Childhood leukaemias
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 30 Nov 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Leukaemia is a cancer of the cells which develop into blood cells. There are different types of leukaemia. Most children with leukaemia will have acute lymphoblastic leukaemia. Some will have acute myeloid leukaemia. The outlook (prognosis) for children with leukaemia is usually very good and most children are cured. This leaflet gives a general overview of childhood leukaemias.
In this article:
Video picks for Children's cancers
Continue reading below
What is leukaemia?
Leukaemia is a cancer of cells in the bone marrow (the cells which develop into blood cells).
Cancer is a disease of the cells in the body. There are many types of cancer which arise from different types of cell. What all cancers have in common is that the cancer cells are abnormal and do not respond to normal control mechanisms. Large numbers of cancer cells build up because they multiply 'out of control', or because they live much longer than normal cells, or both.
With leukaemia, the cancerous (malignant) cells in the bone marrow spill out into the bloodstream. There are several types of leukaemia. Most types arise from cells which normally develop into white blood cells. (The word leukaemia comes from a Greek word which means 'white blood'.)
Childhood leukaemia
Back to contentsIt is very important to know which type of leukaemia a child has. This is because the outlook (prognosis) and treatments vary for the different types. Before discussing the different types of leukaemia it may help to know some basics about normal blood cells and how they are made.
Continue reading below
What is normal blood made up of?
Back to contentsBlood cells
These can be seen under a microscope and make up about 40% of the blood's volume. Blood cells are divided into three main types:
Red cells (erythrocytes). These make blood a red colour. One drop of blood contains about five million red cells. Red cells contain a chemical called haemoglobin. This binds to oxygen and takes oxygen from the lungs to all parts of the body.
White cells (leukocytes). There are different types of white cells, which are called neutrophils (polymorphs), lymphocytes, eosinophils, monocytes and basophils. They are part of the immune system. Their main role is to defend the body against infection.
Platelets. These are tiny and help the blood to clot if we cut ourselves.
Plasma
This is the liquid part of blood and makes up about 60% of the blood's volume. Plasma is mainly made from water. However, it contains many different proteins and other chemicals, such as hormones, antibodies, enzymes, glucose, fat particles, salts, etc.
When blood spills from your body (or a blood sample is taken into a plain glass tube) the cells and certain plasma proteins clump together to form a clot. The remaining clear fluid is called serum.
The bone marrow, stem cells and blood cell production
Back to contentsBone marrow
Blood cells are made in the bone marrow by 'stem' cells. The bone marrow is the soft 'spongy' material in the centre of bones. The large flat bones, such as the pelvis and breastbone (sternum), contain the most bone marrow. To make blood cells constantly you need a healthy bone marrow. You also need nutrients from your diet, including iron and certain vitamins.
Stem cells
Stem cells are immature (primitive) cells. There are two main types in the bone marrow - myeloid and lymphoid stem cells. These derive from even more primitive common 'pluripotential' stem cells. Stem cells constantly divide and produce new cells. Some new cells remain as stem cells; others go through a series of maturing stages ('precursor' or 'blast' cells) before forming into mature blood cells. Mature blood cells are released from the bone marrow into the bloodstream.
Haematopoietic System of the Bone Marrow
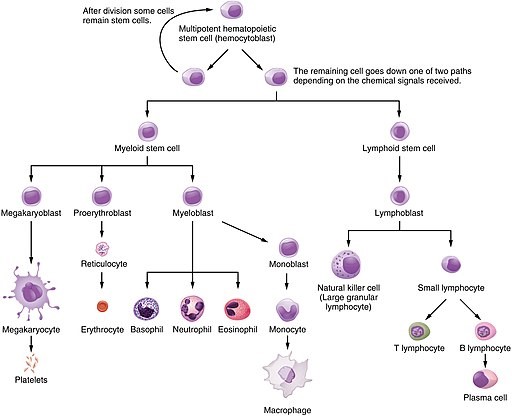
© JulieJenksButteCollege, CC BY-SA 4.0, via Wikimedia Commons
Lymphocyte white blood cells develop from lymphoid stem cells. There are three types of mature lymphocytes:
B lymphocytes make antibodies which attack infecting germs (bacteria, viruses, etc).
T lymphocytes help the B lymphocytes to make antibodies.
Natural killer cells, which also help to protect against infection.
All the other different blood cells (red blood cells, platelets, neutrophils, basophils, eosinophils and monocytes) develop from myeloid stem cells.
Blood production
The body makes millions of blood cells every day. Each type of cell has an expected lifespan. For example, red blood cells normally last about 120 days. Some white blood cells last just hours or days - some last longer. Every day millions of blood cells die and are broken down at the end of their lifespan. There is normally a fine balance between the number of blood cells that you make and the number that die and are broken down. Various factors help to maintain this balance. For example, certain hormones in the bloodstream and chemicals in the bone marrow called 'growth factors' help to regulate the number of blood cells that are made.
Continue reading below
What causes leukaemia?
