Infertility
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 1 Aug 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Infertility treatmentsSperm test
Infertility means difficulty in conceiving naturally (becoming pregnant) despite having regular unprotected sex when not using contraception. There is no definite cut-off point to say when a couple is infertile. Many couples take several months to conceive. About 84 couples out of 100 conceive within a year of trying. About 92 couples out of 100 conceive within two years. Looking at this another way, about 1 in 7 couples do not conceive within a year of trying. However, more than half of these couples will conceive over the following year, without any treatment.
Doctors usually suggest some tests if a couple has not conceived after one year, despite regular sexual intercourse. Tests or treatment may start earlier if the woman is older, or if there is an obvious reason why a particular couple will not conceive, however long they try.
It is usually worth seeing your doctor if you have not conceived after one year of trying. A doctor can check for some common causes, talk things over and discuss possible options. You may want to see your doctor earlier, if the woman in the couple is over the age of 36 or if either partner has a history of fertility problems, or a condition such as endometriosis or polycystic ovarian syndrome which are known to be linked with fertility problems.
At a glance
Infertility is when a couple cannot get pregnant after regular unprotected sex.
Age, ovulation problems, and issues with reproductive organs can cause female infertility.
Low sperm count, poor sperm movement, or abnormal sperm can cause male infertility.
Smoking, excessive alcohol, certain medicines, and recreational drugs can affect fertility.
See your doctor if you have been trying to conceive for 12 months or if there are other concerns.
In this article:
Video picks for General pregnancy information
Continue reading below
What can cause fertility problems?
Older women tend to be less fertile than younger women. The fall off of fertility seems to be greatest once you are past your middle 30s.
92 out of 100 women aged 19-26 trying to conceive will do so within a year.
Between the ages of 35 and 39, this drops to 82 out of 100.
Ovulation problems in women
Not producing eggs (ovulating) is the cause of problems in about 1 in 4 couples. In some women this is a permanent problem. In some it only happens from time to time: some months ovulation occurs and some months it doesn't. There are various causes of ovulation problems including:
Hormone problems (such as hormone imbalance).
Being very underweight or overweight.
Excessive exercise (such as regular long-distance running) can affect your hormone balance which can affect ovulation.
Long-term (chronic) illnesses. Some women with severe chronic illnesses, such as uncontrolled diabetes, cancers and chronic kidney disease, may not ovulate.
A side-effect from some medicines. Medicines that sometimes cause this include chemotherapy medicines. Some street drugs such as cannabis and cocaine can also affect your ability to ovulate.
Various other problems with the ovary such as certain genetic problems.
Fallopian tube, cervix or uterine problems
These are the cause in about 2 or 3 in 10 couples with infertility. Problems include:
Endometriosis, which causes about 1 in 20 cases of infertility.
Previous surgery to the Fallopian tubes, the neck of the womb (cervix) or the uterus.
What can cause infertility in men?
Back to contentsMale reproductive organs
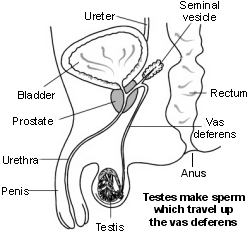
In some couples, a condition which might affect fertility is found in the male partner. The most common reason for male infertility is a problem with sperm, due to an unknown cause. The sperm may be reduced in number, less able to swim forwards (less mobile) and/or be abnormal in their form.
There are various risk factors that may affect sperm production and male infertility. These include:
Current or past infection of the testicles (for example, mumps).
Current or past infections of another part of the sperm-producing system, such as gonorrhoea or other sexually transmitted infections.
Side-effects of some medicines and street drugs. These include sulfasalazine, nitrofurantoin, tetracyclines, cimetidine, colchicine, allopurinol, some chemotherapy drugs, cannabis, cocaine and anabolic steroids.
Scarring from previous operations (such as an inguinal hernia repair) may block the ducts which carry sperm, and affect fertility.
A varicocele may possibly affect male fertility.
Certain hormone problems (for example, problems with the pituitary gland in the brain leading to conditions such as Cushing's syndrome or hyperprolactinaemia).
Some inherited conditions, due to abnormal genes, may affect the development and function of the testicles. Examples are conditions known as Klinefelter's syndrome and Kallman's syndrome.
Being overweight may reduce fertility in men.
Unknown causes
No cause can be found in about 1 in 4 couples with infertility.
