Tuberculosis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 13 Oct 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Tuberculosis (TB) is an infection with a germ (bacterium) called Mycobacterium tuberculosis. If you have symptoms, or a doctor can find signs of the infection when examining you, this is known as active tuberculosis. If you have TB infection without any signs or symptoms, this is known as latent TB.
In this article:
Video picks for Chest and lung infections
Continue reading below
How common is tuberculosis?
Tuberculosis (TB) is common in developing countries. The death rate from TB is falling but it still causes about two million deaths per year worldwide. The main risk factors for TB in the developing world are:
Poor nutrition.
Poor housing.
Poor general health.
Insufficient healthcare.
AIDS (TB is common in people with AIDS).
The number of people with active TB was at an all-time low in the UK in the early 1980s but the number of cases has since increased. This was probably due to a combination of factors. These include:
An increase in poverty.
The ageing population.
Immigration from areas where TB is common.
More people travelling to areas in the world where TB is common.
AIDS.
In the last four years, however, the rate has started to fall. It is thought this is due to several factors, including tackling poor housing and poverty and identifying and treating TB brought into the UK by immigrants. In England in 2015, just under 6,000 new cases were reported. Rates of TB vary in different parts of the UK, with some London boroughs having very high rates.
Country-specific information on the risk of TB and vaccination can be found in our Travel advice by country page.
Who develops tuberculosis?
Back to contentsAnyone can have TB. The risk is increased where one or more of the following apply:
Close contacts of a person who has active TB in the lungs (living in the same household, or spending a lot of time with that person).
If you or your family come from a country where TB is common.
Environment and poverty: rates of TB are higher among homeless people, prisoners, in large cities and in more deprived areas.
A poor immune system: for example, due to HIV infection, immune-suppressing treatment, or alcohol or drug dependency.
Malnutrition: poor nutrition and lack of vitamin D are linked to TB.
Age: babies, young children and the elderly are more susceptible to TB.
Continue reading below
How do you catch tuberculosis?
Back to contentsMost cases affect the lungs at first. TB bacteria are coughed or sneezed into the air by people with active TB disease. The bacteria are carried in the air in tiny water droplets. If you breathe in some TB bacteria, they may multiply in your lung. There are then three ways the infection may progress.
Tuberculosis scarring
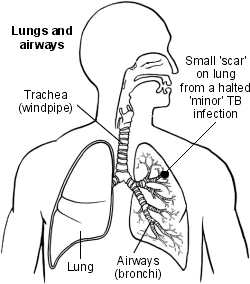
1. Minor infection with no symptoms - occurs in most cases
Most people in good health who breathe in TB bacteria do not develop active TB disease. The TB bacteria that you breathe in begin to multiply in the lung. This stimulates your body defences (immune system) into action. The TB bacteria are killed or made inactive by the immune system. There may be some mild symptoms for a short time, or no symptoms, and the infection is halted.
You are not usually aware that you have had this mild infection. A small scar on the lung may be seen on a chest X-ray. This may be the only indication of a previous TB infection.
2. Infection progressing into active TB disease - occurs in some cases
Active TB disease with symptoms occurs in some people who breathe in some TB bacteria. In these people the immune system does not win the battle and halt the invading bacteria. The TB bacteria multiply further and spread to other parts of the lung and body. Symptoms of active TB then develop about 6-8 weeks after first breathing in some bacteria.
TB infection which progresses to active disease can occur in anybody who is infected with TB bacteria. However, it is more likely if you are already in poor health. For example, it is common in malnourished children in developing countries. Newborn babies are also more at risk of active TB.
3. Secondary (reactivated) infection causing active disease
Some people develop active TB months or years after a minor TB infection had been halted. The body's immune system at first stops the bacteria from multiplying (as above). However, not all the bacteria may be killed. Some bacteria may be 'walled off' in the scar tissue of the initial minor infection. They are stopped from multiplying by the immune system. They do no harm but can remain inactive for many years. The inactive TB bacteria may later start to multiply and cause active TB if the body's immune system becomes weaker for some reason. A weak immune system and re-activated TB are more likely to occur if you:
Are elderly or frail.
