Metatarsal fractures
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 3 Jul 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Plantar fasciitisAchilles tendinopathyAchilles tendon ruptureMetatarsalgiaMorton's neuromaFlat feet and fallen arches
A metatarsal fracture occurs when one of the long bones of the midfoot is cracked or broken. This may be due to sudden injury (an acute fracture), or due to repeated stress (stress fracture).
In this article:
Video picks for Foot and ankle injuries
Continue reading below
Where are the metatarsal bones?
The metatarsal bones are the long slim bones which run the length of the foot to the base of the toes. They are the most commonly broken (fractured) bones in the foot. There are five metatarsal bones in each foot.
Heel and foot bones
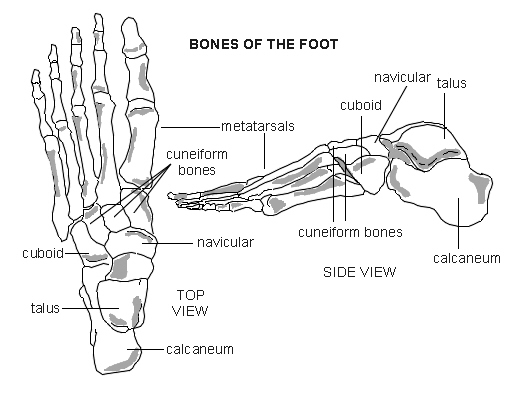
A metatarsal fracture is a break in one of the five long bones which form the middle part of the foot.
Are there different types of metatarsal fracture?
Back to contentsMetatarsal fractures (broken metatarsal bones) can be acute, or caused immediately by injury. They can also occur following recurrent trauma over a longer period of time, when they are called stress fractures.
Acute metatarsal fracture
An acute metatarsal fracture is usually caused by a sudden forceful injury to the foot, such as dropping a heavy object on to the foot, kicking against a hard object when tripping, falling or from a sporting injury.
A metatarsal break may be open or closed, and displaced or not displaced:
Open or closed: A closed fracture is far more common - this is where the bone is broken but the skin and other tissues remain intact over and around the broken bone. An open fracture is one where the skin is broken over the fracture. This is a more serious type of fracture, with more damage to the soft tissues around it making treatment and healing more complicated. There is also a route of possible infection from the outside into the broken metatarsal bone. Specialist assessment is always needed for an open fracture.
Displaced or not displaced: A non-displaced fractured metatarsal is much more common than displaced. A displaced fracture is one where, following the break, the bones have slipped out of line. A displaced fracture needs specialist care, as the bones will need to be properly lined up and stabilised. This may involve an anaesthetic and some kind of metal pinning or plating to the bones.
5th metatarsal fracture
The fifth metatarsal bone is the most common metatarsal bone to be fractured in sudden (acute) injury to the foot. It may be broken at various points along its length, depending on the mechanism of injury. The other metatarsal bones can also be broken. The first, second and fifth metatarsals are the most commonly injured in sport. Several well-known footballers have had metatarsal fractures in recent years.
Stress fracture
A stress metatarsal fracture occurs when the metatarsal bone fractures due to repetitive stress. In this instance, the metatarsal break is usually only partway through the bone. There may be a single split in the bone, or multiple small splits. Because the fracture does not affect the full thickness of the broken metatarsal bone, stress fractures are not generally displaced. However, several small stress fractures can develop around the same area.
Continue reading below
What causes metatarsal fractures?
Back to contentsAcute metatarsal fractures
These are usually caused by a direct injury to the foot. This may happen, for example, through someone stepping on or kicking the foot, by dropping something on to the foot or by falling on to the foot.
Twisting of the foot or the ankle can also cause fractures of the base of the fifth metatarsal. In this injury, the twisting mechanism pulls on a strong ligament that attaches to the base of the fifth metatarsal which then pulls off a fragment of bone.
The shaft of the metatarsal can be injured due to twisting the foot on landing from a jump. This is a common problem in ballet dancers.
Stress fractures
This type of metatarsal fracture generally occurs due to:
Repeated stress to the bone, which is also termed overuse.
Marching or running for long distances, especially if carrying heavy packs (which is why they used to be called 'march fractures'). They are often found in athletes and sportspeople although they can affect any runners, even those who only run a little. They are commonly seen in the military during training exercises.
Stress fractures are more common in runners who:
Suddenly increase their running mileage or intensity.
Run in poor footwear that doesn't suit their feet.
Have a sudden change in footwear.
Have just changed their running shoes and not 'broken them in' carefully.
Continue to exercise despite having foot pain.
People's choices and needs for running shoes vary. Advice from a specialist should be sought before choosing a more unusual shoe type such as barefoot shoes or corrective shoes. For example, there is a particular technique for barefoot running. It's advised to break in new running shoes gradually - many injuries result from a sudden change in running shoes. Ballet dancers and gymnasts are also prone to broken metatarsal bones.
