Contraceptive implant
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 10 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Long-acting reversible contraceptivesContraceptive injectionIntrauterine contraceptive deviceLevonorgestrel intrauterine device
A contraceptive implant is a device that is put under the skin in order to offer you an even dose of contraception without you having to take a daily pill.
In this article:
Video picks for Long-acting reversible contraceptives
Continue reading below
What is the contraceptive implant?
A contraceptive implant is a small, flexible rod about the size of a matchstick. The implant contains a progestogen hormone which provides contraception (prevents pregnancy) without you having to take a daily pill.
The rod is put under the skin on your arm. The only contraceptive implant currently available in the UK is Nexplanon® (there are other devices available elsewhere in the world).
Nexplanon® is 40 mm long and 2 mm wide. That is, about the size of a normal matchstick.
Effectiveness
Back to contentsOne of the benefits of the implant is that it is the most effective contraceptive (birth control) method available. The contraceptive implant is over 99% effective. Only around 1 in 2,000 sexually active women using the implant will become pregnant whilst using it. Some women may appear to have become pregnant whilst using the implant, but when things are checked more carefully, they were actually pregnant before it was put in.
Continue reading below
Timing of fitting
Back to contentsIf an implant is put in during the first five days of your period, you are protected against pregnancy immediately. If an implant is put in at any other time during your cycle, you are not protected until seven days have passed. You will need to use additional contraception if you wish to have sexual intercourse during this time.
You should only have an implant put in if it is certain that you are not already pregnant. You may still need to use contraception such as condoms to protect against sexually transmitted infections (STIs), for example if you are in a new relationship or have any concern that you might be at risk of an STI.
How does the contraceptive implant work?
Back to contentsPlaylist: Contraceptive Implant
4 videos
How does the implant work on the body?
Dr Rosemary Leonard MBE, MRCGP
How does the implant work on the body?
Dr. Rosemary Leonard MBE, MRCGP

How long after the implant is inserted can you be sexually active?
Dr. Rosemary Leonard MBE, MRCGP