Are malnourished.
Have diabetes.
Take steroids or immunosuppressant medication.
Have kidney failure.
Are alcohol-dependent.
Have AIDS.
What other tuberculosis bacteria exist?
Back to contentsAs mentioned above, the disease that we call 'tuberculosis', or 'TB', is caused by a bacterium called Mycobacterium tuberculosis. Other bacteria in the same family are called Mycobacterium bovis and Mycobacterium africanum. They are rare causes of infection in the UK. Mycobacterium bovis used to be more common, as it is passed on from contaminated unpasteurised milk or from infected cattle (now rare in the UK). Treatment for these infections is mostly similar to that for standard TB.
There are various other bacteria in the mycobacterium family which are called atypical mycobacteria. Most of these do not cause infection. However, they sometimes cause serious infection in people whose immune system is not working very well. (For example, some people who have AIDS.) Treatment is with long courses of antibiotics.
Continue reading below
What are the symptoms of tuberculosis?
Back to contentsCough lasting more than three weeks is often a first symptom of active tuberculosis (TB). It can start as a dry irritating cough. It tends to continue for months and get worse. In time the cough produces a lot of phlegm (sputum), which may be bloodstained.
Other common symptoms are a high temperature (fever), sweats, feeling unwell, weight loss, pains in the chest, and poor appetite. You may become breathless if the infection progresses and damages the lungs. If left untreated, complications often develop, such as fluid collecting between the lung and the chest wall (pleural effusion). This can make you very breathless. If the TB gets close to a blood vessel in the lung then you may cough up blood.
TB infection sometimes spreads from the lungs to cause infection in other parts of the body. Depending on which part of the body is affected, various symptoms may then occur:
Lymph glands - you may have a swollen gland or glands anywhere in the body. If the swollen glands are in the neck, armpit or groin then you may see or feel them.
Gut and tummy (abdomen) - the TB may cause tummy pain or swelling, or poor digestion of food with diarrhoea and weight loss.
Bones and joints - TB can get into a bone or joint, causing bone pain (for example, in the spine) or pain and swelling in a joint.
Heart - TB sometimes causes inflammation around the heart, with chest pain or shortness of breath.
Kidneys and bladder - if these are infected, you may have pain in the side (loin), or pain when passing urine.
Brain - TB can cause meningitis, with symptoms such as:
Headache.
Feeling sick (nausea).
Being sick (vomiting).
Fits (convulsions).
Drowsiness.
A change in behaviour.
Skin - TB can cause certain rashes, including erythema nodosum - a red, lumpy rash on the legs - or lupus vulgaris which gives lumps or ulcers.
Spread to many parts of the body - this is called miliary TB, and can affect many organs, including lungs, bones, liver, eyes and skin.
How contagious is tuberculosis?
Back to contentsA person with active tuberculosis disease in the lungs will cough and sneeze TB germs (bacteria) into the air, which can infect others. To catch TB you normally need close and prolonged contact with a person who has active TB in the lungs. So, the people most likely to be infected will be those in the same house or same family. In the UK, if someone is diagnosed with TB then health workers will arrange TB tests for their close contacts.
How is tuberculosis diagnosed?
Back to contentsDiagnosing tuberculosis (TB) is sometimes straightforward, but the diagnosis may be more difficult for some people. In general, the diagnosis is made by looking at the clinical picture (your symptoms and a doctor's examination), combined with the results of certain tests. To start with, you will usually have a chest X-ray and/or a tuberculin skin test, followed by phlegm (sputum) tests.
Chest X-ray
A chest X-ray usually shows any active lung TB. It may also show healed or inactive TB.
Tuberculin skin testing (Mantoux test)
This test shows whether you have been in contact with TB germs (bacteria) at some point in your life. However, it cannot prove you have a current active infection. The tuberculin is made from part of the TB bacterium. It is injected into the skin. The injection site is examined a few days later.
