Polycystic ovary syndrome
PCOS
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 12 May 2026
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Polycystic ovary syndrome (PCOS) is a metabolic condition that affects how the ovaries work. It can cause symptoms such as weight gain, excess hair growth, period problems, and can impact fertility.
In this article:
Video picks for Ovarian problems
Key points
PCOS is a common condition that affects how ovaries work and how the body processes energy (metabolism).
Key symptoms include irregular periods, fertility issues, acne, excess hair, and weight gain.
The exact cause is unknown but is thought to be caused by a mix of hormones, insulin resistance, and genetics.
There is no cure for PCOS but lifestyle changes such as losing weight and other treatments can control symptoms.
Continue reading below
What is polycystic ovary syndrome (PCOS)?
Polycystic ovary syndrome (PCOS) is a medical condition that affects how the body regulates hormones. It can affect how the ovaries function.
People with polycystic ovaries often have insulin resistance. Insulin resistance raises insulin levels and disrupts hormones, which increases testosterone and can stop eggs from developing and being released properly.
These hormone changes can cause symptoms such as enlarged ovaries, irregular periods, reduced fertility, acne, excess hair growth, and weight gain.
PCOS is one of the most common causes of not being able to get pregnant (infertility). However, not all women with PCOS have problems getting pregnant. If you have PCOS and you do not want to get pregnant, it is very important for you to use contraception
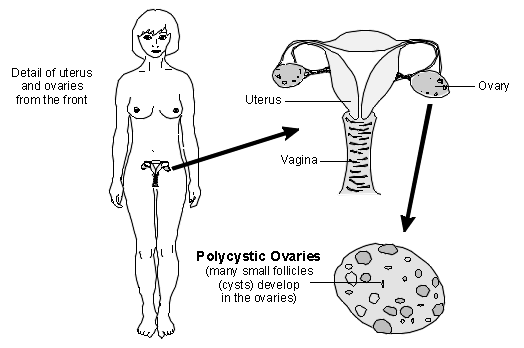
What are polycystic ovaries?
Back to contentsPolycystic ovaries can be seen on an ultrasound scan. Normally your ovaries develop one large follicle (a fluid filled sac) a month which then releases the egg - this is called "ovulation". In polycystic ovaries, the higher levels of testosterone mean that lots of follicles start to form but they don't develop into a full-sized follicle. This can mean that an egg is not produced each month.
It is very important to understand that you can have polycystic ovaries on a scan but not have polycystic ovary syndrome. It is also possible to have polycystic ovary syndrome but have normal looking ovaries on a scan.
What is PCOS?
Continue reading below
How common is PCOS?
Back to contentsPolycystic ovary syndrome is common and affects between 1 in 20 women and 1 in 5 women.
Polycystic ovaries are more common than polycystic ovary syndrome; a large proportion of teenagers have polycystic ovaries.
Read the article 8 common myths about PCOS.
Polycystic ovaries
PCOS symptoms
Back to contentsSymptoms of PCOS include:
Period problems - such as irregular or light periods, or no periods at all.
Fertility problems - such as issues with ovulation.
Excess hair growth (hirsutism) - on the face, lower stomach (abdomen) and chest. It occurs in more than half of women with PCOS.
Acne - that may persist beyond the normal teenage years.
Weight gain - women with PCOS are more at risk of becoming overweight or having obesity.
Depression or poor self-esteem may develop as a result of the other symptoms.
PCOS symptoms can vary from mild to severe and may also change over the years. For example, acne may become less of a problem in middle age but hair growth may become more noticeable.
What age does PCOS start?
Some of the symptoms of PCOS, particularly irregular periods, are very common in the first few years after you start having periods. For this reason, scans are not recommended until at least 8 years after your periods start. If you have PCOS, rather than just polycystic ovaries without the syndrome, this can be diagnosed by looking at your symptoms and doing blood tests.
Continue reading below
What causes PCOS?