Can you get pregnant when you have the implant?
Dr. Rosemary Leonard MBE, MRCGP

Can you get the implant removed early?
Dr. Rosemary Leonard MBE, MRCGP
The progestogen hormone in the implant is called etonogestrel. It is released into the bloodstream at a slow, steady rate.
The contraceptive implant works mainly by stopping the release of the egg from the ovary. It also thickens the cervical mucus which forms a plug in the neck of the womb (cervix). This stops sperm getting through to the womb (uterus) to fertilise an egg.
It also makes the lining of the womb thinner. This means that if an egg were to fertilise, it would not be likely to be able to attach to the womb (implantation).
In order for you to get pregnant you need all of these things to be working (ovulation, sperm getting through the cervix, and implantation). The contraceptive implant blocks all three stages.
Continue reading below
How long do contraceptive implants last?
Back to contentsThe contraceptive implant is fully effective for three years, but it stops being effective if it is removed. After three years, if you want to continue using this method of contraception, you will need a new implant. It is a type of contraception called a LARC (long-acting reversible contraception).
How is the contraceptive implant put in?
Back to contentsThe contraceptive implant is about the size of a matchstick and is placed under the skin of the inner side of your upper arm. A trained doctor or nurse will put the implant in.
An injection of local anaesthetic is used to numb the skin.
A special device is used to place the implant under the skin. The wound is dressed and will soon heal.
The procedure only takes a few minutes. The area around the implant may be bruised and tender for a few days.
How is the contraceptive implant taken out?
Back to contentsA trained doctor or nurse must take your implant out. The procedure is similar to putting the implant in.
An injection of local anaesthetic is used to numb the skin.
A tiny cut is made in your skin the implant is gently pulled out.
A dressing will be put on your arm which should be left in place for a few days. You may also have Steristrips® (paper stitches)
Implanon v
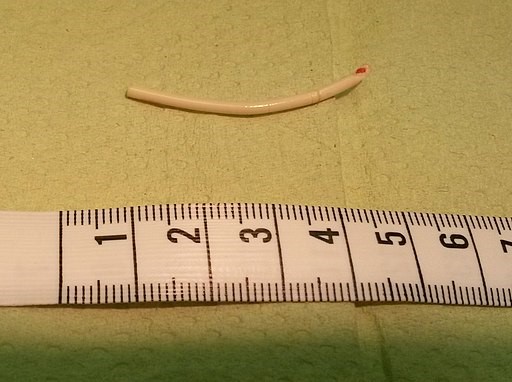
© Vera de Kok, CC BY-SA 4.0 , via Wikimedia Commons
Occasionally, an implant is difficult to feel under the skin, in which case you may be referred to a specialist centre to have it removed with the help of an ultrasound scan. If you want to carry on using an implant, the doctor or nurse can put a new one in at the same time, usually in the other arm. If you do this there will be no break in your contraceptive protection.
The implant can be taken out at any time if you request removal. It loses its effect immediately after being removed.
When should the contraceptive implant be put in?
Back to contentsYou can have an implant fitted at any time in your menstrual cycle if it is certain that you are not pregnant.
If the implant is put in during the first five days of your period you will be protected against pregnancy immediately.
After day 5 and if you haven't had unprotected sexual intercourse (UPSI) since your last period, the implant can be inserted immediately but you should avoid sexual intercourse or use a barrier method of contraception (such as condoms) for 7 days.
If you have had unprotected sexual intercourse since your last period you may need a pregnancy test and emergency contraception. You should discuss this with your clinician.
If you have recently had a baby the implant can be put in at any time after the birth. If the implant is inserted on or before day 21, your contraceptive protection starts straightaway. (You can't become pregnant in the first 21 days after delivery, so as long as you have it inserted any time up to day 21 you are protected.)
If it is fitted later than this and you have had unprotected sexual intercourse, you may need a pregnancy test and emergency contraception. You should discuss this with your clinician.
If you have had a termination of pregnancy or a miscarriage the implant can be put in at the same time, or in the first five days, and is effective immediately.
It is sometimes possible to have an implant fitted even if you aren't certain that you are not pregnant. For example, if you have had unprotected sex and it is too early for a pregnancy test to be reliable. This is called quick starting. If you quick start the implant, it is important that you do a pregnancy test at least three weeks after your last episode of unprotected sex. This test would be bought from a chemist or supermarket and not usually supplied by the GP. Your doctor or nurse will talk you through the pros and cons of quick starting.
Side-effects of the contraceptive implant
Back to contentsMost side-effects caused by the contraceptive implant occur when you first start using the implant. They are not usually severe. Of this list, changes in your period is the commonest side-effect.
The most common side-effects are:
Changes in your periods (see below).
Fluid retention and breast tenderness.
Acne: your skin may temporarily worsen, although it can also improve.
Itching or bruising after implant insertion.
Breast tenderness.
The contraceptive implant does not usually cause altered sex drive (libido), but some women who have experienced other side-effects also say that their sex drive was reduced.
Does the contraceptive implant stop periods?
Back to contentsMost women experience changes in their periods with a contraceptive implant.
Most commonly, the periods will be lighter and less regular.
Some women find that their periods stop altogether with the implant (amenorrhoea).
A few women have longer, irregular periods, which can be heavy.
Changes in your periods may settle in the first three months of using the implant, and it is not ideal to remove it due to side-effects before this time. If that doesn't happen, your doctor may prescribe extra hormones on top of the implant to try and settle the bleeding. These might be used for a short period of time, or long-term.
Does the contraceptive implant cause weight gain?
Back to contentsThere is no strong evidence that the contraceptive implant makes women put on weight.
Risks from using the contraceptive implant
