Housemaid's knee
Prepatellar bursitis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 9 Sept 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Housemaid's knee is also known as prepatellar bursitis. It is caused by inflammation of a small fluid-filled sac (the bursa) in front of the kneecap. It more commonly occurs in people who spend long periods of time kneeling. Treatment is usually supportive and the outlook is generally very good.
At a glance
Housemaid's knee is inflammation of the fluid-filled sac (bursa) in front of your kneecap.
It causes knee pain, swelling, redness, and difficulty bending your knee or kneeling.
Causes include injury, repeated kneeling, infection, or other inflammatory diseases.
Diagnosis is usually by examining your knee, but fluid may be tested for infection.
Treatment for non-infected cases can include rest, ice, knee pads, or anti-inflammatory medicines.
Infected cases are treated with antibiotics, and sometimes drainage of the fluid.
Using knee pads for jobs or hobbies involving kneeling can help prevent it.
In this article:
Video picks for Knee pain
Continue reading below
What is housemaid's knee?
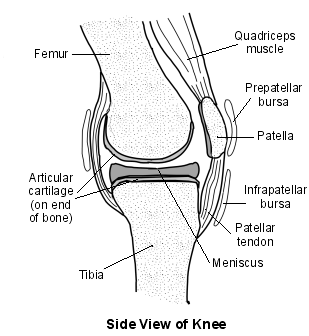
There are four bursae around the knee joint. They are all prone to inflammation, or bursitis. However, the bursa in between the skin and the kneecap (the prepatellar bursa) is most commonly affected. The prepatellar bursa is located as shown in the diagram. Housemaid's knee is the name given to inflammation of the prepatellar bursa, hence, prepatellar bursitis.
Housemaid's knee
What is bursitis?
Back to contentsBursitis means inflammation within a bursa. A bursa is a small sac of fluid with a thin lining. There are a number of bursae in the body. Bursae are normally found around joints and in places where ligaments and tendons pass over bones. They can also be found in other places with high levels of pressure or friction.
Generally, the function of a bursa is to help reduce friction and allow maximal range of motion around joints. When there is inflammation within a bursa (bursitis), the bursa swells due to an increase in the amount of fluid within the bursa sac.
Continue reading below
What causes housemaid's knee?
Back to contentsThere are a number of different things that can cause housemaid's knee (prepatellar bursitis):
A sudden, one-off injury to the knee
This might be, for example, a fall or direct blow on to the knee.
Recurrent minor injury to the knee
This usually happens after spending long periods of time kneeling down, putting pressure on the kneecap (patella). Historically, this was typical of housemaids spending long periods of time on their knees scrubbing floors, or any other job or pastime that requires frequent kneeling; hence, the term housemaid's knee.
Infection
The fluid in the prepatellar bursa sac can become infected and cause inflammation within a bursa (bursitis). This is known as septic prepatellar bursitis. It is particularly common in children with housemaid's knee. This usually follows a cut, scratch or injury to the skin on the surface of the knee which allows germs (bacteria) to spread infection into the bursa.
Another inflammatory disease
If you already have an inflammatory disease such as rheumatoid arthritis, you have an increased risk of developing a bursitis. Rheumatoid arthritis is a form of arthritis that causes inflammation, pain and swelling of joints.
Gout
If you have gout or pseudogout you have an increased risk of developing a bursitis. Gout is caused by a build-up of uric acid crystals. Uric acid is a chemical in the blood that is usually harmless and passed out with the urine. In gout, it builds up and collects within a joint, causing pain, inflammation and joint swelling.
Housemaid's knee symptoms
Back to contentsThe symptoms of prepatellar bursitis include:
Knee pain and swelling of the affected area.
Redness of the skin over the knee.
A tender kneecap.
Difficulty bending the knee and difficulty kneeling and walking.
If housemaid's knee is caused by infection, you may have a high temperature (fever).
Continue reading below
How common is housemaid's knee?
Back to contentsAny age group can be affected by housemaid's knee (prepatellar bursitis). It is generally more common in males than in females. Housemaid's knee in children is more likely to be caused by infection.
Infection is also a common cause of housemaid's knee in people whose immune systems are not working well. Such people include those receiving steroid treatment or those on chemotherapy treatment for cancer.
Prepatellar bursitis is also more common in tradesmen who spend long periods of time kneeling - for example, carpet fitters, concrete finishers and roofers.
How is housemaid's knee diagnosed?
Back to contentsA doctor is usually able to diagnose housemaid's knee simply by examining your knee. They may ask you questions about your occupation or if you have had any recent knee injury. They may also ask whether you have a history of other joint problems.
If a doctor suspects that housemaid's knee is caused by infection, they may suggest that they draw some fluid from the bursa. This is a straightforward procedure. The skin on the front of your knee is sterilised with some fluid and the procedure is carried out in a clean environment.
A small needle is used to take a sample of the fluid from your prepatellar bursa, which is directly underneath the skin in front of your kneecap. This fluid is sent off to the laboratory to look for signs of infection. If infection is confirmed, the laboratory may be able to suggest which antibiotic medicines will treat it.
You do not usually need any X-rays or scans to diagnose housemaid's knee unless the diagnosis is unclear.
Housemaid's knee treatment
Back to contentsThe treatment options for housemaid's knee (prepatellar bursitis) depend on whether or not it is caused by infection.
Housemaid's knee not caused by infection
Most episodes of housemaid's knee will settle with supportive treatment and do not require medicines or surgery.
Supportive treatment
The following may be suggested for prepatellar bursitis treatment:
Resting the knee.
The use of ice packs on the knee (a tea towel wrapped around a bag of frozen peas makes a good ice pack).