Back to contentsThe cause of polycystic ovary syndrome is unknown. It can run in families. It is likely that women have an increased risk of PCOS due to their family history (genetics) but then other factors lead to a higher chance of actually developing PCOS. These factors are being overweight, smoking, and exposure to smoke from coal or wood fires. It is thought that some of the chemicals used to make plastic might also increase the chances of developing PCOS. Black women and those from the Middle East are more likely to develop PCOS than white or Chinese women.
PCOS diagnosis
Back to contentsDiagnosis of PCOS usually involves looking at your symptoms, medical history, and tests to check your hormone levels.
Tests may include:
Blood tests - to measure certain chemicals (hormones). Tests will be done to measure the male hormone testosterone and another hormone called sex hormone binding globulin. Other tests looking at luteinising hormone (LH) and prolactin will often be tested but these are not used to diagnose PCOS; they may help to rule out other conditions.
An ultrasound scan of the ovaries - to detect the typical appearance of PCOS with the many small cysts (follicles) in slightly enlarged ovaries. Scans should not be done in the first 8 years after starting your periods as polycystic ovaries are very common in this age group but do not persist after 8 years.
Diagnosis criteria
PCOS is diagnosed differently in adults and in adolescents.
In adults, you need to have 2 out of these 3 criteria:
Infrequent periods (fewer than 8 periods every year OR a year when you had periods more often than every 21 days or periods less often than every 35 days OR a period coming more than 90 days after the last one).
Evidence of high testosterone levels - either from blood tests or from symptoms of hairiness, loss of scalp hair or acne.
A scan showing at least 12 tiny cysts (follicles) in your ovaries.
In adolescents (children, teenagers and young women in the first 8 years of having periods), you need to have both of these criteria:
Infrequent periods - see below *
Evidence of high testosterone levels - either from blood tests or from symptoms of hairiness, loss of scalp hair or acne.
It is very common to have irregular and infrequent periods when you first start having periods. This is normal for many girls in the first year.
* Infrequent periods in adolescents are:
A whole year of periods coming more than 45 days apart.
3 whole years of periods coming more than 35 days apart or less than 21 days apart.
A period coming 90 days late, as long as it is more than a year since you started your periods.
Not starting your periods by the age of 15.
Screening for diabetes or non-diabetic hyperglycaemia (NDH)
You may be advised to have an annual screening test for diabetes or non-diabetic hyperglycaemia, also known as pre-diabetes or impaired glucose tolerance.
A regular check for other cardiovascular (heart disease) risk factors such as blood pressure and blood cholesterol, may be advised to detect any abnormalities as early as possible. Exactly when and how often the checks are done depends on your age, weight and other factors. After the age of 40, these tests are usually recommended every five years, or more often if an abnormality is found.
PCOS treatment
Back to contentsThere is no cure for PCOS. However, symptoms can be treated with lifestyle changes and medication.
Losing weight
Losing weight helps to reduce the high insulin level that occurs in PCOS. This can improve your chances of ovulation, regulate your periods, and improve your fertility.
Even a moderate amount of weight loss can help - losing 10% of your body weight has a significant chance of helping you to ovulate and so increasing your fertility.
It may also reduce acne, excess hair growth, and long-term problems such as diabetes and high blood pressure.
You can find out whether you are a healthy weight by calculating your BMI (body mass index).
Losing weight can be hard. Advice from a dietician may increase your chance of losing weight, or you could be referred to a weight loss clinic for consideration of medication (such as orlistat or injections of medications known as GLP1 agonists) or surgery to help with weight loss.
Access to these clinics on the NHS varies significantly by area.
Diet and exercise
Consuming a diet high in wholegrains, fruits, vegetables, and pulses, while limiting white bread, pasta, rice, potatoes, and sugary foods and drinks can help manage symptoms.
A healthy diet for PCOS focuses on low glycaemic index (low GI) foods that are absorbed slowly and help keep blood sugar levels steady.
Exercise has also been shown to help with PCOS by improving the body’s sensitivity to insulin, which helps balance hormones and support regular ovulation.
