Hidradenitis suppurativa
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 20 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Hidradenitis suppurativa is a long-term (chronic) skin condition that leads to painful and repeated lumps of pus (boils or abscesses). The exact cause is unknown.
Suppuration means formation or discharge of pus. These areas (commonly the armpits and groin) leak pus and are difficult to heal. Eventually, scarring occurs. Treatments include antibiotic lotions or medicines, or an operation to remove the affected skin area. A newer treatment works by blocking a chemical of the immune system that causes inflammation in the body.
In this article:
Video picks for Other skin problems
Continue reading below
What is hidradenitis suppurativa?
Hidradenitis suppurativa (HS) is a long-term (chronic) inflammatory skin disease with recurrent boil-like lumps. These boils often become bigger and turn into collections of pus (abscesses). The abscesses leak pus and become difficult to heal, leading to scarring. The scarring left behind can be as unsightly as the discharging wounds
Hidradenitis suppurativa is known by several other names, which can cause confusion. These are:
Acne inversa.
Apocrine acne.
Verneuil's disease.
Apocrinitis.
Velpeau's disease.
Hidradenitis
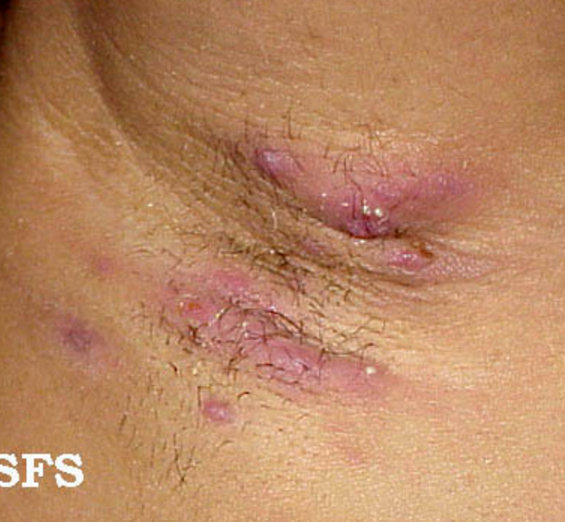
© Samuel Freire da Silva, CC BY-SA 4.0, via Wikimedia Commons
What areas does hidradenitis suppurativa affect?
The problem affects only areas of the skin containing a certain type of sweat gland, called apocrine sweat glands. Apocrine glands release an oily fluid; bacteria break down this fluid, causing body odour.
Apocrine sweat glands are mostly found in the:
Armpits.
Groin.
Breasts.
Between skin folds in the tummy (abdomen).
Between the buttocks (bum).
Women tend to develop it more commonly in the armpits, in the groin and under the breasts. Men more commonly develop disease that affects the skin around the anus.
Hidradenitis suppurativa symptoms
Back to contentsHidradenitis suppurativa usually starts with a single inflamed, boil-like, firm, raised skin lump (nodule). Sometimes this stage can result in itching but usually there is discomfort or pain.
The nodule either slowly disappears (between 10 and 30 days) or remains (persists) to become a draining (suppurative) collection of pus (abscess). Abscesses are usually very painful.
Eventually, healing occurs but the affected skin is permanently damaged, leaving deep scarring. In more severe disease the affected areas spread. Either single or multiple abscesses occur. The formation of tunnels (channels), called sinus tracts, causes the overlying skin to feel hard and lumpy (indurated).
Hidradenitis suppurativa staging
A staging system (Hurley's staging) can be used to describe the severity of the disease:
Stage 1 - here there are either single or multiple areas affected but the abscesses are separate from one another. There is no scarring or sinus tract formation.
Stage 2 - involves recurrent abscesses which can be single or multiple. Although there are sinus tracts, the affected areas are usually widely separated.
Stage 3 - generally, large areas are affected with multiple interconnected sinus tracts and abscesses.
For some people, the disease is extremely distressing and painful, with a constant succession of new nodules and abscesses forming as soon as older ones have finally healed.
Continue reading below
What causes hidradenitis suppurativa?
Back to contentsThe exact cause of hidradenitis suppurativa is unknown. It is thought to happen due to blockage of the hair follicles on the skin. When the hair follicle becomes blocked, fluid or pus inside them builds up, causing the follicle to swell and eventually burst.
The immune system reacts against this, causing the surrounding area to become inflamed or form abscesses. Sometimes, bacteria can also cause an infection, making things worse.
Things that might cause hidradenitis suppurativa include:
Genetics. Hidradenitis suppurativa tends to run in families; about one-third of people with hidradenitis suppurative have a family member who is affected.
Hormones. Excessive levels of androgens (testosterone and similar hormones) may be involved; androgen-reducing medication is sometimes used as a treatment.
Immune system problems. Over-activity of the immune system (causing inflammation) seems to be an important part of hidradenitis suppurativa; immune-suppressing medications are one of the treatments.