A positive reaction is a red inflamed area of the skin. This means that you have an active infection, or have had a previous infection, or you have been immunised in the past with BCG. (BCG is the vaccine used to prevent TB.) A negative skin reaction tends to rule out TB. However, the result may be falsely negative for some people with TB infection - for example, if you have severe TB, if you have AIDS or a poor immune system, or in young children in the early stages of infection.
Sputum tests
If the chest X-ray or tuberculin test results suggest that TB is possible, the next test will be to look for TB bacteria from the lung. This is done by sending samples of sputum to the laboratory.
A smear of the sputum is examined in a laboratory, under a microscope using a special dye (stain) to show the TB bacteria. The results are obtained quite quickly, usually within a few days.
Another test for the sputum samples is a culture test. This involves growing (culturing) the TB bacteria in the laboratory. This can take several weeks because TB bacteria grow slowly. There are two important reasons for doing this test. First, to detect TB bacteria that may not be found on the smear test. Second, the culture test can check whether the TB bacteria are resistant to any antibiotic medicines. (Antibiotic resistance is explained below.)
It's considered that sputum results should be awaited before treatment is started, unless the illness is thought to be life-threatening.
It is sometimes difficult to obtain sputum for the test (for example, with children). A sample of fluid from the stomach (gastric washings) may then be used instead.
Other tests
Other possible tests for suspected TB are:
A blood test called an interferon gamma test. This can be helpful if the tuberculin skin test result was unclear. The advantage of this test is that the result is not affected by the BCG vaccine.
An HIV test should be offered. This is because TB is more common in people who have HIV, and treatment may be needed for both conditions.
A computerised tomography (CT) scan or a magnetic resonance imaging (MRI) scan may be used to look for TB in internal organs. For example, a brain scan is useful if TB meningitis or TB infection in the brain is suspected.
Samples from other parts of the body: TB may be suspected in organs other than the lung. It may then be helpful take a sample of tissue or fluid from the affected part of the body. This sample can then be tested in the laboratory by the same methods used for sputum samples (above). For example, samples can be taken from urine, from lymph glands near the skin, or from the lung. A test called a lumbar puncture samples fluid near the spine, if meningitis is suspected.
New tests are being developed. Some are similar to the culture test above, but give faster results. Other tests help identify bacteria which are resistant to antibiotics.
Do family, friends or colleagues need tests?
Back to contentsIf you have TB of the lung or voice box, anyone who comes into close and prolonged contact with you needs testing. The usual tests available for contacts are a chest X-ray and/or tuberculin skin test (Mantoux test). If these show possible TB, other tests may need to be done.
It may be difficult to diagnose babies and children under the age of 2 years. They may be put on treatment whilst awaiting results of tests.
What is the treatment for tuberculosis?
Back to contents'Normal' antibiotics do not kill tuberculosis (TB) germs (bacteria). You need to take a combination of special antibiotics for several months. Standard treatment in the UK is usually for six months. First, it involves a combination of four antibiotics that you take for two months. These are isoniazid, rifampicin, pyrazinamide and ethambutol. This is followed by continuing with rifampicin and isoniazid for a further four months. The treatment plan may be different, depending on what type of TB you have and which part of the body is affected.
If treatment fails, it is often due to not taking medication properly and regularly. It is vital that you follow the instructions about medication. Even if you feel much better in a few weeks (as many people do), you must finish the full course of treatment.
Attending follow-up appointments is important. This is to check that your TB is responding to the treatment and to check for any side-effects of treatment.
Why is important to take the full course of treatment?
The TB bacteria in the body are more difficult to get rid of than 'ordinary' bacteria. Only a long course of treatment can fully clear TB bacteria from the body. If you do not take the full treatment then the following problems often occur:
You may remain infectious to other people.
You may not be cured. You may feel better at first but some TB bacteria may stay in your body. These can reactivate at a later time and make you very ill.
If the original infection is only partly treated, the bacteria can become resistant to antibiotics (explained below). The TB then becomes more difficult to treat.
Are there side-effects of tuberculosis treatment?
