Primary sclerosing cholangitis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 6 Mar 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Primary sclerosing cholangitis is an uncommon condition affecting the bile ducts and liver. Inflammation and scarring of the bile ducts can lead to liver damage and cirrhosis - a condition where normal liver tissue is replaced by scar tissue (fibrosis). Different treatments are available to control symptoms that may develop and also to manage any complications which may occur. The outlook for people with primary sclerosing cholangitis can be very variable.
At a glance
Primary sclerosing cholangitis (PSC) is a rare condition affecting the bile ducts and liver.
It causes scarring and narrowing of the bile ducts, leading to bile build-up and liver damage.
Common early symptoms include tiredness, itchiness, weight loss, and tummy discomfort.
Yellowing of the skin or eyes (jaundice) can occur as the condition worsens.
There is currently no cure for PSC, and treatments focus on managing symptoms and complications.
A liver transplant may be considered if the liver is badly affected.
In this article:
Video picks for Liver and gallbladder
Liver function
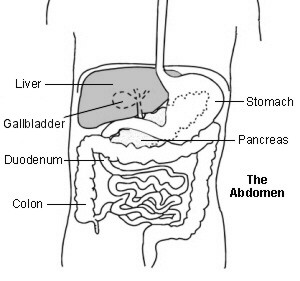
The liver is in the upper right part of the tummy (abdomen). It has many functions which include:
Storing glycogen (fuel for the body), which is made from sugars. When required, glycogen is broken down into glucose which is released into the bloodstream.
Helping to process fats and proteins from digested food.
Making proteins that are essential for blood to clot (clotting factors).
Processing many medicines which you may take.
Helping to remove or process alcohol, poisons and toxins from the body.
Making bile, which passes from the liver to the gut down the bile duct. Bile breaks down the fats in food so that they can be absorbed from the bowel.
Upper abdomen showing bile ducts
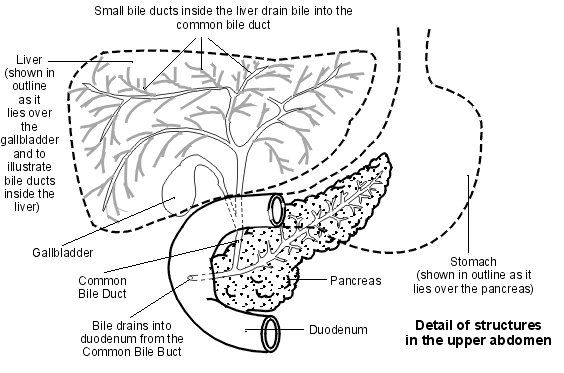
Bile is a yellow-green liquid that contains various chemicals and bile salts. Bile helps you to digest food, particularly fatty foods. It also helps the body to absorb certain vitamins (A, D, E and K) from the food that you eat.
Bile is made by liver cells. Liver cells pass out bile into a network of tiny tubes called bile ducts. They join together (like tributaries of a river) to form the larger common bile duct. Bile constantly drips down the tiny bile ducts, into the common bile duct, and into the first part of the small intestine (which is called the duodenum).
The gallbladder lies under the liver. It is like a pouch off the common bile duct and fills with bile. It is like a reservoir that stores bile. The gallbladder squeezes (contracts) when we eat, as the bile is needed to aid digestion. This empties the stored bile back into the common bile duct and out into the duodenum.
Continue reading below
What is primary sclerosing cholangitis?
Primary sclerosing cholangitis (PSC) is a rare condition that affects the bile ducts and liver. PSC can occur at any age but is more common in people aged around 40 years. It is twice as common in men as in women. PSC is called:
Primary - because the cause is not known. (That is, it is not 'secondary' to any known cause such as alcohol or poisons.)
Sclerosing - because it causes scarring and thickening (sclerosis) of the bile ducts.
Cholangitis - which means inflammation of the bile ducts.
In this condition, the bile ducts both inside and outside the liver become inflamed and scarred. The scarring causes narrowing of these bile ducts which results in bile building up in the liver. The bile can then damage the liver cells. Eventually, the scar tissue can spread throughout the liver, causing cirrhosis and liver failure. Cirrhosis is a serious condition where normal liver tissue is replaced by scar tissue (fibrosis). It tends to progress slowly and often does not cause symptoms in its early stages. However, as the function of the liver gradually becomes worse, serious problems can develop.
See the separate leaflet called Cirrhosis for more details.
