Acute bronchitis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 18 Jan 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Chest infectionPneumoniaAspiration pneumoniaPost-operative chest infectionBronchoscopy
Acute bronchitis is a common chest infection that causes inflammation of the airways. It is usually caused by viral infections and often gets better on its own within a few weeks. See a doctor if symptoms don't improve or you have trouble breathing.
This leaflet explains the symptoms to look out for and how to manage them.
In this article:
Video picks for Chest and lung infections
Key points
Acute bronchitis is a lung infection that causes inflammation of the airways. It is mainly caused by viral infections such as the common cold or flu.
Common symptoms include a persistent cough with mucus, chest tightness, mild fever, wheezing, and tiredness.
Most cases often improve on their own with plenty of rest, fluids, and symptom management.
You should see a doctor if bronchitis symptoms are severe, last longer than three weeks, or include high fever, chest pain, or difficulty breathing.
Continue reading below
What is acute bronchitis?
What is bronchitis?
Acute bronchitis is an infection of the large airways (the bronchi). It is common and is usually due to a viral infection. A bacterial Infection is less common and causes around 1% to 10% of cases of bronchitis.
Respiratory tract
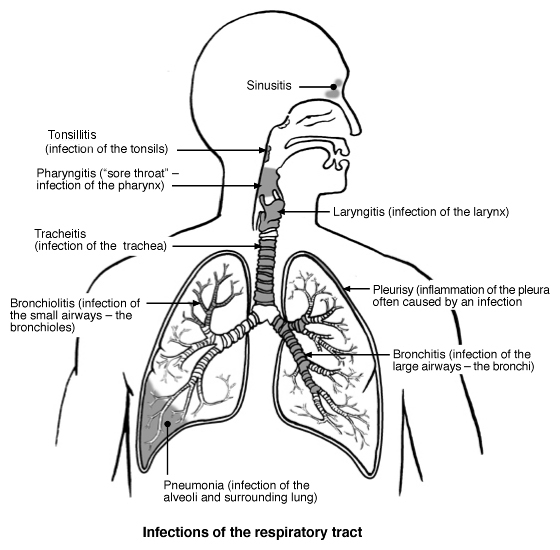
The diagram above shows the sites of a range of respiratory infections. This leaflet just deals with acute bronchitis. See the separate leaflets called Acute sinusitis, Tonsillitis, Sore throat, Laryngitis, Pleurisy, Bronchiolitis, and Pneumonia for the other types of infection shown in the diagram.
Note: chronic bronchitis is a separate illness and is not dealt with here. See the separate leaflet called Chronic obstructive pulmonary disease (COPD) for more details.
Is bronchitis contagious?
As with any infection, bronchitis is contagious and so it is important to cough into a tissue and wash your hands regularly to reduce the risk of passing it to others.
You are usually contagious with acute bronchitis for as long as your symptoms, particularly the cough, are present. Most cases are caused by viruses, and the highest risk of spreading the infection is during the first few days.
Acute bronchitis symptoms
Back to contentsThe main symptom of acute bronchitis is a cough. You may also develop:
General aches and pains.
Symptoms typically peak after 2-3 days and then gradually clear. However, it can take 2-3 weeks for the cough to go completely after the other symptoms have gone. This is because inflammation in the airways caused by the bronchitis infection may take some time to settle.
Emergency symptoms
Consult a doctor if any of the following occur:
If high temperature (fever), wheezing or headaches become worse or severe.
If you develop fast breathing, shortness of breath, or chest pains.
If you cough up blood or if your phlegm (sputum) becomes dark or rusty coloured.
If you become drowsy or confused.
If a cough persists for longer than 3-4 weeks.
If you have repeated (recurring) bouts of acute bronchitis.
If any other symptom develops that you are concerned about.
Continue reading below
Diagnosing acute bronchitis
Back to contentsYour doctor will listen to the history and examine you - this is usually enough to make a diagnosis and tests are rarely needed. If further tests are needed, they could include blood tests, a chest X-ray or sending a sample of sputum to the laboratory for analysis.
Acute bronchitis treatment
Back to contentsA main aim of treatment is to ease symptoms whilst your immune system clears the infection. The most useful treatments are:
Taking pain relievers such as paracetamol, ibuprofen, or aspirin to reduce high temperature (fever) and to ease any aches, pains and headaches. (Children aged under 16 years should not take aspirin.)
Having lots to drink if you have a fever, to prevent mild lack of fluid in the body (dehydration).