Abnormalities of the structure of the foot, and abnormalities of the bones and joints, such as rheumatoid arthritis or 'thinning' of the bones (osteoporosis), can make stress fractures more likely.
They can also occur in people who have lost nerve sensation in their feet due to neurological problems - for example, diabetes that has affected the feet.
Does osteoporosis cause metatarsal fractures?
Back to contentsMetatarsal fractures occur more easily if the metatarsal bones are weakened due to 'thinning' of the bones (osteoporosis).
See the separate leaflet called Osteoporosis for more detail.
Continue reading below
Does ageing make metatarsal fractures more likely?
Back to contentsMost metatarsal fractures occur in younger people, as they are more likely to be involved in the kinds of sports and activities that are higher risk. However, as we become older the 'springiness' and padding of our feet tend to reduce. This means that our feet absorb impact less well and it is easier to fracture bones. Supportive footwear will make this much less likely.
See the separate leaflet called Ageing feet for more detail.
What are the symptoms of a metatarsal fracture?
Back to contentsAcute metatarsal fracture
There is usually immediate pain and tenderness around the area of the fracture.
The pain is often described as 'pinpoint pain' as it is usually well localised at the site of impact to the bone.
Bruising and swelling often develops due to bleeding and inflammation around the injury site. It may be difficult to put weight on the affected foot.
Movement of your foot may also be limited.
Mobility with a broken bone in the foot depends on which bone (and which part of the bone) is broken, whether the fracture is displaced, the supportiveness of the shoes and on personal tolerance to pain.
Stress fractures
These cause similar symptoms to acute metatarsal fractures (above), although there is usually no bruising.
At first, the main symptom may just be pain in the foot during exercise that is relieved by rest. The pain tends to be widespread and diffuse in the foot.
After a while, the pain may become continuous, so that it is not relieved by resting. The sore area tends to become more localised to the area of the fracture, and the pain gradually increases.
Typically the stress fracture causes a tender area along the line of the second or third metatarsal bone.
There may be some swelling but there is usually no bruising.
People who have stress fractures may continue to walk for some time. Eventually this becomes increasingly painful, as the splits in the bone tend to worsen and the bone itself starts to react and become inflamed, and it can become impossible to weight bear. A metatarsal stress fracture can progress to become a full-thickness fracture.
Will the pain increase?
Back to contentsMetatarsal stress fractures can begin as very small injuries which do not cause severe pain. However, if the bone continues to experience stress, the crack will often deepen and widen, becoming gradually more painful. Eventually, in the worst case scenario, the stress fracture may progress to become a full fracture.
In an acute fracture, if the bone continues to experience stress, the pain will increase further as the broken ends of bone will start to rub slightly against one another and the area will become inflamed. In the worst case scenario the fracture may become displaced.
Do I need any investigations?
Back to contentsA healthcare worker is likely to suggest an X-ray of the foot if they suspect a metatarsal fracture.
Acute metatarsal fractures
Most can be seen easily on X-ray. Initially doctors can see the crack in the bone, and after a few days they can also see irregularities in the bone as it starts to heal and remodel itself.
CT scan (computerised tomography scanning) or MRI scan (magnetic resonance imaging scanning) are almost never required for broken bones in the foot.
Stress fractures
These do not show up as easily on X-ray, particularly not at first. Half of them never show up on a normal X-ray.
There can be multiple, very tiny fractures and splits in the bone, or just one fine crack which doesn't go right through the bone. Because they have formed very gradually, the bone may not have 'reacted' very much to the injury.
A specialised ultrasound scan may show a fracture that can't be seen on X-ray.
Metatarsal stress fractures can usually be seen by using a bone scan.
MRI scanning is also sometimes used to find stress fractures.
Do I need to see a doctor if I suspect metatarsal fracture?
Medical advice should be sought if a metatarsal fracture or other broken bone in the foot is suspected. This is usually best provided in an Urgent Care Centre or the equivalent as x-rays will be available at the time.
Metatarsal fracture treatment
Back to contentsThis depends on:
Which metatarsal bone is broken (fractured).
Which part of the metatarsal bone is broken.
How severe the damage is.
Whether it is an acute fracture or a stress fracture.
It also depends on:
Whether the fractured bone is displaced or non-displaced (see above).
Whether the tissues of the foot around the break are also badly injured causing the fracture to be an open fracture.
The basic principles of treating metatarsal fractures are as follows.
Simple painkillers
Painkillers such as paracetamol and anti-inflammatory tablets such as ibuprofen which may help to relieve pain.
Ice
Applying ice to the foot can also be helpful as pain relief and to reduce inflammation. Ice should be applied as soon as possible after injury, for 10-30 minutes. (Less than 10 minutes has little effect. More than 30 minutes may damage the skin.) Make an ice pack by wrapping ice cubes in a plastic bag or towel, or by using a bag of frozen peas.
