Rectal prolapse
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 29 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A rectal prolapse is when part of the rectum (the last part of the bowel) drops or slips through the anus.
A rectal prolapse causes a lump to stick out of your back passage (anus) and this can become quite painful. Although the lump can pop in and out at first, later on it can stay out all the time, especially when you stand up. This can cause problems with daily activities that involve walking or standing for any length of time.
In this article:
Video picks for Anal and rectal problems
Continue reading below
What causes rectal prolapse?
Anything that increases the pressure inside your tummy (abdomen) can make you more likely to develop a rectal prolapse. This can include:
Chronic constipation and straining.
Diarrhoea.
Straining to pass urine due to a swollen prostate gland.
Pregnancy.
Persistent cough.
Damage to the back passage (anus) or pelvis from previous surgery.
Damage to the muscle on the floor of the pelvis.
Infections of the bowel with certain types of microbes called parasites (such as amoebiasis and schistosomiasis).
Diseases of the nervous system such as multiple sclerosis.
Damage to the nerves from back surgery, a slipped disc, or an accident injuring the pelvic nerves.
Rectal prolapse in children
In children, rectal prolapse occurs in:
Hirschsprung's disease (a rare condition that can cause poo to become stuck in the bowel).
Malnutrition (not having enough food, not eating the right food, or not being able to absorb the nourishment from food).
Click on the links for more information about the highlighted conditions.
Prolapse of the bladder or womb (uterus) doesn't cause rectal prolapse but is sometimes associated with it.
Rectal prolapse symptoms
Back to contentsA lump sticking out
The first thing you will notice is a lump sticking out of your back passage (anus). In the early stages this will only appear after you've had a poo or strained to pass a motion. It tends to disappear when you stand up.
Later on, you may notice the lump in other circumstances that involve straining, like coughing or sneezing.
Eventually, the lump may be noticeable most of the time and interfere with day-to-day activities such as walking.
You may have to push the lump back with your hand.
A doctor examining the prolapse will see a lump sticking out which has concentric rings around it. An ulcer on the prolapse may also be seen.
Rectal Prolapse Pictures
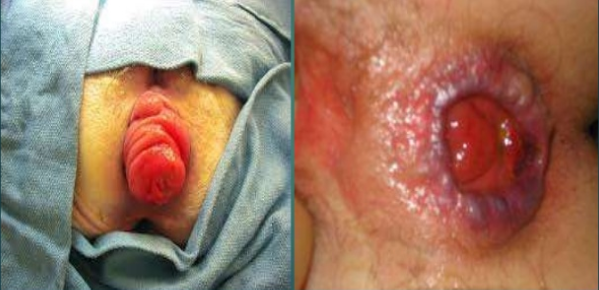
Full rectal vs mucosal prolapse.
Dr Hassan Mahmud, via SlideShare.net
Other symptoms
You may notice pain, constipation and bleeding from the last part of your bowel (the rectum).
The muscles around the anus (anal sphincter) may become weak, allowing a little bit of poo to escape (faecal incontinence). This can also happen with slime (mucus) produced by the bowel wall.
Continue reading below
How common is a rectal prolapse?
Back to contentsNo-one knows how common rectal prolapse is because people often have it without reporting it to their doctor. However, it is known to happen most frequently in elderly people. Women seem to be more prone to it than men.
It is occasionally seen in children, especially from the ages of 1 to 3 years.
What else looks like rectal prolapse?
Back to contentsA prolapsed intussusception
An intussusception occurs when a section of bowel folds into the next section, a bit like the way a telescope folds up. Sometimes the folded bowel pokes outside the back passage (anus) and looks like a rectal prolapse.
A rectal polyp
A rectal polyp is a thickening of the lining (mucosa) of the bowel that comes to resemble a finger-like structure growing out of the side wall of the gut. If it pokes outside the anus it can resemble a rectal prolapse.
A haemorrhoid
What we know as a pile is a large vein that usually develops from straining whilst going to the loo. This is yet another condition that can look like a rectal prolapse if it pokes outside the anus.
Rectal Prolapse and Haemorrhoid Pictures

