Pityriasis rosea
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 26 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Pityriasis rosea article more useful, or one of our other health articles.
In this article:
Continue reading below
What is pityriasis rosea?
Pityriasis rosea is an acute, self-limiting skin condition. A primary plaque ('herald patch') is followed by a distinctive, generalised itchy rash 1-2 weeks later.
The rash typically lasts for approximately 5-8 weeks. Lesions are typically oval, dull pink or tawny and appear in a 'Christmas tree' distribution, usually on the trunk and the upper arms and legs.
Causes of pityriasis rosea (aetiology)1 2
Back to contentsThe cause is unknown but it is believed to be infective in origin due to factors such as seasonal and geographical clustering.
No bacterium, virus, or fungus has been isolated as a cause but human herpesviruses 6 and 7 may play a role.
Pityriasis rosea-like drug eruptions have been associated with numerous medications, including:
Angiotensin-converting enzyme inhibitors.
Antibiotics (such as metronidazole) and antifungals (such as terbinafine).
Non-steroidal anti-inflammatory drugs (NSAIDs).
Antidepressants and anxiolytics, such as nortriptyline, bupropion and barbiturates.
Vaccines.
Lithium.
Lamotrigine.
Atenolol.
Omeprazole.
Biologics such as imatinib, adalimumab and etanercept.
Continue reading below
How common is pityriasis rosea? (Epidemiology)1 3
Back to contentsPityriasis rosea is most common in children and young adults, aged 10-35 years. It is more common in women (with a female-to-male ratio of 1.4:1).
Pityriasis rosea is rare in infants and young children and in the elderly.
Prevalence in the community has been estimated to be around 1.3%.
It occurs most often during the spring and autumn.
Symptoms of pityriasis rosea (presentation)
Back to contentsPityriasis rosea on the abdomen
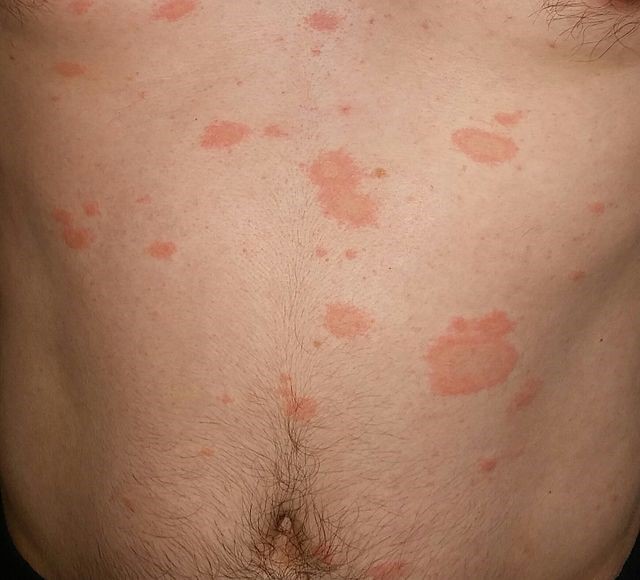
© Marekzerzan, CC BY-SA 4.0, via Wikimedia Commons
Several images of the rash of pityriasis rosea are available on the DermNet NZ site.2
Clinical features1
There may be prodromal symptoms (eg, malaise, nausea, anorexia, fever, joint pain, lymph node swelling and headache) that precede the appearance of the herald patch.
Pruritus (may be intense) is thought to occur in about half of cases.
The rash begins with a herald patch in 40-76% of cases. The herald patch measures 2-5 cm in diameter and is oval or round with a central, wrinkled, salmon-coloured area, separated from a dark-red peripheral zone by fine scales. The herald patch is usually located on the trunk but may be seen on the neck or extremities.
The secondary rash is symmetrical and localised, predominantly to the trunk, neck and proximal extremities.
The lesions of the secondary rash are small versions of the herald patch, with the two red zones separated by a scaling ring. They are distributed in a 'Christmas tree' pattern.
In some cases, the herald patch is either absent or confluent with the other lesions. In others, there are multiple herald patches.