Continue reading below
When to see a doctor about infertility
Back to contentsMost doctors are happy to talk through any difficulties that you may have concerning fertility. It is best for both partners to seek medical advice together. It is quite usual for doctors to do the following:
Ask how long you have been trying to get pregnant and if you have been pregnant before. (This includes asking the male partner if any previous partner of his has been pregnant before.)
Go over your general health and discuss any past illnesses and infections.
Ask about any medication or recreational drugs that you may be taking.
Ask if you smoke and how much alcohol you drink. Your doctor may also discuss your weight.
Ask about your occupation.
Ask if either partner is feeling stressed at present.
Talk about sex and be sure there are no sexual problems. Sometimes people ask their doctor about difficulties with fertility when the real problem is difficulty with sex.
Examine both partners. This can include weighing both partners, a pelvic examination for a woman and an examination of the penis and scrotum for a man.
Tests for infertility
Back to contentsYour doctor may suggest a few tests. For example:
A sperm test (semen analysis) of the male partner.
A blood test to check that ovulation occurs in the female partner. This measures the hormone progesterone which is high just after ovulation. The blood sample is taken on the 21st day of a regular 28-day cycle (counting day one as the first day of bleeding).
Blood tests for other hormones, including prolactin, thyroid hormone, and a hormone called FSH which is high in women who have gone through their menopause.
They may also suggest some other tests, depending on any other symptoms that you may have. For example, whether the female partner has regular periods or not, etc. Further blood tests or an ultrasound scan may be helpful in finding out your risk of infertility.
Tests for common infections, such as HIV, hepatitis B and hepatitis C.
A test to see if the woman is immune to rubella - if not, she should have the MMR vaccination and ideally pause trying to conceive for three months after the vaccination.
Tests or referral to a doctor who is a specialist are generally not suggested until you have been trying to conceive for 12 months:
If the female partner is under the age of 36.
If both partners are otherwise healthy.
If your doctor has not found any problems in the examination or tests that he or she has carried out.
If any of these conditions do not apply, you may be referred earlier to a doctor who is a specialist.
Continue reading below
Some general advice
Back to contentsThe success rate of conceiving gradually goes down over time. However, for couples where no cause is found for the problem, there is still a good chance of conceiving without treatment. In such couples, without treatment, about half who do not conceive within one year conceive within the following year. Therefore, the usual pre-conception advice still applies. For example, women are advised to:
Take folic acid each day to reduce the chance of a spinal cord problem in a baby.
Eat a healthy diet.
See the separate leaflet called Planning to Become Pregnant.
In addition, the following may be relevant to some people:
Smoking
This can affect fertility in men and women. It has been estimated that in each menstrual cycle, smokers have about two thirds the chance of conceiving compared to non-smokers. Smoking is also harmful to a developing baby if the mother smokes. Therefore, it is a good time for both partners to stop if they are smokers.
Alcohol in excess
This may affect fertility - both for men and for women. The Department of Health recommends that women trying to become pregnant do not drink any alcohol. However, the exact amount of alcohol that is safe during pregnancy is not known. This is why the advice is not to drink at all.
If you do choose to drink when trying to become pregnant then limit it to one or two units, once or twice a week. (This is the equivalent of one or two glasses of wine, once or twice a week.) You should never binge drink or get drunk. This is because alcohol may harm a developing baby.
Medication
If you take any medication regularly and are thinking about becoming pregnant, discuss this with your doctor in advance. Some medicines can affect a developing baby and may need to be changed before you become pregnant. An important example of this is medicines for epilepsy.
Diabetes
If you have a medical condition which needs regular monitoring, in particular diabetes, it is very important to start planning before you ever become pregnant.
Weight control
You may have a reduced chance of conceiving if you are very overweight or underweight. For the best chance of conceiving, you should aim to have your body mass index (BMI) at between 20 and 30.
If appropriate, see your practice nurse to measure your BMI and for advice about diet and weight control. Participating in a group programme involving exercise and dietary advice has been shown to lead to more pregnancies than weight loss advice alone.
Some recreational drugs
Recreational drugs can affect fertility and should be avoided.
Sex and fertility
Back to contentsAfter a couple has had unprotected sex, sperm survive for up to seven days. Therefore, even though an egg (ovum) only survives for 12-24 hours, having sex two or three times a week is sufficient if you are trying to conceive.
Studies have shown that having sex every two to three days is likely to maximise your chance of getting pregnant. You may want to have sex more often, which is fine, but it probably will not increase your chance of conceiving. It is thought that the more relaxed and spontaneous your sex life, the more likely that you will conceive.