For kneeling, the use of a thick foam cushion or knee pads - these can help to prevent the condition from coming back.
A physiotherapist can help by teaching you some exercises if your knee joint is affected by a reduced range of movement.
A stick or a cane can help with walking temporarily.
Housemaid's knee treatment using medicines
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can be taken for mild-to-moderate pain caused by housemaid's knee. These also help to reduce inflammation.
If housemaid's knee becomes more troublesome, your doctor may suggest that they draw out the fluid from the bursa, using a small needle. They can then inject a steroid medicine into the bursa to counteract the inflammation.
The idea is that the fluid will no longer accumulate. Infection must be excluded beforehand, as the steroid injection can make any pre-existing infection worse. You are unlikely to develop complications after this procedure. However, occasionally the following may occur:
The inflammation of the bursa (bursitis) can come back.
You can develop infection, bleeding or damage to the tendon joined to the kneecap.
Surgical treatment
In rare cases when housemaid's knee does not go away, or keeps coming back and is causing intolerable symptoms, surgery may be necessary.
This is most commonly carried out using keyhole surgery. A local anaesthetic is used (an injection is given around the knee joint to numb the area; you are not put to sleep). It is usually done as a day case which means that you are not admitted to hospital overnight.
During the surgery the prepatellar bursa is removed. The knee joint can function perfectly well without this bursa and there are not usually any long-term effects from the treatment.
Housemaid's knee caused by infection
If your housemaid's knee is thought to be caused by infection, some fluid may be drawn from your knee, as described above. This fluid can be sent off to the laboratory for tests.
Whilst waiting for the results, some antibiotics may be prescribed for you to take, for example:
Usually, these antibiotics can be taken by mouth. If the infection is severe, it may be suggested that you are admitted to hospital and given antibiotics into your veins (intravenous antibiotics).
When the laboratory return the results after a couple of days, they may suggest that your antibiotics are changed. The tests which were performed should suggest which antibiotic is most likely to be effective in treating the infection.
If your prepatellar bursitis symptoms do not seem to be improving despite 36-48 hours of antibiotics, your doctor may suggest that a small cut (incision) should be made on the front of your knee. This will allow the infected fluid to drain out from the bursa. The procedure may require referral to hospital but does not normally mean an overnight stay.
What is the outlook for housemaid's knee?
Back to contentsGenerally, the outcome is very good with appropriate treatment. You should find the condition clearing up in a few weeks.
However, if housemaid's knee is persistent (chronic) or keeps coming back, you might have long-term pain and problems moving your knee.
Can housemaid's knee be prevented?
Back to contentsTo prevent prepatellar bursitis, you should take care if you have a job or hobby that involves kneeling for a long time or frequently. In such cases, you should use thick foam cushions or knee pads. Knee pads should especially be used by people who have already had an episode of housemaid's knee, in order to prevent it from coming back.
Patient picks for Knee pain

Bones, joints and muscles
Baker's cyst
A Baker's cyst is a swelling that can develop behind the knee. It is filled with the lubricating fluid that is usually found inside the knee joint, known as "synovial fluid". It most commonly occurs if there is an underlying problem with the knee such as osteoarthritis. Symptoms can include pain, swelling and tightness behind the knee. Sometimes, a Baker's cyst can split open (rupture) and cause symptoms in the calf that can be similar to a deep vein thrombosis (DVT). A Baker's cyst often gets better and disappears by itself over time. However, there are various treatments that may help if there are symptoms associated with it.
by Dr Philippa Vincent, MRCGP

Bones, joints and muscles
Osgood-Schlatter disease
Osgood-Schlatter disease is a condition that causes swelling and pain just below the knee. It is most common in teenagers who play sport. It is not serious and usually goes away in time.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
What is a bursa, and why is the one in the knee called the prepatellar bursa?
A bursa is like a small, fluid-filled sac with a thin lining found near joints, or where ligaments and tendons pass over bones, or in areas of high pressure. Its main job is to reduce friction and help joints move smoothly. The one in the knee that gets inflamed and is called 'housemaid's knee' is specifically named the prepatellar bursa because it's located in front of the kneecap (patella), between the skin and the bone.
How quickly can I expect to recover from housemaid's knee?
With the right treatment, most cases of housemaid's knee clear up within a few weeks. However, if the condition becomes persistent or keeps returning, you might experience long-term pain and difficulties moving your knee.
Is it true that certain jobs or activities make me more likely to get housemaid's knee?
Yes, housemaid's knee is more common in people whose jobs or hobbies involve frequent or prolonged kneeling. Historically, it was common among housemaids, and today it’s often seen in tradesmen like carpet fitters, concrete finishers, and roofers, due to the pressure put on the kneecap.
If my housemaid's knee is infected, how does the doctor decide which antibiotic to give me?
If an infection is suspected, your doctor may take a fluid sample from your bursa and send it to a lab. While waiting for the results, you might be given broad-spectrum antibiotics to start. Once the lab results are back, they will indicate which specific antibiotic is most effective against the bacteria causing your infection, and your doctor may then change your prescription if needed.
Further reading and references
- Bursae and Bursitis of the Knee; Wheeless' Textbook of Orthopaedics
- Pre-patellar bursitis; NICE CKS, May 2024 (UK access only)
- Rishor-Olney CR, Pozun A; Prepatellar Bursitis. StatPearls, Jan 2024.
- Sato M, Watari T; Housemaid's Knee (Prepatellar Septic Bursitis). Cureus. 2020 Sep 11;12(9):e10398. doi: 10.7759/cureus.10398.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Sept 2027
9 Sept 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.