Back to contentsThe medicines used to treat TB have a good safety record. Sometimes side-effects occur. If one does, see a doctor urgently, so that your treatment can be adjusted or changed to a different antibiotic.
You can read the leaflet which comes with the medicine packet for a list of possible side-effects. Some important things to know are:
Liver problems. You will have blood tests to monitor your liver function. It is common to get mildly abnormal liver tests when taking TB treatment. This doesn't always mean that the treatment needs to be changed. Symptoms of liver problems are:
A yellow tinge to the skin and eyes (jaundice).
A high temperature (fever).
Feeling sick (nausea).
Itching.
Feeling generally more unwell.
If you have any of these, stop the tablets and see a doctor urgently.
Vision changes (if taking ethambutol). Early symptoms are slight loss of vision or loss of colour vision. If you notice any loss of vision, stop the ethambutol and see a doctor urgently. Vision can recover fully if the ethambutol is stopped quickly. You will need to have a sight test before you start taking ethambutol.
Nerve problems (neuropathy) if taking isoniazid. This can cause numbness and tingling in the arms and legs. It can be helped by taking an extra vitamin (pyridoxine) - which is sometimes prescribed together with the isoniazid.
Rifampicin makes your tears and urine orange-coloured. This is normal.
TB medication can affect other medicines, including the contraceptive pill. Tell the TB clinic about all your medication, so that it can be taken into account when deciding about treatment.
How do I access tests and treatment for tuberculosis?
Back to contentsTests and treatment for TB are free to everyone in the UK - even if you are not a UK resident.
Your doctor will refer you for tests if he or she suspects that you have TB. This is usually to a local TB or chest clinic. In addition, there are also mobile X-ray units in London, which provide chest X-rays as an initial test for TB. The mobile units visit prisons, shelters for the homeless, and refugee centres.
Treatment is normally from a TB clinic. Most hospitals in the UK have a chest clinic or TB clinic with staff experienced in treating TB. Your GP can help with prescriptions.
Most people with TB can have treatment at home. Hospital admission is not usually necessary unless:
You are quite ill.
The treatment is complicated for some reason.
You have difficult circumstances such as homelessness.
Some people find it hard to remember to take their medication regularly. If so, you may be offered 'observed treatment', where a health worker sees you for each dose. The treatment schedule is adjusted so that medication is taken three times weekly instead of daily.
Drug-resistant TB
Some people have TB bacteria which are 'resistant' to certain antibiotics - meaning that the bacteria are not killed by that antibiotic. This means that other antibiotics have to be used instead, to cure the TB. So antibiotic resistance can make the TB more difficult to treat and more dangerous to others who are infected. Difficulty of treatment is increased if the bacteria are resistant to more than one antibiotic. This is called multidrug-resistant (MDR) TB. If the bacteria are resistant to more than three antibiotics, this is called extensively drug-resistant TB.
Drug-resistant TB can be due to not taking a full course of treatment, or to catching TB with bacteria that are already resistant.
If you have (or may have) drug-resistant TB then extra precautions are needed to prevent the infection spreading to others. Your health worker will advise about this. You will need different antibiotics from the standard treatment above, with advice from a specialist.
TB and HIV infection
TB is more common in people with HIV infection. It may be more difficult to diagnose, because the symptoms and test results may not be typical. Also, treatment can be more complex because the TB medication and the HIV medication can interfere with each other. Specialist advice may be needed.
Sometimes, if you have TB and then start antiviral treatment for HIV, the TB symptoms can get worse for a while. This happens because the immune system gets stronger and produces a reaction to the TB infection.
Steroid treatment
Steroid treatment (prednisolone) is recommended as an additional treatment for some forms of TB. If there is TB in the brain (meningitis), or TB around the heart (pericarditis), then a course of prednisolone can help prevent complications.
Are precautions needed to stop others catching tuberculosis?
Back to contentsIf you have active tuberculosis (TB) in the lung, you can infect other people until you have taken the correct treatment for two weeks. After that, normally you will not be infectious (but you should continue with the treatment). During the first two weeks of treatment, you will be advised to stay at home (or stay in your room if in hospital) and avoid contact with anyone who has poor body defences (immune system). This includes people with HIV, those taking chemotherapy medicines, or young babies.