Overweight and obesity. This can lead to friction between skin folds, increased sweat production, and hormonal changes that make hidradenitis suppurativa more likely.
Smoking. Smoking is more common amongst people with hidradenitis suppurativa. It might make the hair follicles more likely to become blocked.
Bacteria. Bacteria (germs) on the skin can become trapped in a blocked hair follicle, causing infection and inflammation. This doesn't seem to cause hidradenitis suppurativa itself, but can make the inflammation and other symptoms worse.
Hidradenitis suppurativa is not caused by poor hygiene.
How common is hidradenitis suppurativa?
Back to contentsAround 1 in every 100 people in Europe have hidradenitis suppurativa, meaning it is quite common. Many people will have very mild problems with it.
Hidradenitis suppurativa usually affects people between puberty and middle age. It is three times more common in women than in men. It is rare in Asian people and far more common in white-skinned people or Afro-Caribbean people.
Continue reading below
Hidradenitis suppurativa diagnosis
Back to contentsThere are no tests used to diagnose hidradenitis suppurativa. The diagnosis is usually based on the typical signs and symptoms of hidradenitis suppurativa that a person may have. Sometimes, if there are signs of infection, small samples (swabs) can be taken.
Hidradenitis suppurativa is sometimes confused with other similar-looking skin conditions such as common boils, collections of pus (abscesses), skin infections and ingrowing hairs. Tests might be needed to exclude these other conditions, although they often have many other symptoms.
Your doctor might also take blood tests to make sure you are not anaemic and to monitor the level of infection or inflammation.
Hidradenitis suppurativa treatment
Back to contentsGeneral advice
Unfortunately, there is no 'cure' for hidradenitis suppurativa, although it can settle down after some time (usually years).
Try to lose weight if you are obese, and stop smoking if you smoke.
Also, the following may help relieve some of your symptoms:
Wear loose-fitting cotton clothing. Avoid tight underwear.
Wash the affected areas carefully and gently, preferably using an antibacterial or antiseptic soap or shower gel. This is to try to get rid of germs (bacteria) on the skin. (Note: it is normal to have germs harmlessly living on the skin.)
Avoid shaving affected areas, such as the underarms.
Avoid using deodorants and antiperspirants if the underarms are affected and avoid perfumes on affected areas too.
You can use a hot flannel to hold against affected areas and encourage the collections of pus (abscesses) to come to a 'point', so that they start draining. A tense hard abscess that has not burst is more painful than one where the pus is draining out.
Try to minimise heat exposure and sweating. This might mean avoiding sitting next to the fireplace, or avoiding intense exercise in the gym.
Try to minimise getting affected areas moist. Tampons may be better than sanitary pads for women.
Some people have found that certain diets help symptoms. Diets being studied are diets low in dairy products, and low glycaemic-index diets.
Medical treatment
Medical treatment means using medicines, either on the skin (topically), or by mouth. Examples of medical treatment include:
Topical antibiotics. The one usually prescribed is clindamycin. This is a lotion used twice a day on the affected area for three months.
Short courses of antibiotic tablets. These can be used when there are new abscesses. The aim is to try to stop the infection from spreading and to help the abscess heal more quickly. Generally, a short course of antibiotics will last for two weeks.
Prolonged courses of antibiotic tablets. These are usually used for their anti-inflammatory action. They are prescribed for at least 3-6 months. Some antibiotics which may be used are:
Trial of the combined oral contraceptive (COC) pill can be used. A trial of up to 12 months may be needed before deciding whether the skin has improved. Some COC pills (such as Dianette® or Yasmin®) might be better than others.
Retinoids. Acitretin and isotretinoin are sometimes used. These are vitamin A-based medicines. These medicines work by stopping the secretion of sebum from sebaceous glands. They also help the normal shedding of dead skin cells in the hair follicles, preventing pore blockage. They cause serious birth defects, so cannot be used in pregnancy. Women of childbearing age who take them must use effective contraception.
Corticosteroid tablets (steroids), such as prednisolone, may be used in short courses to reduce inflammation. Long courses of steroids are not usually advised. This is because they can cause serious side-effects such as 'thinning' of the bones (osteoporosis), weight gain, high blood pressure, cataracts and mental health problems. See the separate leaflet called Oral steroids for more details.
Medicines that affect the immune system may be used for severe cases and when other treatments haven't worked. The most promising of these treatments are monoclonal antibodies, including anti-TNF medicines such as adalimumab. TNF stands for tumour necrosis factor. TNF is a chemical produced by the immune system which causes inflammation in the body. Anti-TNF medicines block excess TNF, thus preventing inflammation.
Dapsone (usually used to treat leprosy) is used in hidradenitis suppurativa for its anti-inflammatory action.
Surgical treatment
Long-standing hidradenitis suppurativa often requires surgery. Generally, this would be performed under general anaesthetic. The surgical procedure chosen depends on the grade or extent of the hidradenitis suppurativa.
