexual health clinic, or a genitourinary medicine (GUM) clinic.
Don't have sex until you and your sexual partner(s) have been tested. Even after treatment, you must avoid sex until it's shown that any infection has been cleared by treatment.
For additional information, see the separate leaflets called:
Lumps on the penis
Back to contentsMany men have tiny bumps around the bottom of the head of the penis. These are called penile pearly papules (see the photo below), and are normal and harmless.
Penile pearly papules
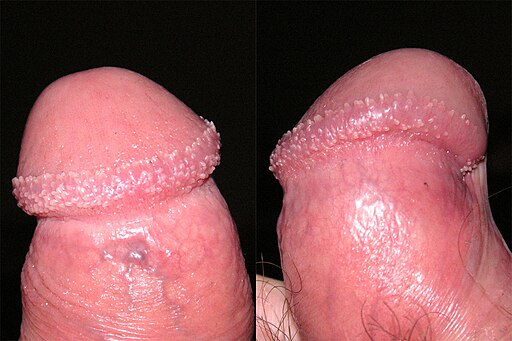
© No machine-readable author provided. Kissekatt assumed (based on copyright claims)., Public domain, via Wikimedia Commons
Another common cause for lumps on the penis is warts, also called anogenital warts or simply genital warts.
They look like little lumps on the outer skin of the penis.
They also sometimes occur around the anus.
They are caused by infection with the human papillomavirus (HPV).
They are passed on by skin-to-skin contact.
This is mainly during sexual contact, but can occur in other circumstances (eg, from mother to baby during birth).
Warts on the penis usually don't cause any penis pain or symptoms but people seek treatment because of their appearance. It's best to visit a GUM clinic to get checked out for other infections.
Genital warts are not cancers, but some types of HPV can increase the risk of certain cancers, such as:
Anal cancer.
Vulval cancer (in women).
Cervical cancer (in women).
Persistent HPV infection is the leading cause of cervical cancer.
The warts can be left alone, or removed by a variety of methods such as chemicals, freezing, burning, lasers or surgery. New warts develop after treatment in 1 in 4 cases, due to reactivation of the infection.
Condoms - both male and female - help reduce the risk of acquiring genital warts but don't abolish it because of contact with uncovered skin. Sex toys can pass on the virus and should not be shared. A vaccine is now available against HPV infection which is offered to boys and girls aged 12 to 13 years.
See the separate leaflet called Genital warts for additional information.
Circumcision
Back to contentsThis is an operation in which the foreskin is cut off and the remaining skin stitched back. It is usually performed for a condition called phimosis. Phimosis means tightening of the foreskin. This can result in difficulties in pulling the foreskin over the head of the penis and sometimes penis pain.
If the foreskin is pulled back for cleaning or insertion of a tube (catheter) to drain the bladder, and it is not pulled forwards again, the head of the penis (glans) can swell. The foreskin can become trapped under the swollen glans: this is called a paraphimosis. It's not uncommon for this to result in penis pain.
Steroid cream or an operation to loosen the foreskin can sometimes be used if it is not too tight. Otherwise, a circumcision is required.
Sometimes a circumcision is done for religious or hygienic reasons. Other reasons include:
An infection of the glans, called balanitis (see above).
An infection of the foreskin, called posthitis.
A skin condition called balanitis xerotica obliterans.
See the separate leaflet called Circumcision for additional information.
Erectile dysfunction
Back to contentsThis is also called erectile dysfunction or impotence. There are 2 types of ED:
You can't maintain an erection long enough to complete sexual intercourse; or
You're unable to get an erection at all.
A lot of men have ED now and again, often as a result of stress or tiredness. It can, however, become a more persistent problem. Long-term ED is more likely to happen as you become older.
There are many causes of persistent ED, including:
Circulation problems to the penis.
Diseases of (or injury to) the nerve supply.
Lack of the male hormone (testosterone).
Other causes include:
Recreational drugs.
Cycling.
Leakage of blood through the veins of the penis.
Psychological causes.
If your ED is due to a circulatory cause (as many cases are) you will need checks to make sure you don't have a more general problem with the state of your circulatory system, including your heart. These may include:
Blood tests to rule out raised cholesterol and diabetes.
A blood pressure check.
Your lifestyle will also be reviewed (eg, weight, exercise, smoking and alcohol intake).
Treatment options will include:
Removing any of the aggravating factors such as excessive alcohol or stress.
Medication in the form of cream.
Tablets that you swallow.
Injections or pellets put in the urethra.
Other options include:
Vacuum devices
A rod inserted into the penis (a prosthesis).
See the separate leaflet called Erectile dysfunction (Impotence) for additional information.
Penile cancer
Back to contentsThis is also known as penis cancer. It is very rare, affecting 1 in 100,000 men in Europe. A cancerous (malignant) tumour grows from one abnormal cell. It is not known why this happens but certain factors are known to increase the risk. These include:
Age (it is more common over the age of 50).
Becoming infected with the human papillomavirus (HPV).
Certain rare skin conditions (eg, erythroplasia of Queyrat and balanitis xerotica obliterans).
Poor hygiene in adults and having phimosis can increase the risk. Having a circumcision as a baby seems to have a protective effect.
The first sign of penile cancer is an alteration in the colour of the skin either:
On the head of the penis (the glans).
Or the underside of the foreskin if you have not been circumcised.
It never occurs on the shaft.
Eventually, the whole of the glans and/or foreskin can become involved.
You will probably need removal of some tissue for analysis (a biopsy) and some scans to confirm the size and spread of the cancer.
Treatment options include:
Surgery.
Chemotherapy.
See the separate leaflet called Penile cancer for additional information.
Patient picks for Penis problems

Men's health
Penis problems, itchy penis, and penis pain
There are a number of penis problems that can result in penis pain, an itchy penis or general penile discomfort. For example, different types of infection or inflammation can cause itch or pain in the penis, such as thrush, herpes, and eczema. Sometimes there are other symptoms, like bumps or ulcers on the penis, or discharge from the penis.
by Dr Doug McKechnie, MRCGP

Men's health
Peyronie's disease
Peyronie's disease causes a curved or bent penis. It is caused by scar tissue forming along the shaft of the penis. This causes painful erections and a bend or curve, usually about halfway along the penis. The change in shape is usually only obvious when the penis is erect.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Snodgrass W, Bush N; Recent advances in understanding/management of hypospadias. F1000Prime Rep. 2014 Nov 4;6:101. doi: 10.12703/P6-101. eCollection 2014.
- van der Horst HJ, de Wall LL; Hypospadias, all there is to know. Eur J Pediatr. 2017 Apr;176(4):435-441. doi: 10.1007/s00431-017-2864-5. Epub 2017 Feb 11.
- Peyronie's disease; British Association of Urological Surgeons (BAUS), 2020
- Balanitis; NICE CKS, May 2024 (UK access only)
- Penile curvature; European Association of Urology, Sexual and Reproductive Health guidelines, 2023
- European guideline for the management of balanoposthitis; Journal of the European Academy of Dermatology and Venereology, 2022
- Nam JK, Lee DH, Park SW, et al; Clinicopathologic Characteristics and Treatment Outcomes of Penile Cancer. World J Mens Health. 2017 Apr;35(1):28-33. doi: 10.5534/wjmh.2017.35.1.28.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Oct 2027
10 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.