Do not put ice directly next to skin, as it may cause ice burn. Gently press the ice pack on to the injured part. The cold is thought to reduce blood flow to the damaged area. This may limit pain, inflammation and bruising.
Some doctors recommend re-applying for 15 minutes every two hours (during daytime) for the first 48-72 hours. Do not leave ice on while asleep.
See the separate leaflet called Ice and heat therapy for pain relief for more details.
Rest and elevate
Elevation initially aims to limit and reduce any swelling. For example, the foot should be kept up on a chair to at least hip level when sitting or on a pillow when in bed. Sometimes rest is the only treatment that is needed, even in traumatic fracture.
Stop stressing the foot
With a stress fracture, it is important to avoid the activity that caused it.
Immobilisation
Some fractures need support to help healing. For example, a supportive elastic tubular bandage with a supportive, rigid shoe or boot may be advised. If needed, special shoes are available to help to immobilise the fracture and support the foot enable walking.
Progressive weight bearing on the foot can then follow as pain allows. Other fractures may need treatment with a below-the-knee plaster cast.
Surgery
Very occasionally, surgery may be necessary to re-align any part of the bone that has moved out of position. Surgery is not needed for stress fractures.
Follow-up care
Physiotherapy and a gradual return to exercise are a part of good follow-up care.
How long does a metatarsal fracture take to heal?
Back to contentsAcute metatarsal fractures
These generally take around six to eight weeks to heal. However, it may be longer than this before a sportsperson is fully back in action.
Stress fractures
These will normally heal without any complications and, in time, people are able to return to their previous activities fully. Return to normal activities is advised when they can be performed without pain. This will typically take six to twelve weeks.
However, when starting exercising again, it is important to gradually build up the activity levels. A sudden return to high-intensity exercise after a break may cause a repeat or a new stress fracture or other injury.
What if the pain gets worse?
If the pain gets worse then medical advice should be sought. The expected pattern of healing, in bony injuries of any kind, is that they should gradually hurt less as healing occurs, and any gradual worsening of pain should be reviewed.
If foot pain is increasing over time then activity may be making an existing problem worse. In the case of a stress fracture this may mean progression to an acute fracture.
In the case of an acute fracture it may be worsening displacement of the bones and preventing the two ends of the bone from knitting together.
What are the complications of metatarsal fractures?
Back to contentsIf properly treated then metatarsal fractures should heal without any long-term consequences. If not recognised and treated then some of these problems can occur:
A metatarsal stress fracture can become gradually worse if repeated stress to the bone continues. It can eventually become a full-thickness metatarsal fracture.
A fracture of the first metatarsal bone can lead to later arthritis of the big toe joint.
A fracture at the base of the fifth metatarsal bone is often mistaken for an ankle sprain and therefore not rested or supported enough. This can lead to problems in healing and continuing pain.
A full-thickness fracture which is displaced and not 'put back' into line can heal 'out of shape', leading to deformity of the foot, sometimes making shoe fitting difficult. The foot may be painful.
Acute metatarsal fracture can also, occasionally, lead to 'non-union', which is when the two ends of broken bone stop trying to heal because movement between them makes this impossible. This may lead to reduced ability of the foot to cope with stresses and strains of walking and running and it may also lead to chronic pain in the foot.
How to prevent metatarsal stress fractures
Back to contentsThere are a number of things that can be done to help prevent stress fractures:
Exercise intensity and duration should be built up slowly and gradually.
Rest time and recovery time need to be built in to any training schedule.
Footwear should be well fitting and suit the running style.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Foot and ankle injuries

Bones, joints and muscles
Broken toe
A broken (fractured) toe is a fairly common injury which usually needs no specific treatment. It is most often caused by dropping a heavy object on to your foot or badly stubbing your toe.
by Dr Toni Hazell, MRCGP

Foot care
Metatarsalgia
Metatarsalgia is the name given to pain in the front part of the foot under the heads of the metatarsal bones, also known as the ball of the foot. Metatarsalgia can be caused by a number of different conditions affecting the foot. Treatment will depend on the underlying cause. Measures such as changes to footwear, rest and losing weight can sometimes help.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Kiel J, Kaiser K; Stress Reaction and Fractures
- Smidt KP, Massey P; 5th Metatarsal Fracture.
- Ficek K, Kedra N, Skowronek R, et al; The Fifth Metatarsal Bone Fracture in Athletes - Modalities of Treatment Related to Agility in Soccer Players. J Hum Kinet. 2021 Jul 28;79:101-110. doi: 10.2478/hukin-2020-0059. eCollection 2021 Jul.
- Agrawal U, Tiwari V; Metatarsal Fractures.
- Chloros GD, Kakos CD, Tastsidis IK, et al; Fifth metatarsal fractures: an update on management, complications, and outcomes. EFORT Open Rev. 2022 Jan 11;7(1):13-25. doi: 10.1530/EOR-21-0025.
- Virtual Fracture Clinic; Metatarsal Fracture
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 3 Jul 2027
3 Jul 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.