Ankle injury
Sprained or broken ankle
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 14 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Sports injuriesHamstring injuryGroin strainSprains and strainsKnee ligament injuriesMeniscal tears
The ankle is a complicated joint and it is commonly injured. Almost half of injuries are as a result of playing sports or exercising. A sprained ankle is the most common sports injury.
In this article:
Video picks for Sports injuries
What causes ankle pain?
To read more about different types of sports injuries, see the separate leaflet called Sports injuries.
To find out more about sprains, see the separate leaflet called Sprains and strains.
A sprain is an injury to the band of tissue that connects two or more bones to a joint. This band is called a ligament. A sprain is usually caused by the joint being forced suddenly outside its usual range of movement. Most sprains heal within a few weeks. A severe sprain may look and feel like a fracture, and it can be difficult for health professionals to tell the difference between the two. A sprained ankle is the most common sports injury.
A fracture is a break in a bone. A broken ankle means one of the bones which make up the ankle joint has broken. These are the leg bones (the tibia and fibula) and the hindfoot bones (the calcaneus and talus). Depending upon the exact cause of the fracture, one or more ankle bones may be involved. Fractures cause sudden pain and usually cause significant swelling. Stress fractures are smaller cracks in the bone which also cause intense pain but with less dramatic swelling.
This leaflet considers ankle sprains and ankle fractures. Ankle pain may arise from many other conditions, including arthritis, gout or Achilles tendinopathy. You can read more about these in the separate leaflets called Arthritis, Gout and Achilles tendinopathy.
Continue reading below
Anatomy of the ankle
As you can see from the picture below, showing bones and ligaments of the ankle, it is a complicated joint. The top illustration shows the foot and ankle looking from the inner side (medial). The bottom illustration shows the foot and ankle looking from the outer side (lateral).
Joints of the ankle and foot
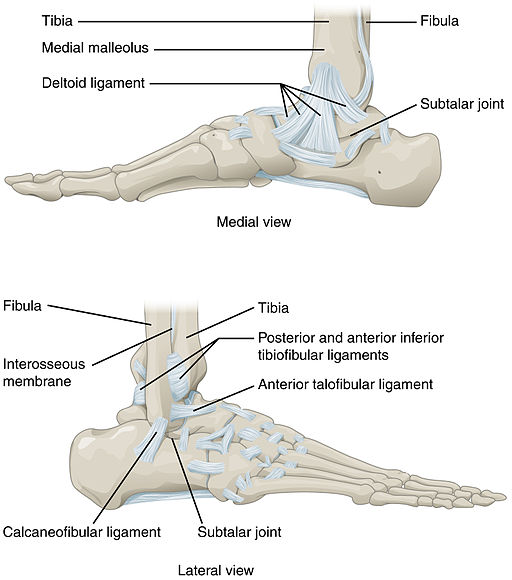
© OpenStax College,Anatomy & Physiology, Connexions Website, Jun 19, 2013, via Wikimedia Commons
What is a sprain?
Back to contentsA sprain is an injury to a ligament. Ligaments are strong band-like structures around joints, which attach bones together and give support to joints. A ligament can be injured, usually by being over-stretched. Some of the fibres of the ligament will then tear.
A damaged ankle ligament causes inflammation, swelling, and bleeding (which shows as bruising) around the affected joint. Moving the joint is painful. The picture below shows a badly sprained ankle with lots of bruising.
Ankle sprain
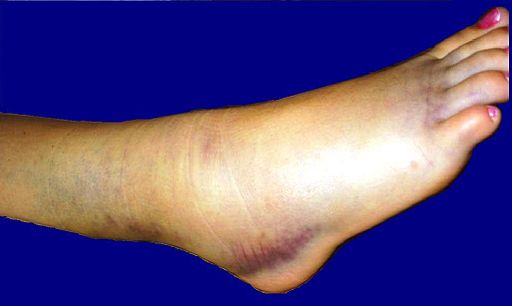
© Harrygouvas, CC BY-SA 3.0, via Wikimedia Commons
The severity of a sprain is graded according to how badly the ligament has been damaged and whether or not the ankle joint has been made unstable. The joint can become unstable when the damaged ligament is no longer able to give it the normal support:
Grade I - mild stretching of the ligament without joint instability.
Grade II - partial tear (rupture) of the ligament but without joint instability (or with mild instability).
Grade III - a severe sprain: complete rupture of the ligament with instability of the joint.
Lateral ankle sprain
The most common ligaments to damage when you sprain your ankle are the ones on the outer side of the ankle joint (a lateral sprain): the anterior talo-fibular ligament and the calcaneo-fibular ligament (lateral ligaments).