Difference between rectal prolapse and haemorrhoids.
Dr Hassan Mahmud, via SlideShare.net
Continue reading below
Do I need any tests for rectal prolapse?
Back to contentsIt's usually easy to tell if you have piles (haemorrhoids) rather than a rectal prolapse because a prolapse has concentric rings around the outside, whereas piles don't.
You may need a barium enema (an X-ray exam of the lower bowel) to check that you haven't got any other bowel conditions. Instead of, or as well as this, you may be offered a colonoscopy (an examination in which a colonoscope - a thin flexible tube containing fibre-optic channels) is passed through your anus and into the lower part of your bowel (the colon).
A proctosigmoidoscopy (an examination using a non-flexible scope) is used to check the rectum and anus for ulcers which sometimes occur with rectal prolapse.
Anal physiology tests - these sound complicated but are basically ways of examining your bowel movement and how your bowel works. They include X-ray pictures while your bowel is emptying (defecography), a test to check the pressure inside your bowel (anorectal manometry) and checks to test how well the muscles and nerves of the area are working. All this information is useful to diagnose rectal prolapse, especially if you are going to have surgical treatment.
Other tests may be suggested, depending on what conditions the doctor wants to rule out. For example, a sample of your poo may need checking for infection or your child may need a sweat test to rule out cystic fibrosis.
Rectal prolapse treatment
Back to contentsSometimes a rectal prolapse can be treated without an operation, especially for very young children or if the prolapse only involves the lining of the rectum (partial prolapse). Otherwise, there are a variety of operations that can be used to treat rectal prolapse.
Treatment without surgery
A prolapse which is small and/or has only recently occurred can sometimes be pushed back using pressure from your hand. If doing this is painful, a doctor may be required to do this after giving you a sedative and a local anaesthetic injection to numb the area.
Make sure you sort out any underlying cause such as constipation or diarrhoea.
If the prolapse cannot be pushed back you will need the attention of a surgeon.
A partial prolapse (in which it's only the lining of the bowel that pops out) can usually be treated without surgery although sometimes the extra tissue needs to be trimmed off.
In children, the prolapse can usually be gently pushed back using a lubricant gel. You need to make sure your child has a high-fibre diet and doesn't strain when they go to the loo. Sometimes a laxative is required. Very occasionally an injection that shrinks tissue (a sclerosant) has to be given.
Most elderly people can cope by pushing the prolapse back themselves. However, sometimes a rubber ring is inserted under the skin to keep the prolapse in place. This is not very successful as it is often too tight (causing constipation) or too loose (causing the prolapse to poke out again).
Rectal prolapse surgery
Back to contentsThere are many different types of rectal prolapse surgery and the choice will depend on age, severity of the rectal prolapse, and general health.
Different types of surgery for adults
These include:
If your prolapse can't be pushed back and the blood supply has been cut off, that is a medical emergency and you will need emergency surgery. This involves removing the prolapse and part of the lower bowel (a rectosigmoidectomy).
A prolapse involving just the lining (mucosa) of the bowel is treated by removing the excess mucosa. This is basically identical to surgery for a pile (haemorrhoidectomy). Staples are sometimes used instead of conventional cutting with a scalpel.
Abdominal surgery involving opening the tummy. The basic procedure is called a rectopexy, which involves placing the lower part of the bowel (the rectum) back into its original position and fixing it so it doesn't slip down again. Various methods are used to prevent slippage, including sutures, staples, slings and shortening the stretched bowel. Surgeons can also use a laparoscope - a thin telescope with a light source - for some of these procedures. The instrument is passed through a small hole in the tummy, resulting in a smaller scar than you would get with conventional surgery and usually a shorter hospital stay.
Rectal prolapse repair through the area around the anus. This is called a perineal rectosigmoidectomy. Variations include:
The more commonly performed form of this repair is known as the Altemeier procedure. The surgeon pulls the rectum through the anal canal and anus, and removes the prolapsed portion of the rectum. The remaining portion of the rectum is then re-joined to the lower part of your large intestine.
Another method for repairing a rectal prolapse through the perineum is called the Delorme procedure. The surgeon removes the lining of the rectum and folds the muscular layer to shorten the rectum.
Surgery for children
This is usually reserved for children aged under 4 years who have failed to respond to non-surgical treatment for more than a year.
Surgery may also be used where the prolapse keeps coming back, becomes painful or where ulcers or bleeding develop.
Lots of different methods are used including:
Injections to cause scarring around the rectum.
Insertion of a sling to support the rectum.
Use of mesh gauze to pack around the rectum and the use of a hot probe called a cautery.
Opening the tummy (abdomen) to reposition the rectum.
Placing a suture inside the rectum so that scar tissue sticks it to the tail bone (the sacrum).
As with adult surgery, some of these techniques are now being done through a laparoscope.
What is the best treatment for me?
Back to contentsStudies suggest that there is no difference in success rate whichever surgical procedure is used. Your surgeon will discuss the best option, taking on board:
Your age.
General health.
Previous experience with anaesthetics.
How long you have had your prolapse.
In general:
Young fit people are better off having a procedure through the tummy (abdomen).
Older people may be more suited to perineal operations which can be done under local anaesthetic.
There's more of a chance of the prolapse coming back but less risk to your health if you're a bit frail.
Is a rectal prolapse dangerous?
Back to contentsRisk factors include:
Ulcers in the lining (mucosa) of the lower part of the bowel (the rectum).
Death of tissue (necrosis) of the wall of the rectum.
Bleeding and breakdown (dehiscence) of tissue where two bits of bowel have been stitched together. These are the most common complications after surgery.
What is the outlook for rectal surgery?
Back to contentsThe outlook (prognosis) will depend on your age, on whether you have any untreatable causes for the prolapse and on the state of your general health.
Most people can return to their normal activities within 4 to 6 weeks, with no long-term restrictions after prolapse surgery.
About 1 in 10 children who have a rectal prolapse will continue to have it when they grow up, especially if they are aged over 4 years when they first develop it.
Patient picks for Anal and rectal problems