Variant presentations include peripheral distribution of the rash; facial involvement may be seen in children. Skin lesions may also be large, urticarial, vesicular, pustular, and purpuric, and resemble erythema multiforme.
Hypopigmentation and hyperpigmentation of affected skin may follow the inflammatory stage.
Oral lesions are rare but may occur - eg, erythematous plaques and ulcers.
Continue reading below
Differential diagnosis3
Back to contentsPolymorphic eruption of pregnancy.
Secondary syphilis.
HIV seroconversion (usually associated with a febrile, flu-like illness).
Diagnosing pityriasis rosea (investigations)
Back to contentsDiagnosis is clinical and usually no investigations are required.
Skin biopsy is not usually advised but may be occasionally required to confirm or alter the diagnosis.
Other investigations - eg, syphilis serology - may be required to rule out other possible diagnoses.
It is not uncommon for the herald patch to be diagnosed as tinea, with the actual diagnosis of pityriasis rosea only becoming apparent after the more generalised rash appears.
Management of pityriasis rosea1 3
Back to contentsPityriasis rosea is a self-limiting disease. Treatment is symptomatic and only if required. Reassure the person that the rash will disappear on its own but that it may take a few weeks to do so. Explain that new areas may be affected by the rash for up to six weeks. Also reassure that it is not contagious.
There is no convincing evidence of efficacy for any treatments used. For pruritus the following may be tried:
Emollients.
Topical corticosteroids, with the potency depending on the severity of the itch.
Topical menthol.
A sedative antihistamine at night such as hydroxyzine or chlorphenamine.
Referral
Refer to a dermatologist if:
The rash persists for more than three months.
Itch is severe.
Diagnosis is not clear.
Although the evidence of efficacy is not yet clear, phototherapy is often used in secondary care.
Oral aciclovir has been shown to be effective in terms of rash improvement. Erythromycin may be effective in improving the itch.4
Pregnancy 356
There is believed to be a risk of viral reactivation in pregnancy, due to the change in immune response. Consequently, there appears to be an increased risk of miscarriage for women who develop pityriasis rosea in early pregnancy. The absolute risk is low and most of the data comes from small studies; women can be reassured that the vast majority who get pityriasis rosea during pregnancy will have no significant complications. Despite this reassurance, the NICE CKS page suggest that we discuss pityriasis rosea urgently with secondary care, and the NHS website tells women to call their maternity team if they notice a new rash. It would therefore be prudent to discuss a suspected case with obstetrics.
Prognosis3
Back to contentsThe eruptions are self-limiting and usually disappear gradually in 2-12 weeks, without any treatment.
However, they can take up to five months to disappear in some cases.
New skin lesions may continue to appear in the first 2-6 weeks.
After lesions have disappeared, there may be some darkening or lightening of the affected skin for several months.
It typically heals without scarring.
Most people who have pityriasis rosea will not have another attack during their lifetime; the risk of recurrence is 2-3%.
Further reading and references
- Eisman S, Sinclair R; Pityriasis rosea. BMJ. 2015 Oct 29;351:h5233. doi: 10.1136/bmj.h5233.
- Pityriasis rosea; DermNet NZ
- Pityriasis rosea; NICE CKS, April 2020 (UK access only)
- Contreras-Ruiz J, Peternel S, Jimenez Gutierrez C, et al; Interventions for pityriasis rosea. Cochrane Database Syst Rev. 2019 Oct 30;2019(10). doi: 10.1002/14651858.CD005068.pub3.
- Stashower J, Bruch K, Mosby A, et al; Pregnancy complications associated with pityriasis rosea: A multicenter retrospective study. J Am Acad Dermatol. 2021 Dec;85(6):1648-1649. doi: 10.1016/j.jaad.2020.12.063. Epub 2021 Jan 8.
- Wenger-Oehn L, Graier T, Ambros-Rudolph C, et al; Pityriasis rosea in pregnancy: A case series and literature review. J Dtsch Dermatol Ges. 2022 Jul;20(7):953-959. doi: 10.1111/ddg.14763. Epub 2022 May 26.
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Jan 2028
26 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free