The lateral ligaments can stretch and be sprained when you 'go over' on your ankle and your foot turns inwards under you and points downwards.
Sometimes you can break a small bit of bone off the very end of the fibula (where the ligaments are attached) at the same time. This and other types of ankle fractures are discussed below.
High ankle (syndesmotic) sprain
It is much less common to damage the ligaments that attach across the ankle on the inner (medial) side of the foot: for every 10 people who have a lateral ankle sprain, one or two will have a high ankle sprain.
This is partly because of the shape of the bones and partly because the band that goes across the inner side of the ankle joint (deltoid ligament) is much stronger than the ligaments on the other side of the ankle joint.
A high ankle sprain (a syndesmotic sprain) is one in which the ligaments above the ankle joint are stretched or torn. These ligaments link the two bones of the lower leg (tibia and fibula).
It is particularly common in sports such as football and hockey and also in skiing injuries. Typically the foot has been twisted forcefully away from the lower leg.
A high ankle sprain takes twice as long to heal compared to a lateral ankle sprain.
A high ankle sprain may be suspected if you feel that your ankle isn't stable and you are having difficulty walking, not just because of pain. Usually, the damaged ligament heals by itself over time. Some scar tissue may be produced where there has been a tearing of tissues.
Continue reading below
What is the treatment for a sprained ankle?
Back to contentsUsually, the damaged ligament heals by itself over time. Some scar tissue may be produced where there has been a tearing of tissues.
The initial treatment is described as PRICE (Protect, Rest, Ice, Compression, and Elevation), together with avoiding HARM (Heat, Alcohol, Running, and Massage).
This treatment must be balanced fairly early with early controlled weight bearing and ensuring as normal a gait pattern as possible. This assists in retaining the power and balance of the muscles of the legs and in maintaining a healthy posture. Painkillers may be needed.
For the first 48-72 hours think of:
Paying the PRICE
Protect from further injury:
For example, by using a tubular bandage and/or an ankle support or a boot with high sides
Rest the ankle joint:
For the first two or three days following injury, consider the use of crutches when wanting to be mobile.
It is important that the ankle is not rested for too long as this may delay recovery.
In most cases, early controlled weight bearing with the ankle well supported is preferable to complete rest.
Ice can be applied soon after injury:
The cold is thought to reduce blood flow to the damaged ligament. This may limit pain, inflammation and bruising.
Applying ice packs used to be common advice for soon after an injury but it is not known how effective it is. Some scientists think it may actually delay healing.
If used, apply for 15-20 minutes every 2-3 hours during the day, for the first 2-3 days.
Make an ice pack by wrapping ice cubes in a plastic bag or towel, or by using a bag of frozen peas. Do not put ice directly next to skin, as it may cause ice burn. Gently press the ice pack on to the area of your ankle that hurts.
Do not leave ice on while asleep.
Compression with a bandage:
This will limit swelling and will help to rest the joint.
A tubular compression bandage or an elastic bandage can be used.
The bandage should not be too tight - mild pressure that is not uncomfortable and does not stop blood flow is the aim.
A pharmacist will advise on the correct size.
Remove the bandage before going to sleep.
You may be advised to remove the bandage for good after 48 hours, so that the joint can move.
Elevation:
This aims to limit and reduce any swelling. For example, keep the foot up on a chair to at least hip level when you are sitting. (It may be easier to lie on a sofa and to put your foot on some cushions.) When you are in bed, put your foot on a pillow.
Avoid HARM for 72 hours after injury
That is, avoid:
Heat - for example, hot baths, saunas, heat packs. Heat encourages blood flow which will tend to increase bruising and inflammation. So, heat should be avoided when inflammation is developing. However, after about 72 hours, no further inflammation is likely to develop and heat can then be soothing.
Alcohol, which can increase bleeding and swelling and decrease healing.
Running, or any other exercise which may cause further damage.
Massage, which may increase bleeding and swelling. However, after 72 hours, gentle massage may be soothing.
Other treatments
Your healthcare professional will advise. The advice may typically include:
Do not stop moving the joint. Don't do anything that causes much pain, but gently get the joint moving again. The aim is to get the ankle joint moving in normal directions, and to prevent it becoming stiff.
Consider wearing an ankle support until symptoms have gone. There are various forms of ankle supports which can be used - from an elasticated bandage to a specialised brace. The aim is to give some support to the joint whilst the damaged ligament is healing, but to allow the ankle to move to a reasonable degree.
Physiotherapy may help for more severe sprains, or if symptoms are not settling. A physiotherapist can advise on exercises:
To get the ankle joint back to a full range of normal movement.