Surgical treatments include:
Incision and drainage - this means piercing (lancing) a tense, hard abscess and allowing the pus to drain out. This is most appropriate for grade 1 hidradenitis suppurativa, and a course of antibiotic tablets would usually be given afterwards.
Wide-scale removal (excision) of affected areas - this can be used for grade 2 and 3 disease. For stage 2 disease, the sinus tracts are surgically removed. In stage 3 disease, the operation needs to be more extensive, as the tracts and scarring go deeper and larger areas are involved. This means a lot of scarred, infected tissue has to be removed. Often skin grafts and other plastic surgery techniques are needed.
Deroofing and skin-tissue-saving excision is a less major operation option.
Carbon dioxide laser treatment can be used as an alternative to conventional surgery (where available) and dependent on the severity of the disease. The diseased tissue is 'vapourised' leaving an open wound which is left to heal. Other similar options being studied are another type of laser treatment called Nd:YAG laser, and intense pulsed light treatment.
Complications of hidradenitis suppurativa
Back to contentsThe main complication is scarring of the skin and deeper tissues. In severe cases, this can cause swelling of the arm (if the armpit was affected) or of the leg (if the groin was affected). This is called lymphoedema.
Other complications include:
A general feeling of being unwell and tired (malaise).
Long-term (chronic) infection leading to problems such as anaemia, kidney problems and low levels of protein in the blood.
Joint pains and inflammation (arthropathy).
Skin cancer. This is rare but has been reported in very severe long-term hidradenitis suppurativa.
Fistula formation. A fistula occurs when channels, called sinus tracts, tunnel into other parts of the body, such as the bowel or bladder (this is rare).
What is the long-term outlook?
Back to contentsThe outlook (prognosis) is very variable. Not everyone progresses from stage 1 to stage 3.
For many affected people, hidradenitis suppurativa is a painful and debilitating condition. It has a tendency to flare up regularly, gradually causing more problems. Deep scarring and formation of tunnels (channels), called sinus tracts, are not uncommon.
Some people have mild (stage 1) disease only. Early surgical treatment can (in some cases) cure the disease and stop it from returning. In rare cases, the condition goes away on its own without treatment.
The condition can prevent normal working and social activities (for example, swimming). Psychological problems are common, as are difficulties in sexual relationships. These problems can either be directly due to the pain and messiness of the condition or to embarrassment and body image problems. As a result, it can cause a less good quality of life.
There are several different foundations that provide advocacy and support for people with hidradenitis suppurative. These include the HS Foundation and the British Skin Foundation. See Further Reading for links.
Patient picks for Other skin problems

Skin, nail and hair health
Skin ulcers
An ulcer is a break in the skin, through which the underlying tissues can be seen. There is usually a problem affecting the normal healing of the skin. There are a number of different types of skin ulcers. Treatment may vary depending on the type of ulcer.
by Dr Doug McKechnie, MRCGP

Skin, nail and hair health
Sun and sunburn
This leaflet discusses the risks and benefits of sunlight to your skin. It gives tips on how to enjoy sunshine safely so it you can do you good and reduce the risk of causing harm. It is very important to protect children from the sun. The delicate skin of a child is more sensitive to sun damage than the skin of an adult.
by Dr Caroline Wiggins, MRCGP
Further reading and references
- Adalimumab for treating moderate to severe hidradenitis suppurativa; NICE Technology Appraisal Guidance, June 2016
- Zouboulis CC, Desai N, Emtestam L, et al; European S1 guideline for the treatment of hidradenitis suppurativa/acne inversa. J Eur Acad Dermatol Venereol. 2015 Apr;29(4):619-44. doi: 10.1111/jdv.12966. Epub 2015 Jan 30.
- Alikhan A, Sayed C, Alavi A, et al; North American clinical management guidelines for hidradenitis suppurativa: A publication from the United States and Canadian Hidradenitis Suppurativa Foundations: Part I: Diagnosis, evaluation, and the use of complementary and procedural management. J Am Acad Dermatol. 2019 Jul;81(1):76-90. doi: 10.1016/j.jaad.2019.02.067. Epub 2019 Mar 11.
- Alikhan A, Sayed C, Alavi A, et al; North American clinical management guidelines for hidradenitis suppurativa: A publication from the United States and Canadian Hidradenitis Suppurativa Foundations: Part II: Topical, intralesional, and systemic medical management. J Am Acad Dermatol. 2019 Jul;81(1):91-101. doi: 10.1016/j.jaad.2019.02.068. Epub 2019 Mar 11.
- Hidradenitis suppurativa; Primary Care Dermatology Society (PCDS)
- Hidradenitis suppurativa; DermNet New Zealand
- British Skin Foundation.
- HS Foundation.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Oct 2027
20 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.