Back to contentsWomen who use progestogen only contraception such as the implant have a small increased risk of breast cancer. The risk is very small - if 100,000 women aged 16 - 20 use the implant for 5 years, there will be an extra 8 cases which happen over the next 15 years. This figure increases to 265 for women aged 35 - 39 (who are also more likely to have breast cancer without an implant) - that is just under an extra 3 cases per 1000 women over 15 years.
Can I have the implant after emergency contraception?
Back to contentsLevonorgestrel. After taking levonorgestrel (Levonelle®) as emergency contraception the implant can be inserted immediately. You should avoid sex or use a barrier method of contraception (such as condoms) for 7 days. In addition you should take a pregnancy test 3 weeks or so after the time you had unprotected sex.
Ulipristal acetate. If you took ulipristal acetate (ellaOne®) the implant should be inserted 5 days after taking the tablet. You should avoid having unprotected sex or use a barrier method of contraception (such as condoms) until the implant is inserted and for 7 days after. You should also take a pregnancy test no sooner than 3 weeks after the last time you had unprotected sex.
Can a contraceptive implant be used when breastfeeding?
Back to contentsYes, an implant can be used when breastfeeding. The implant will not affect your milk production and will not harm your baby.
Although breastfeeding does slightly reduce the chance of another pregnancy, it is not a reliable contraceptive and it is possible to become pregnant whilst breastfeeding.
Can anything make an implant less effective?
Back to contentsSome medicines may make an implant less effective. This includes some medicines used in epilepsy, HIV and tuberculosis, and St John's wort (a herbal remedy often used to treat headaches, mood disturbances and premenstrual syndrome).
These medications reduce the effectiveness of the implant by increasing the rate at which your body disposes of the hormone in the blood. If you are using one of these medicines you will need to consider a different or additional contraceptive method.
The implant is not affected by common antibiotics, or by an attack of diarrhoea or being sick (vomiting).
Who should not have a contraceptive implant?
Back to contentsMost women can have an implant fitted but there are a few exceptions. You should not have a contraceptive implant put in if you think you might be pregnant, or if you don't want to use a contraceptive method that might affect your periods.
You also should not use the contraceptive implant if you currently have breast cancer. This is known as an absolute contraindication, that is you should never use the implant if you have breast cancer.
Other health conditions are relative contraindications, in which the risks of using the implant might outweigh the benefits. Your doctor or nurse can help you to understand how important any relative contraindication is, or how more than one risk might combine to affect your decision as to whether or not to use the implant.
Relative contraindications include:
Some types of severe heart or liver disease.
Past breast cancer.
Current unexplained vaginal bleeding.
A hereditary blood disorder called porphyria.
You have an increased risk of blood clots in the veins due to antiphospholipid syndrome, antithrombin deficiency or factor V Leiden.
You have previously had a deep vein thrombosis or pulmonary embolism.
You have migraines.
You have systemic lupus erythematosus.
You have gene mutations associated with breast cancer - for example, BRCA1.
You have cervical cancer.
You have experienced a stroke, angina or heart attack.
You have several risk factors for heart disease, such as smoking, high cholesterol, high blood pressure, diabetes.
You have had jaundice or itching caused by previous use of a hormonal contraceptive.
If I have a contraceptive implant, what do I do when I want to try to get pregnant?
Back to contentsIf you want to try for a baby, you need to have the implant removed. Your periods will return to normal, although it can be up to three months before you get back to your old rhythm. However, it is possible to get pregnant before you have your first period.
Start pre-pregnancy care such as taking folic acid, stopping smoking and considering any regular medication you take beforehand. You can ask your doctor or nurse for further advice.
Where can I get the contraceptive implant?
Back to contentsThe contraceptive implant has to be fitted by a specially trained nurse or doctor. This service may be offered at your local GP surgery and, if it is, how to arrange it will probably be explained on their website. Alternatively, a family planning, sexual health or community gynaecology clinic will do this for you. You can find details of services in your area in the UK online.
In the UK the contraceptive implant is free of charge.
All contraceptive services are completely confidential. You will not need an internal examination, a breast examination or a smear before you can have a contraceptive implant. In some cases you may need a pregnancy test to be certain that you are not already pregnant.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Long-acting reversible contraceptives

Sexual health
Contraceptive injection
The contraceptive injection contains a progestogen hormone. It is used to prevent pregnancy.
by Dr Caroline Wiggins, MRCGP

Sexual health
Intrauterine contraceptive device
An intrauterine device (IUD) is a small device made from plastic and copper which sits inside the womb (uterus). It is also known as the coil.
by Dr Rosalyn Adleman, MRCGP
Further reading and references
- Trussell J; Contraceptive failure in the United States, Contraception, 2011
- UK Medical Eligibility Criteria Summary Table for intrauterine and hormonal contraception; Faculty of Sexual and Reproductive Healthcare, 2016 - amended September 2019
- Contraception - Progestogen-only methods; NICE CKS, November 2024 (UK access only)
- Contraception - assessment; NICE CKS, January 2024 (UK access only)
- Progestogen-only implants; Faculty of Sexual and Reproductive Healthcare (Feb 2021 - Updated July 2023)
Continue reading below
About the author

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Jan 2028
10 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.