To improve the strength of the surrounding muscles. The stronger the muscles, the less likely it is that a sprain will happen again.
To improving proprioception. This means the ability of your brain to sense the position and movement of your joints. Good proprioception helps you to make immediate, unconscious minor adjustments to the way you walk when walking over uneven ground. This helps to prevent further sprains, and is achieved through special exercises, such as balancing on one leg and balancing on a wobble board or slider board.
You are unlikely to be able to play sport or do vigorous exercise involving the ankle for at least 3-4 weeks after a sprain but it will depend on:
The severity of the sprain.
How painful it is.
How likely you are to re-injure it.
Treatment of severe sprains
Extra treatment may be needed for some types of ankle sprain:
Severe sprains (where the ligaments are badly torn (ruptured) or the joint is unstable).
A high ankle sprain, where the ligament above the ankle joint is torn, making the joint unstable.
There is some evidence that these types of sprain may heal more quickly if treated with a short period of immobilisation. This means wearing a brace or a plaster cast on the lower leg and ankle for about 10 days (longer for a syndesmotic sprain).
In some cases, if ligaments are very badly torn or the joint is too unstable, surgery may be advised. Your doctor will assess if this is necessary (but it is not needed in most cases).
If the sprained ankle is still very painful six weeks after the original injury, you may be advised to have additional tests on the joint, such as a further X-ray or scan. Sometimes there are torn ligaments or small breaks (fractures) which do not show up when the injury first happens. The ankle may initially have been very swollen and small additional points of damage might have been difficult to detect.
You may not need any medication if the sprain is mild and you can tolerate the pain. If needed, paracetamol is the safest painkiller to use, particularly in the first few days. You can read about other painkiller options in the separate leaflet called Sprains and strains.
When should I see a doctor?
Back to contentsYou should see a doctor if there is any concern about the injury, or if the injury is severe. In particular, see a doctor if:
You suspect a bone may be broken or a ligament is ruptured.
You have a lot of tenderness over a bone.
The leg or joint looks out of shape (deformed) rather than just swollen. This may mean there is a break (fracture) or dislocation which needs urgent treatment.
There is loss of circulation in the foot (a numb, cold foot with pale or bluish skin). If this occurs, treatment is urgent.
The pain is severe.
You cannot walk or bear weight because of the injury.
Bruising is severe.
The joint does not seem to work properly or feels unstable after the pain and swelling have gone down. This may be a sign of an additional injury such as a torn tendon or a syndesmotic sprain.
Symptoms and swelling do not gradually settle. Most sprains improve after a few days, although the pain often takes several weeks to go completely, especially when you use the injured joint.
Continue reading below
What is an ankle fracture/broken ankle?
Back to contentsAn ankle fracture (or a broken ankle) is a break to one of the bones that make up the ankle joint. These are the tibia and fibula in the leg, the calcaneus in the heel and the talus in the front part of the ankle.
Types of fractures
Fractures may in general be:
Open or closed: an open fracture is one where the skin is broken over the fracture so that there is a route of possible infection from the outside into the broken bones. This is obviously a more serious type of fracture, with damage to the soft tissues around the ankle, making treatment and healing more complicated, and it needs specialist assessment.
Displaced or not displaced: a displaced fracture is one where, following the break, the bones have slipped out of line. A displaced fracture also needs specialist care, as the bones will need to be properly lined up and stabilised. This may involve an anaesthetic and some kind of metal pinning or plating to the bones.
Types of ankle fracture
Back to contentsAnkle fracture types
Back to contentsThere are many types of ankle fracture, depending on which bones (or combination of bones and ligaments) are damaged. Doctors classify ankle breaks (fractures) in various ways. Some classifications are based on whether the line of breakage (fracture) of the bone or bones runs through the ankle joint, just above it or just below it. Other classifications are based on particular patterns of breakage which are seen after particular types of injury.
Pott's fracture
This involves both the tibia and fibula leg bones (bimalleolar fractures). These fractures are unstable and require urgent treatment.
Weber fracture
Weber fracture is a fracture of the end of the fibula (lateral malleolus). They are classified as either:
A - the fracture is below the syndesmosis.
B - the fracture is at the level of the syndesmosis (most common).
C - the fracture is above the syndesmosis.
Maisonneuve fracture
Maisonneuve fracture is a fracture of the fibula often in combination with either a syndesmotic sprain or other fracture of the ankle.
Pilon fracture
A pilon fracture is a fracture of the very end of the tibia and top of the talus forefoot bone. The talus is 'driven' into the tibia as may happen in a fall from a height or a foot braced against the floor of a car in a collision.