Digestive health
Anal fistula
An anal fistula is usually caused by an infection near your back passage (anus) that causes a collection of pus (abscess) in the nearby tissue. When the pus drains away, it can leave a small channel (fistula) behind. An anal fistula may also be associated with certain long-term bowel conditions.
by Dr Hayley Willacy, FRCGP

Digestive health
Rectal bleeding
There are many causes of rectal bleeding (bleeding from your bottom). The severity can vary from mild bleeding (common) to a severe life-threatening bleeding (uncommon). If the bleeding is heavy or if you have black stools (faeces) - older blood due to a bleed from high up in the gut - then see a doctor immediately or call an ambulance. However, rectal bleeding is usually a mild bleed. In this situation, make an appointment with your doctor so that the cause can be found.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Murphy PB, Wanis K, Schlachta CM, et al; Systematic review on recent advances in the surgical management of rectal prolapse. Minerva Chir. 2017 Feb;72(1):71-80. doi: 10.23736/S0026-4733.16.07205-9. Epub 2016 Oct 6.
- Bordeianou L, Hicks CW, Kaiser AM, et al; Rectal prolapse: an overview of clinical features, diagnosis, and patient-specific management strategies. J Gastrointest Surg. 2014 May;18(5):1059-69. doi: 10.1007/s11605-013-2427-7. Epub 2013 Dec 19.
- Rentea RM, St Peter SD; Pediatric Rectal Prolapse. Clin Colon Rectal Surg. 2018 Mar;31(2):108-116. doi: 10.1055/s-0037-1609025. Epub 2018 Feb 25.
- Rectal prolapse; Guy's and St Thomas' NHS Foundation Trust 2022
Continue reading below
About the author

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 28 Jun 2027
29 Jun 2024 | Latest version
2 Jun 2017 | Originally published
Authored by:
Dr Laurence Knott

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.