Treating hair growth
Hair growth caused by increased levels of testosterone can be removed by shaving, waxing, using hair-removal creams, electrolysis, and laser treatments.
These need repeating every now and then, although electrolysis and laser treatments may be more long-lasting (but are expensive and are often not available on the NHS).
Medical treatments are also available. A cream called eflornithine can slow facial hair growth. This is only usually available in hospital endocrinology (hormone specialist) clinics.
The combined oral contraceptive (COC) pill can also reduce the effects of testosterone which can reduce hair growth.
These treatments can take several months to work, and hair growth may return if they are stopped. Some medications may not be suitable for everyone due to side effects or increased risk of blood clots.
Treating acne
The treatments used for acne in women with PCOS are no different to the usual treatments for acne.
The combined oral contraceptive pill often helps to improve acne.
See the separate leaflets called Acne and Acne treatments which covers topical treatments and antibiotic tablet treatment for acne.
Treating period problems
When women with PCOS have periods less than every 3 months, it is possible for the lining of the womb to get thicker - this is called "endometrial hyperplasia". Endometrial hyperplasia leads to a higher risk of endometrial cancer (cancer of the womb/uterus) so, in women over 18 years of age, treatment is needed to induce regular bleeding.
This treatment can be:
the combined contraceptive pill
progestogen medication, such as medroxyprogesterone, given every 3 months to make you have a bleed
a hormonal intrauterine device - this can be confusing as many women have no bleeds at all with this. However this is because the lining of the womb becomes very thin and so there is a reduced risk of endometrial cancer.
Fertility treatment
If you’re not ovulating and want to get pregnant, a specialist may recommend fertility treatment, which often works well. Medicines such as Clomifene or letrozole can help trigger ovulation.
Being overweight or having obesity can lower your chances, so weight loss is usually advised, and in some areas treatment is only offered below a certain BMI.
Metformin and other insulin-sensitising medicines
Metformin is a diabetes medication that improves insulin sensitivity and may help with PCOS. It is usually recommended for women with higher risks - particularly women with a BMI over 25 or women of Black, Asian or South American ethnicities.
For adolescents, metformin is only recommended if advised by a specialist.
Complications of PCOS
Back to contentsIf you have PCOS, over time you have an increased risk of:
Developing type 2 diabetes.
Developing diabetes in pregnancy.
Being overweight, particularly around the tummy.
Developing endometrial hyperplasia and, if not treated with preventative medication, endometrial cancer.
These problems in turn may also increase your risk of having a stroke and heart disease in later life. These increased health risks are due to the long-term insulin resistance.
Other possible problems in pregnancy include a higher chance of:
Having premature babies.
Preventing long-term problems
A healthy lifestyle is important to help prevent the conditions listed above.
For example, you should:
Eat a healthy diet.
Exercise regularly.
Lose weight if you are overweight or have obesity.
Not smoke.
Healthy lifestyle advice applies to everyone, whether they have PCOS or not. However, it is particularly important for women with PCOS, as they may have extra risk factors for health problems in later life.
Living with PCOS
Back to contentsCan PCOS affect mental health?
PCOS does not affect mental health in itself but there is a higher rate of women getting depression, anxiety and eating disorders with PCOS. This may be because of the symptoms of PCOS.
Does PCOS go away during menopause?
PCOS is a lifelong condition although, with lifestyle changes and medication, many women have reduced or no symptoms of PCOS. It does not go away after the menopause although some of the symptoms reduce (for example, there are no period symptoms!) Many women without PCOS develop some of the same symptoms as PCOS after the menopause - for example increased hair growth or thinning of the scalp hair.
Frequently asked questions
Back to contentsWhat does a PCOS flare up feel like?
There is not really such a thing as a PCOS flare up. PCOS is a chronic condition which means it is long-term. The symptoms tend to be fairly stable. There may be flare ups of certain aspects such as acne which can get worse and better over time.
Can you get pregnant with PCOS?