Snowboarder's fracture
Snowboarder's fracture is a fracture of the outer side of the talus, produced by forced turning down and inwards of the foot at the ankle.
Stress fracture
A stress fracture is a small crack in a bone. Stress fractures often develop from overuse, such as from high-impact sports like distance running - the repeated stress of the foot striking the ground can cause problems. Stress fractures differ from other ankle fractures in that they result from overuse rather than sudden trauma. The cracks are small (although they may be multiple) so that, although they are painful, the swelling may be only slight. In the ankle, the heel (calcaneus) and the lower leg (fibula) are most commonly affected.
Broken ankle signs and symptoms
Back to contentsAn ankle break (fracture) and a severe sprain may feel (and look) very similar. Both cause sudden pain, swelling and loss of weight bearing. Sprains vary in severity and may not always affect the ankle to this degree. Fractures (apart from stress fracture) are almost always severe enough to cause the following symptoms:
Fractures cause sudden pain, and they can be very painful. People who have broken a bone stop what they are doing. They are unlikely to be able to continue running, jumping or walking.
Swelling is a feature of broken bones, because they bleed. Bones have a rich blood supply so when broken they bleed into the surrounding tissues. This happens immediately, so the swelling from a broken ankle appears fast, with the ankle usually looking significantly swollen within the first thirty minutes.
Bruising results as the swelling is caused by blood. It may not be immediately 'bruise-coloured' as it can take a while for the bruising to track through to the skin and be visible.
Inability to weight bear: being able to take the body weight on to the injured foot is usually impossible or very painful in ankle fracture. An exception to this would be stress fracture, when impact is likely to be painful but may still be tolerable.
Bony tenderness is seen in ankle fracture. There are particular points of tenderness which doctors look for under and around the ankle and forefoot (see diagram below). Most ankle fractures will cause tenderness in one of these areas. This is less often the case in bad sprains, so it can be a good way of determining which injuries need an X-ray.
Deformity: if the ankle looks odd or misshapen, not just by bruising but because the foot looks twisted or out of place, a displaced fracture is likely. This is an extremely serious condition, as when bones slip out of place nerves and blood vessels may become trapped. It's important that the fracture be assessed urgently.
Diagnosing a broken ankle
Back to contentsIt can be very difficult to tell a severe sprain from a break (fracture) of the ankle.
Ankle fractures need an X-ray test for diagnosis, for management and in order for you to know what to expect in terms of recovery. Sprains do not need X-ray, and doctors prefer to avoid unnecessary X-rays in order to keep your lifetime exposure to radiation as low as possible.
Ottawa Rules
These are a set of rules devised by doctors to determine which ankle injuries should be X-rayed to look for fracture. They centre on whether there is bony tenderness at certain points around the ankle. If there is no bony tenderness in any of these points AND you are able to weight bear (both in casualty when seen and immediately after the injury) then fracture is unlikely and you will not need to be X-rayed. If, however, any of those features ARE present then an X-ray will be offered in order to detect or rule out fracture.
Broken ankle treatment
Back to contentsAs with all breaks (fractures), the aim is to promote healing and restore function.
If your fracture is displaced you will need surgical management (reduction of the fracture to re-align the bones). This is likely to be done under anaesthetic, and the bones may need some form of temporary of permanent fixation to hold them in line.
If your fracture is open then you may need surgical treatment to clean your wound and repair the soft tissue damage, in addition to having the ankle fracture assessed.
If neither of these applies (ie you have a closed, non-displaced fracture) then treatment of the fracture involves:
Stabilisation - initially with a 'backslab' cast which is open on one side to allow for continuing swelling.
Elevation - keeping the ankle raised will reduce swelling, which in turn improves healing.
A well-moulded cast for 4-6 weeks - after this, weight bearing can be resumed.
Some stable fractures are treated with a brace rather than a cast.
Serial X-rays may be offered to make sure healing is taking place.
Ankle fracture surgery
Surgical treatment involving open reduction and internal fixation is considered for:
Displaced fractures.
Fractures which doctors think may be unstable (ie they are at risk of displacing).
Some fractures which run through the joint and damage the ligaments which hold it together. These are called syndesmotic fractures and may need surgical repair.
What are the complications of a broken ankle?
Most ankle breaks (fractures) heal uneventfully. Possible early complications include:
Infection (especially after open fracture).
Damage to nerves and blood vessels (especially after displaced fracture).
Compartment syndrome (severe swelling in the leg soon after the injury, putting pressure on nerves and blood vessels).
Poor healing.
Damage to skin and soft tissues by a tight or poorly finished cast.