Back to contentsLeukaemia is thought to start first from one abnormal cell. What seems to happen is that certain vital genes which control how cells divide, multiply and die, are damaged or altered. This makes the cell abnormal. If the abnormal cell survives it may multiply 'out of control' or survive a long time, and develop into a leukaemia.
In most cases of leukaemia, the reason why a cell becomes abnormal is not known. There are certain 'risk factors' which increase the chance that certain leukaemias will develop. However, these only account for a small number of cases. Risk factors for some types of leukaemia include:
High levels of radiation - for example, previous radiotherapy for another condition.
Past treatment with chemotherapy or other medicines that weaken the immune system.
Certain inherited (genetic) disorders, the most common is Down's syndrome.
Exposure to certain chemicals such as benzene.
What are the main types of leukaemia?
Back to contentsThe main types of leukaemia that occur in childhood are:
Chronic myeloid leukaemia (CML) can occur in children but is much less common and chronic lymphocytic leukaemia (CLL) is very rare in childhood.
'Acute' means the disease develops and progresses quite quickly.
'Chronic' means persistent or ongoing. When talking about leukaemia, the word chronic also means that the disease develops and progresses slowly (even without treatment). Chronic leukaemias are much more common in adults than in children.
'Lymphoblastic' and 'lymphocytic' mean that an abnormal cancerous (malignant) cell is a cell that originated from a lymphoid stem cell.
'Myeloid' means that an abnormal cancerous cell is a cell that originated from a myeloid stem cell.
Acute lymphoblastic leukaemia (ALL)
In ALL the bone marrow makes large numbers of abnormal immature lymphocytes called lymphoblasts. There are various subtypes of ALL. For example, the abnormal lymphoblasts can be immature B or T lymphocytes. Typically, ALL develops quite quickly (acutely) and rapidly becomes worse (over a few weeks or so) unless treated. ALL can occur at any age but about 6 in 10 cases occur in children. It is the most common form of leukaemia to affect children (although it is an uncommon disease).
Acute myeloid leukaemia (AML)
In AML the bone marrow makes large numbers of abnormal immature white blood cells which are derived from a myeloid stem cell. The abnormal immature cells are called blasts. There are various subtypes of AML, depending on exactly what cell type becomes cancerous and at what stage in the maturing process. Typically, AML develops quite quickly and rapidly becomes worse (over a few weeks or so) unless treated. AML is an uncommon disease. Most cases occur in people over 50 years of age but AML can occur in children.
Chronic myeloid leukaemia (CML)
CML develops due to a problem with a stem cell in the bone marrow, which becomes abnormal. The abnormal stem cell multiplies. The cells that are made from the abnormal stem cells mature and develop into near-normal white cells - mainly neutrophils, basophils and eosinophils (collectively called granulocytes). Typically, CML develops and progresses slowly - over months or years, even without treatment. CML is the rarest of the four main types of leukaemia. It occurs mainly in adults, and becomes more common with increasing age. However, CML may also occur in children, although this is very rare.
See the separate leaflet called Leukaemia for information on leukaemia in adults.
How common is childhood leukaemia?
Back to contentsChildhood leukaemia is rare, but is still the most common cancer in children and teenagers. Leukaemia causes about 1 in every 3 childhood cancers.
About 3 out of 4 leukaemias in children and teenagers are ALL. Most of the remaining cases are AML.
ALL most often first presents in early childhood, most often between 2 and 4 years of age. AML can occur at any time but is slightly more common during the first two years of life and during the teenage years.
Chronic leukaemias are very rare in children. Most children with chronic leukaemia have CML, which more often affects teenagers than younger children.
There are other much less common causes of leukaemia in children that include:
Hybrid or mixed lineage leukaemias: the cancerous (malignant) cells have features of both ALL and AML. These leukaemias are usually treated like ALL and usually respond well to treatment.
Juvenile myelomonocytic leukaemia (JMML): this rare type of leukaemia is neither chronic nor acute. It most often occurs in children under the age of 4 years.
What are the main symptoms of leukaemia?
Back to contentsAs large numbers of abnormal blood cells are made, much of the bone marrow fills with these abnormal cells. Because of this it is difficult for normal cells in the bone marrow to survive and make enough normal mature blood cells. Also, the abnormal cells spill out into the bloodstream. Therefore, the main problems which can develop include:
Anaemia. This occurs as the number of red blood cells in the bloodstream goes down. This can cause tiredness, breathlessness and pale skin and lips.
Blood clotting problems. This is due to low levels of platelets in the bloodstream. This can cause easy bruising, bleeding from the gums and other bleeding-related problems.
Serious infections. The abnormal white blood cells do not protect against infection. Also, there is a reduced number of normal white blood cells which usually combat infection. Therefore, serious infections are more likely to develop. Depending on the type and site of infection which develops, the symptoms can vary greatly.
The time taken to develop these symptoms after the disease starts varies. Typically, it is within weeks for ALL or AML. It may take months or years for symptoms to develop with CLL or CML, as these leukaemias progress slowly.