If you smoke, trying to stop for good. Bronchitis, chest infections and serious lung diseases are more common in smokers.
Taking plenty of rest.
What about cold and cough remedies?
You can buy many other 'cold and cough remedies' at pharmacies. There is little evidence of any impact on the infection but they may be useful for certain symptoms. For example, a decongestant nasal spray may help to clear a blocked nose.
Remember, cold and cough remedies often contain several ingredients. Some may make you drowsy. This may be welcome at bedtime if you have difficulty sleeping with a bronchitis. However, do not drive if you are drowsy. Some contain paracetamol, so be careful not to take more than the maximum safe dose of paracetamol if you are already taking paracetamol tablets. Always follow the advice of your pharmacist about which medicines can be used for children of different ages.
What about antibiotics?
The National Institute for Health and Care Excellence (NICE) has confirmed that otherwise healthy people who have acute bronchitis should not be prescribed antibiotics. Your immune system can usually clear the infection. Antibiotics do not kill viruses. Even if a germ (bacterium) is the cause, antibiotics usually do little to speed up recovery of an acute bronchitis. Antibiotics may even make symptoms worse, as some people develop side-effects such as loose or watery stools (diarrhoea), feeling sick (nausea) and rashes.
NICE recommends that your doctor should consider either an immediate prescription for antibiotics or a 'delayed prescription' (to be taken if symptoms do not improve or get worse) for the following people:
Over-80s who have been in hospital in the preceding year, are taking steroids, have diabetes or have heart failure.
Over-65s who have two of the risk factors in the line above.
People with long-term kidney, liver, heart, lung or nervous system conditions.
People with cystic fibrosis.
People with conditions which can stop their immune system from working properly.
NICE does not recommend prescribing bronchodilators (to open up the airways) or steroids in either inhaled or tablet form.
It recommends that you should consult your doctor if your symptoms have not settled within 3-4 weeks, or if your symptoms get rapidly worse or you become very unwell in yourself.
Antibiotics may also be prescribed if a complication develops such as pneumonia - but this is unlikely to occur if you are otherwise healthy.
Continue reading below
Preventing acute bronchitis
Back to contentsWashing your hands regularly is important to reduce the risk of catching bronchitis or other respiratory tract infections from those around you who may have them. Smoking causes lung problems such as COPD which predispose to bronchitis and so stopping smoking may help to reduce the risk of catching bronchitis.
Frequently asked questions
Back to contentsCan bronchitis go away on its own?
Most acute bronchitis cases improve on their own within a few weeks. Rest, fluids, and avoiding irritants can help, but see a doctor if symptoms worsen or persist.
How long does acute bronchitis last?
Acute bronchitis usually clears without complications within 3-4 weeks. Occasionally, the infection travels to the lung tissue to cause pneumonia.
What’s the difference between bronchitis and pneumonia?
Bronchitis and pneumonia are both infections of the lungs, but they affect different parts. Bronchitis affects the airways, whilst pneumonia infects the lung air sacs and causes more severe symptoms, often needing immediate medical care.
Is menthol vapour rub good for acute bronchitis?
Menthol vapour rub may ease symptoms of bronchitis, such as a blocked nose or chest congestion, by creating a cooling effect, but it does not treat the infection. You should always use it as instructed and do not apply it to babies or young children.
Can children get acute bronchitis?
Children are more likely to get bronchiolitis (an infection of the smaller parts of the respiratory tree) than bronchitis.
Patient picks for Chest and lung infections

Chest and lungs
Tuberculosis
Tuberculosis (TB) is an infection with a germ (bacterium) called Mycobacterium tuberculosis. If you have symptoms, or a doctor can find signs of the infection when examining you, this is known as active tuberculosis. If you have TB infection without any signs or symptoms, this is known as latent TB.
by Dr Colin Tidy, MRCGP
Chest and lungs
Pneumonia
Pneumonia is a lung infection that causes inflammation and swelling in the air sacs (alveoli). These sacs can fill with fluid, making it harder to breathe and for oxygen to reach the bloodstream. It's usually caused by bacterial infections but can also be caused by viral infections, and sometimes fungi. This leaflet explains the types, causes, symptoms, treatment, and prevention of pneumonia.
by Dr Mohammad Sharif Razai, MRCGP
Further reading and references
- Cough (acute): antimicrobial prescribing; NICE Guidance (February 2019)
- Singh A, Avula A, Zahn E; Acute Bronchitis
- Chest infections - adult; NICE CKS, May 2024 (UK access only)
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Jan 2028
18 Jan 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.