Primary sclerosing cholangitis symptoms
Back to contentsIn many cases the symptoms develop gradually over weeks or months. At the beginning of the disease, many people have no symptoms at all. The most common early symptoms include:
Feeling more tired than usual.
Feeling generally unwell.
Itchy skin.
Weight loss.
Having some discomfort in the right upper tummy (abdomen).
Jaundice is a symptom of PSC when the condition worsens. If you have jaundice, you 'go yellow'. You tend to notice it first when the whites of the eyes become yellow. This is due to a build-up of the chemical bilirubin, which is made in the liver and, in some liver conditions, spills into the blood.
Continue reading below
Primary sclerosing cholangitis causes
Back to contentsThe cause is not clear. It can sometimes run in families. Around four out of five people with PSC also have inflammatory bowel disease (most often ulcerative colitis, but it can also be associated with Crohn's disease). About 1 in 10 people with inflammatory bowel disease are affected by PSC.
Primary sclerosing cholangitis treatment
Back to contentsAt present there is no specific treatment for PSC which either cures or slows the progression of PSC disease. Treatments aim to improve symptoms and also to manage any complications which may arise.
Treatment of symptoms. Itching of the skin can be difficult to treat but is usually eased with a medicine called colestyramine. Other medicines may be tried if this is not effective.
Medical treatment. Although vitamin supplements may be advised, there is no proven medical treatment that alters the progression or outcome in PSC. Ursodeoxycholic acid (UCDA) is often used and has been shown to improve liver function but clinical trials have not shown any benefit regarding any improved outcome.
Treatment of complications. Antibiotics will be given if you have an episode of infective cholangitis. If your cholangiogram shows that you have an obstruction to the bile duct outside your liver, it may be possible for a doctor to place a small drainage tube (a stent) or use a very small balloon to open up the blockage.
Liver transplant. Liver transplantation is the only treatment able to modify the outlook of the disease. It may be considered if your liver is affected badly. The outlook following a liver transplant is good. However, PSC recurs in around a fifth of cases following a liver transplant.
Diet and alcohol. Most people with PSC will be advised to eat a normal healthy diet. Ideally, anybody with inflammation of the liver should not drink alcohol, or only in very small amounts. If you already have liver inflammation, alcohol may increase the risk and speed of developing cirrhosis - where normal liver tissue is replaced by scar tissue (fibrosis).
Continue reading below
What are the complications?
Back to contentsVarious complications can occur in some people with PSC. These include:
Deficiencies of some vitamins, usually vitamins A, D, E and K. These are the vitamins which are fat-soluble (rather than the other vitamins which are water-soluble). This means they dissolve in fat. Bile helps the fat to be broken down and these vitamins to be absorbed.
PSC cholangitis, which is infection of the blocked bile ducts. This is called infective cholangitis. This may cause chills, fever and upper tummy (abdominal) tenderness.
Cirrhosis - where normal liver tissue is replaced by scar tissue (fibrosis).
Liver failure.
Bile duct cancer. This eventually affects around 1 in 10 people who have PSC.
Diagnosing primary sclerosing cholangitis
Many people with PSC have no, or only vague, symptoms for quite some time in the early stages of the disease. Therefore, the diagnosis is often made when you have tests for an unrelated condition or routine tests if you have inflammatory bowel disease.
Tests usually include:
Blood tests called liver function tests. These measure the activity of chemicals (enzymes) and other substances made in the liver. This gives a general guide as to whether the liver is inflamed and how well it is working. See the separate leaflet called Abnormal liver function tests for more details.
Other blood tests may be performed to rule out (exclude) other causes of liver conditions, such as viral hepatitis.
An ultrasound scan of the liver may be performed.
A cholangiogram is a test which produces a picture of the bile ducts. This is often done using a magnetic resonance imaging (MRI) scan.
Taking a small sample (biopsy) of the liver. This may be carried out to look at the sample under the microscope. It can show inflammation and the extent of any cirrhosis (where normal liver tissue is replaced by scar tissue (fibrosis) in the liver). The liver biopsy can also assess how early or advanced the disease is. See the separate leaflet called Liver biopsy for more details.
Does primary sclerosing cholangitis alter life expectancy?
The course of PSC is variable. The outlook and life expectancy are poorer in older patients, those who have an enlarged liver and spleen, and in patients who are persistently jaundiced. There is also an increased risk of developing cancer of the bile duct (cholangiocarcinoma) or bowel (colorectal) cancer. The risk of developing bowel cancer is higher in people with PSC who also have ulcerative colitis.