Burns to the skin as the plaster hardens.
Failure of bones to knit together and heal well. This can lead to delayed union, union with poor alignment, or complete non-union even after six months.
Temporary complications of wearing a cast include thinning of the bones and wasting of the muscles, both of which occur significantly even in a 4-6 week period of casting.
Inflammation of the veins of the lower leg (thrombophlebitis).
Clotting (thrombosis) of the deep veins of the leg (deep vein thrombosis) which can relate both to reduced mobility and to pressure on the leg veins from swelling and casting.
Complications of surgical treatment of ankle fracture can include pain from, and infection around, surgical pins (which can in themselves be distressing and frightening).
Possible later complications include:
Osteoarthritis of the ankle.
Stiffness and loss of flexibility in the ankle (less.
Long-term instability of the ankle joint, needing later correction.
Complex regional pain syndrome (also called Sudeck's atrophy or algodystrophy) - a nerve abnormality which can develop after fracture and which leads to continuous burning pain and gradual loss of strength. Treatment is prolonged and difficult.
In children, damage to the growing parts of the bones of the ankle can affect overall growth
Painkiller options in ankle fracture are the same as for ankle sprain, above. However, rub-on (topical) treatments will not be possible if you are wearing a cast or have damage to the skin and soft tissues around the ankle.
How do I get back to full function after ankle fracture?
Back to contentsA period of immobilisation has lasting effects on the bones and muscles around your ankle. Therefore, both before and after the cast comes off, it is important to work towards full recovery. This may involve physiotherapy, graded exercise and sometimes use of protective ankle supports or of crutches. It is important to take the advice of your doctor or physiotherapist before using an ankle support in the long term. Whilst a support may stabilise the ankle, the best stabilisation for your ankle is the development of its own strong and supportive muscles and developing excellent proprioception.
Preventing sprains and fractures
Back to contentsResearch shows that if you have had a sprained ankle while playing sport or exercising, you are twice as likely to sprain that ankle again in the following year.
Proprioceptive training
Proprioception is the ability of your brain to sense the position and movement of your joints. Improving this sense has been shown to be the most effective way to prevent a repeat ankle injury in athletes. It is not clear whether proprioceptive training can also reduce the risk of a first ankle injury. A physiotherapist can advise on exercises to improve proprioception.
Examples of proprioceptive training include:
Balancing on a wobble board or ankle disc.
Throwing and catching a ball while standing on one leg.
Balancing on one leg with eyes closed.
Other preventative factors
To reduce the risk of ankle injury consider:
Exercises to build up the muscle strength around the ankle.
Wearing boots that give ankle support when hiking across country or rambling over hills and uneven ground.
Avoiding falls where possible:
Clear paths of ice and snow.
Avoid getting drunk.
Take extra care if on medication that causes drowsiness.
Keep stairways free of clutter.
Ensure rugs and carpets can't slip.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Sports injuries

Bones, joints and muscles
Sports injuries
Regular exercise has many benefits for your body. However, exercise does come with risks. Most people only experience minor sports-related injuries such as strained muscles and blisters. A few will experience more serious injuries such as torn cartilages or even broken bones. This leaflet describes some of the more common sports injuries, how to recognise them and how to avoid them.
by Dr Colin Tidy, MRCGP

Bones, joints and muscles
Meniscal tears
You've all seen the footballer on TV - one moment they're running full pelt, the next they've tripped over another player and are clutching their knee in agony. There's a good chance an injury to their knee cartilage is at least part of the problem.
by Dr Colin Tidy, MRCGP
Further reading and references
- Sprains and strains; NICE CKS, September 2020 (UK access only)
- Ruiz-Sanchez FJ, Ruiz-Munoz M, Martin-Martin J, et al; Management and treatment of ankle sprain according to clinical practice guidelines: A PRISMA systematic review. Medicine (Baltimore). 2022 Oct 21;101(42):e31087. doi: 10.1097/MD.0000000000031087.
- Wagemans J, Bleakley C, Taeymans J, et al; Exercise-based rehabilitation reduces reinjury following acute lateral ankle sprain: A systematic review update with meta-analysis. PLoS One. 2022 Feb 8;17(2):e0262023. doi: 10.1371/journal.pone.0262023. eCollection 2022.
- Wire J, Hermena S, Slane VH; Ankle Fractures.
- Goost H, Wimmer MD, Barg A, et al; Fractures of the ankle joint: investigation and treatment options. Dtsch Arztebl Int. 2014 May 23;111(21):377-88. doi: 10.3238/arztebl.2014.0377.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 Oct 2027
14 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.