Sometimes extra precautions are needed - for example, if your TB is thought to be very infectious or resistant.
Do family, friends or colleagues need tests?
Back to contentsHousehold members and close regular contacts of a person with TB of the lungs (pulmonary TB) or voice box (laryngeal TB) may be advised to have tests. Close regular contacts may include colleagues, friends, classmates, teachers and non-teaching school staff, depending on the situation and on how infectious your TB is. The usual tests for contacts are a chest X-ray and/or a tuberculin test (Mantoux test). If these show possible TB then further tests can be done to look for active TB.
Special rules apply for babies and young children aged less than 2 years who have been in contact with active TB. Diagnosing TB in young children is difficult. In the early stages, the infection may not show up on tests. But young children are vulnerable to TB (they can get a severe infection). Therefore, they may be started on some treatment (such as isoniazid) for several weeks. This helps to prevent a severe infection whilst having further tests to see if TB is present.
What is the outlook if you have tuberculosis?
Back to contentsWith treatment, most people make a full recovery. If left untreated, about half of people with active TB eventually die of the infection. TB bacteria multiply quite slowly compared to most other bacteria. Therefore, active TB tends to cause an illness that slowly gets worse. Some people survive without treatment and may even fully recover. The outlook (prognosis) tends to be worse where the TB is more difficult to treat. For example, with HIV/AIDS, other serious illness, or extensively drug-resistant TB.
How can tuberculosis be prevented?
Back to contentsTB is both preventable and treatable. It is a tragedy that it remains one of the biggest killers worldwide. Relieving poverty, better nutrition and prompt treatment of TB are the most important ways of reducing TB worldwide. Having the TB vaccination also helps.
Who should have screening tests for tuberculosis?
Back to contentsA 'screening test' for TB means testing someone who is well, with no symptoms, for TB. The tests used for screening are a chest X-ray and/or a tuberculin test. Sometimes an interferon gamma blood test is used as well. In the UK, screening is currently recommended for:
Close contacts of people with active TB (as above).
People newly arrived in the UK from countries with high rates of TB.
People at risk due to their job - for example, healthcare workers, prison staff, etc.
Homeless people living on the street or in hostels.
Patient picks for Chest and lung infections

Chest and lungs
Acute bronchitis
Acute bronchitis is a common chest infection that causes inflammation of the airways. It is usually caused by viral infections and often gets better on its own within a few weeks. See a doctor if symptoms don't improve or you have trouble breathing. This leaflet explains the symptoms to look out for and how to manage them.
by Dr Toni Hazell, MRCGP

Chest and lungs
SARS and MERS virus
Severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS) are viral infections. Both infections can cause very serious illnesses that particularly affect the lungs. SARS caused many infections, especially in Asia, in 2002-2004 but was not heard of for some time. A SARS-CoV-2 (COVID-19) outbreak emerged in Wuhan, China in December 2019. This spread rapidly and was declared a global pandemic in 2020. MERS was first recognised in the Middle East in 2012. Most of the initial infections were in the Middle East. However, by February 2018, the World Health Organization (WHO) had reported cases in many other countries.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Tuberculosis (TB); World Health Organization
- Tuberculosis (TB) and other mycobacterial diseases: diagnosis, screening, management and data; United Kingdom Health Security Agency
- Tuberculosis; NICE Guideline (January 2016 - last updated September 2019)
- Tuberculosis; NICE CKS, January 2019 (UK access only)
- Koegelenberg CFN, Schoch OD, Lange C; Tuberculosis: The Past, the Present and the Future. Respiration. 2021;100(7):553-556. doi: 10.1159/000516509. Epub 2021 May 25.
- Tuberculosis; British National Formulary (BNF)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Oct 2027
13 Oct 2022 | Latest version
20 May 2014 | Originally published
Authored by:
Dr Colin Tidy, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.