Yes, many women get pregnant with PCOS. If you do not want to get pregnant, it is very important to use reliable contraception. If you are able to take it, the combined oral contraceptive pill is a good method to use as it also tends to reduce some of the symptoms of PCOS. Also, because the multiple cysts on the ovaries often disappear when taking the COCP, there is some evidence that fertility is higher in the few months after stopping it.
However, about 7 in 10 women with PCOS do have more problems getting pregnant than the average woman. If you have PCOS and are not having regular periods and are trying to get pregnant, you should be referred to a fertility specialist. (You will need blood tests and a scan, and your partner will need to provide a sperm sample, before this referral can be made).
Can PCOS be prevented?
Many women have a tendency to develop PCOS and this cannot always be prevented. However, keeping a healthy weight, not smoking and eating a healthy low sugar diet can reduce the risks of developing PCOS.
What is a PCOS belly?
Due to the insulin resistance which is part of PCOS, there is a tendency to gain weight and this weight gain tends to be worse around the abdomen.
Can PCOS go away?
PCOS is a lifelong condition. However, maintaining a healthy weight, eating a healthy diet and not smoking can reduce the symptoms. Polycystic ovaries (without the syndrome) very often go away and this is why girls and young women should not have a scan in the first 8 years after starting their periods.
Patient picks for Ovarian problems

Women's health
Premature ovarian insufficiency
Premature ovarian insufficiency is sometimes called premature ovarian failure. The condition occurs when your ovaries no longer work properly when you are under the age of 40 years. Your ovaries no longer produce normal amounts of oestrogen and therefore may not produce eggs. This means that your periods stop (or become irregular) and you may experience symptoms of the menopause. In the majority of women, this occurs around the age of 51 years and is called the menopause. The term early menopause is usually used if you go through the menopause when you are between 40 and 45 years of age. With premature ovarian insufficiency your ovaries are not working properly and have stopped producing eggs early. In some women, however, this loss of function is temporary and their ovaries work and function again in the future. This means that you may find that your periods return at some stage in the future. Therefore premature ovarian insufficiency is not necessarily the same as premature menopause, which means the irreversible loss of ovarian function before the age of 40 years. Around 4 in 100 women under the age of 40 years have premature ovarian insufficiency. About 4 in 100 women have premature menopause.
by Dr Colin Tidy, MRCGP

Women's health
Ovarian cyst
Ovarian cysts are fluid-filled pockets that grow on the ovaries. Almost all ovarian cysts are non-cancerous (benign), but some are cancerous (malignant), or may become cancerous over time. Many people with ovarian cysts don't have any symptoms or require any treatment, as many go away on their own. However, some ovarian cysts may need removal with an operation.
by Dr Toni Hazell, MRCGP
Further reading and references
- Hirsutism; NICE CKS, October 2024 (UK access only)
- Fraison E, Kostova E, Moran LJ, et al; Metformin versus the combined oral contraceptive pill for hirsutism, acne, and menstrual pattern in polycystic ovary syndrome. Cochrane Database Syst Rev. 2020 Aug 13;8:CD005552. doi: 10.1002/14651858.CD005552.pub3.
- Morley LC, Tang T, Yasmin E, et al; Insulin-sensitising drugs (metformin, rosiglitazone, pioglitazone, D-chiro-inositol) for women with polycystic ovary syndrome, oligo amenorrhoea and subfertility. Cochrane Database Syst Rev. 2017 Nov 29;11:CD003053. doi: 10.1002/14651858.CD003053.pub6.
- Polycystic ovary syndrome; NICE CKS, March 2025 (UK access only)
- Teede HJ, Tay CT, Laven JJE, et al; Recommendations from the 2023 international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Eur J Endocrinol. 2023 Aug 2;189(2):G43-G64. doi: 10.1093/ejendo/lvad096.
- PCOS Charity Verity
- Fertility problems: assessment and treatment; NICE guideline (March 2026)
- International Evidence-based Guideline for the assessment and management of polycystic ovary syndrome 2023
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Nov 2030
12 May 2026 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.