Apart from liver transplantation, there are no effective treatments for PSC. Some US studies suggest life expectancy ranges from 9 to 18 years if the patient does not have a liver transplant. However, researchers in the Netherlands concluded that life expectancy may be longer than 21 years from the time when the diagnosis is made.
The treatment of PSC is a developing area of medicine. New treatments continue to be researched and the information above is very general. The specialist who knows your case can give more accurate information about the outlook for your particular situation.
Patient picks for Liver and gallbladder

Digestive health
Gallstones
Gallstones are common but cause no symptoms in two out of three people who have them. They sometimes cause pain, yellowing of your skin or the whites of the eyes (jaundice), inflammation of the pancreas (pancreatitis) and gallbladder inflammation. Surgery is the usual treatment for gallstones that cause symptoms.
by Dr Colin Tidy, MRCGP

Digestive health
Cirrhosis
Cirrhosis is a serious condition where normal liver tissue is replaced by scar tissue (fibrosis). It tends to progress slowly and often does not cause symptoms in its early stages. However, as the function of the liver gradually becomes worse, serious problems can develop. In the UK, the two commonest causes of cirrhosis are alcohol drinking above recommended limits and hepatitis C infection. Treatments may vary, depending on the cause. If cirrhosis becomes severe, a liver transplant may be the only option.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
What is the main function of bile and how does PSC affect it?
Bile is a yellow-green liquid produced by the liver that helps digest food, especially fatty foods, and absorb certain vitamins (A, D, E, K). In Primary Sclerosing Cholangitis (PSC), the bile ducts become inflamed and scarred, which narrows them. This narrowing causes bile to build up in the liver, which can then damage liver cells and eventually lead to cirrhosis.
What does 'cholangitis' mean in the context of PSC?
Cholangitis means inflammation of the bile ducts. In PSC, this refers to the inflammation and scarring that occurs in both the bile ducts inside and outside the liver.
If I have inflammatory bowel disease, am I at a higher risk of developing PSC?
Yes, there is a known association between PSC and inflammatory bowel disease. Around four out of five people with PSC also have inflammatory bowel disease, most commonly ulcerative colitis but also Crohn's disease. About 1 in 10 people with inflammatory bowel disease are affected by PSC.
Are there any effective ways to slow down or cure PSC?
Currently, there is no specific treatment for PSC that can cure it or slow down its progression. Treatments focus on managing symptoms and complications. A liver transplant is the only treatment that can change the outlook of the disease, but PSC can recur in about a fifth of cases even after a transplant.
Why are vitamin deficiencies a complication of PSC?
PSC can lead to deficiencies of fat-soluble vitamins (A, D, E, K). Bile plays a crucial role in breaking down fats and helping the body absorb these specific vitamins. When bile ducts are damaged and bile flow is impaired due to PSC, this absorption process is disrupted.
What kind of tests are used to diagnose PSC?
Diagnosis of PSC often involves several tests. These include blood tests like liver function tests to check liver health and rule out other conditions such as viral hepatitis. An ultrasound scan of the liver, a cholangiogram (often using MRI) to visualise the bile ducts, and sometimes a liver biopsy are also used. A liver biopsy allows doctors to examine a sample of liver tissue to assess inflammation and the extent of scarring or cirrhosis.
Further reading and references
- Nicoletti A, Maurice JB, Thorburn D; Guideline review: British Society of Gastroenterology/UK-PSC guidelines for the diagnosis and management of primary sclerosing cholangitis. Frontline Gastroenterol. 2020 Mar 2;12(1):62-66. doi: 10.1136/flgastro-2019-101343. eCollection 2021.
- EASL Clinical Practice Guidelines on sclerosing cholangitis. J Hepatol. 2022 Sep;77(3):761-806. Epub 2022 Jun 21.
- Tan N, Lubel J, Kemp W, et al; Current Therapeutics in Primary Sclerosing Cholangitis. J Clin Transl Hepatol. 2023 Oct 28;11(5):1267-1281. doi: 10.14218/JCTH.2022.00068S. Epub 2023 Apr 17.
- Sarcognato S, Sacchi D, Grillo F, et al; Autoimmune biliary diseases: primary biliary cholangitis and primary sclerosing cholangitis. Pathologica. 2021 Jun;113(3):170-184. doi: 10.32074/1591-951X-245.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Mar 2028
6 Mar 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.