The idea behind using temperature charts and ovulation kits to help predict when you are most fertile is that this can help you time when to have sex. However, using methods like this has not been shown in studies to improve your chance of conceiving. It can also cause a lot of stress within a relationship. They are therefore not usually recommended.
Doctors are used to talking about sexual problems. Any worries or concerns in this area are best talked over with your doctor.
Infertility treatment
Back to contentsThe treatments for infertility will depend on the underlying cause. The treatments, such as fertility drugs, are discussed in a separate leaflet on infertility treatments.
Patient picks for General pregnancy information

Pregnancy
Pregnancy and smoking
If you smoke and you are pregnant or planning to become pregnant, you are strongly advised to stop to benefit your health and the health of your baby.
by Dr Mary Harding, MRCGP

Pregnancy
Early pregnancy signs and symptoms
Pregnancy tests are very sensitive so it is common to find out that you are pregnant before you develop any signs or symptoms of pregnancy. However, as your pregnancy continues you may experience these early symptoms and signs of pregnancy. For further advice about having a healthy pregnancy, see also the leaflet Planning to Become Pregnant, which includes information about prenatal vitamin recommendations.
by Dr Colin Tidy, MRCGP
Frequently asked questions
What is the likelihood of conceiving naturally if no cause for infertility is found?
If no specific cause for infertility can be identified, there's still a good chance of conceiving without medical treatment. Approximately half of couples who don't conceive within the first year without treatment will become pregnant in the following year.
How does increasing age affect a woman's fertility?
A woman's fertility generally decreases with age, with the most significant decline occurring after her mid-30s. For example, while 92 out of 100 women aged 19-26 trying to conceive will do so within a year, this number drops to 82 out of 100 for women aged 35-39.
Should I be concerned about my medication if I am planning to get pregnant?
Yes, if you're taking any regular medication and are considering pregnancy, it is important to discuss this with your doctor in advance. Some medicines can potentially harm a developing baby, and your doctor may need to adjust your medication before you try to conceive. Medicines for epilepsy are an important example where this consultation is crucial.
Can my weight impact my ability to conceive?
Both being very overweight and very underweight can reduce your chances of conceiving. To optimise your fertility, it is recommended to aim for a Body Mass Index (BMI) between 20 and 30. Your practice nurse can help you measure your BMI and offer advice on diet and weight management, which has been shown to increase pregnancy rates.
Is it helpful to use ovulation predictor kits or temperature charts to time intercourse?
While these methods aim to help you identify your most fertile window for sex, studies have not shown that using temperature charts or ovulation kits actually increases your chances of conceiving. They can also create stress in a relationship and are therefore not typically recommended.
How soon after quitting smoking might my fertility improve?
Smoking can negatively affect fertility in both men and women. It is estimated that smokers have about two-thirds the chance of conceiving per menstrual cycle compared to non-smokers. Quitting smoking for both partners is advised for improving fertility and reducing harm to a developing baby.
What kind of information does a doctor typically collect during an initial infertility consultation?
During an initial consultation for infertility, your doctor will usually ask about how long you've been trying to conceive, any previous pregnancies, your general health, past illnesses, medications, recreational drug use, smoking and alcohol habits, occupation, and stress levels. They will also discuss your sexual health and may conduct physical examinations, including weighing both partners, a pelvic examination for women, and an examination of the penis and scrotum for men.
Further reading and references
- Santos EP, Lopez-Costa S, Chenlo P, et al; Impact of spontaneous smoking cessation on sperm quality: case report. Andrologia. 2011 Dec;43(6):431-5. doi: 10.1111/j.1439-0272.2010.01089.x. Epub
- Fertility - Assessment and treatment for people with fertility problems; NICE Guidance (February 2013, updated September 2017)
- Infertility; NICE CKS, August 2018 (UK access only)
- Sexual and Reproductive Health; European Association of Urology. 2025.
- Human Fertilisation and Embryology Authority
- Bordewijk EM, Ng KYB, Rakic L, et al; Laparoscopic ovarian drilling for ovulation induction in women with anovulatory polycystic ovary syndrome. Cochrane Database Syst Rev. 2020 Feb 11;2(2):CD001122. doi: 10.1002/14651858.CD001122.pub5.
- Gibbons T, Reavey J, Georgiou EX, et al; Timed intercourse for couples trying to conceive. Cochrane Database Syst Rev. 2023 Sep 15;9(9):CD011345. doi: 10.1002/14651858.CD011345.pub3.
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 31 Jul 2028
1 Aug 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.