The abnormal cells may also build up in lymph glands and in the spleen. This causes swollen lymph glands in various parts of the body and also an enlarged spleen.
Other symptoms which may develop include pain in the bones or joints (mainly with ALL), persistent raised temperature (fever) and weight loss.
How is childhood leukemia diagnosed?
Back to contentsA blood test
A blood test can often suggest the diagnosis of leukaemia, as abnormal cells are often detected in the blood test. Further tests are usually done to confirm the diagnosis.
A bone marrow sample
For this test, a small amount of bone marrow is removed by inserting a needle into the pelvic bone (or sometimes the breastbone (sternum)). Local anaesthetic is used to numb the area. A small sample of bone may also be taken. The samples are put under the microscope to look for abnormal cells and are also tested in other ways. This can confirm the diagnosis. (See the separate leaflet called Bone Marrow Biopsy and Aspiration for more detail.)
Cell and chromosome analysis
Detailed tests are often done on abnormal cells obtained from the bone marrow sample or blood test. These find out the exact type or subtype of the cell that is abnormal.
X-rays and scans
A chest X-ray, CT scan, MRI scans, ultrasound scan and bone scan may be used to look for any abnormal lymph nodes or other abnormalities in the chest, tummy (abdomen), brain or bones.
Lumbar puncture
This test collects a small amount of fluid from around the spinal cord - cerebrospinal fluid (CSF). It is done by inserting a needle between the bones (vertebrae) in the lower (lumbar) region of the back. (See the separate leaflet called Lumbar Puncture (Spinal Tap) for more detail.) By examining the fluid for leukaemia cells, it helps to find out if the leukaemia has spread to the brain and spinal cord. This is mainly done when assessing ALL and sometimes AML.
What is the treatment for childhood leukaemia?
Back to contentsThe treatment advised depends on the exact type of leukaemia and the stage it is at. For example, ALL is usually treated as soon as possible with intensive chemotherapy. On the other hand, adults in the early stages of CLL may not need any treatment. This is because CLL often progresses very slowly and may not need treatment for several years.
For details of treatments for each type of leukaemia, see the separate leaflets called Acute Lymphoblastic Leukaemia (ALL), Acute Myeloid Leukaemia (AML) and Chronic Myeloid Leukaemia (CML).
What is the outlook for childhood leukaemia?
Back to contentsThe outlook varies for each of the different leukaemias. However, the overall outlook may be better than many people imagine. With acute leukaemias, children who are free of the disease after five years are very likely to have been cured. This is because it is very rare for these cancers to return after this long.
For example, the outlook for ALL has greatly improved over the period of 20 years or so. More than 90 out of every 100 children treated for ALL will live for at least five years after treatment and most children are completely cured.
The outlook for children with AML has also improved and between 6 and 7 out of every 10 children treated for AML will live for at least five years after treatment.
However, children who have been cured of leukaemia may have some physical and psychological problems in later life. The physical problems may include reduced height, being overweight, reduced bone strength (osteoporosis) or infertility when they become adults.
The treatment of cancer and childhood leukaemia is a developing area of medicine. New treatments continue to be developed and the information on outlook above is very general. There are some newer medicines that have been introduced in the last few years that show promise to further improve the outlook.
Patient picks for Children's cancers

Cancer
Children's cancers
Childhood cancer is rare and is much less common than cancer in adults. There are many different type of cancer that can affect children and childhood cancers can cause many different symptoms. Therefore, any child should be seen by a GP or other healthcare professional if you are concerned about any unexplained symptoms. The treatments and outcome (prognosis) for childhood cancers are improving all the time. Most children who are diagnosed with cancer will be cured.
by Dr Colin Tidy, MRCGP

Cancer
Retinoblastoma
Retinoblastoma is an uncommon cancer of the eye which occurs in children under the age of 5. This leaflet describes retinoblastoma. It discusses the symptoms and signs of retinoblastoma and the management options children with retinoblastoma may be offered.
by Dr Mary Elisabeth Lowth, FRCGP
Further reading and references
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
- Brivio E, Baruchel A, Beishuizen A, et al; Targeted inhibitors and antibody immunotherapies: Novel therapies for paediatric leukaemia and lymphoma. Eur J Cancer. 2022 Mar;164:1-17. doi: 10.1016/j.ejca.2021.12.029. Epub 2022 Feb 1.
- Chennamadhavuni A, Lyengar V, Shimanovsky A; Leukemia
- Inaba H, Mullighan CG; Pediatric acute lymphoblastic leukemia. Haematologica. 2020 Nov 1;105(11):2524-2539. doi: 10.3324/haematol.2020.247031.
- Bispo JAB, Pinheiro PS, Kobetz EK; Epidemiology and Etiology of Leukemia and Lymphoma. Cold Spring Harb Perspect Med. 2020 Jun 1;10(6). pii: cshperspect.a034819. doi: 10.1101/cshperspect.a034819.
Continue reading below
About the author

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Nov 2027
30 Nov 2022 | Latest version
13 Sept 2016 | Originally published
Authored by:
Dr Colin Tidy, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.