Pigmented skin lesions
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 10 Feb 2026
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Melanoma skin cancer article more useful, or one of our other health articles.
In this article:
Continue reading below
What are pigmented skin lesions?
Pigmented skin lesions can be considered as melanocytic neoplasms. The essential task is to exclude malignant melanoma. See also the separate Malignant melanoma of skin and Skin biopsy techniques in general practice articles.
It is important to bear in mind that younger people in the UK are increasingly being affected by malignant melanoma, with over 900 diagnoses a year. This makes it the second most common cancer in those who are 25-49 years of age in the UK.1
Malignant melanoma
Back to contentsImage: a suspicious flat lesion, irregular in shape and pigmentation
Superficial spreading melanoma
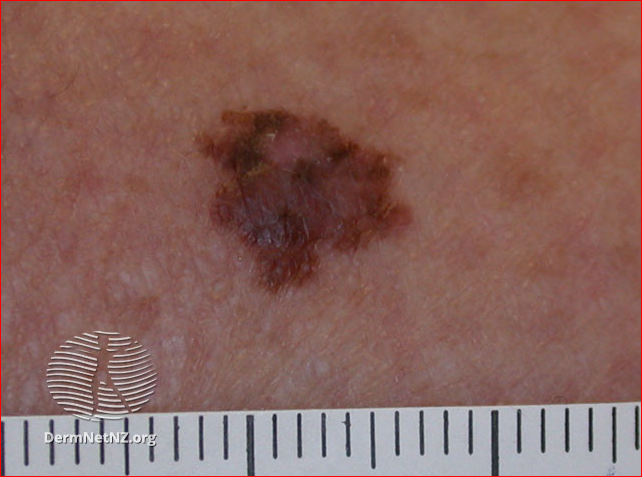
Superficial spreading melanoma image above:DermNet New Zealand. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 New Zealand License.
Melanomas may have a variety of colours, including tan, dark brown, black, blue, red and, occasionally, light grey.
When assessing melanomas, factor in risk factors2 including:
Family history of melanoma.
Personal history of melanoma.
Immunosuppression.
Excessive UV exposure, including tanning beds.
7-point checklist
Use the 7-point weighted checklist for assessment of pigmented skin lesions:3
Major features of lesions (two points each):
Change in size.
Irregular shape.
Irregular colour.
Minor features of lesions (one point each):
Largest diameter 7 mm or more.
Inflammation.
Oozing.
Change in sensation.
Lesions scoring three points or more in the 7-point checklist above are suspicious (if you strongly suspect cancer, any one feature is adequate to prompt urgent referral).
For low-suspicion lesions, undertake careful monitoring for change, using the 7-point checklist.
The National Institute for Health and Care Excellence (NICE) recommends ideally making measurements with photographs and a marker scale and/or ruler.
This guidance comes from the 2015 NICE guideline on detection of cancer. The guidance was updated in 2020, but there were no changes relevant to assessment and diagnosis of skin cancer.3
ABCDE
An alternative aide-mémoire to the 7-point checklist described below is the 'ABCDE' list:
Asymmetry.
Border irregular.
Colour irregular.
Diameter greater than 7 mm.
Evolving.
Melanoma vs normal mole
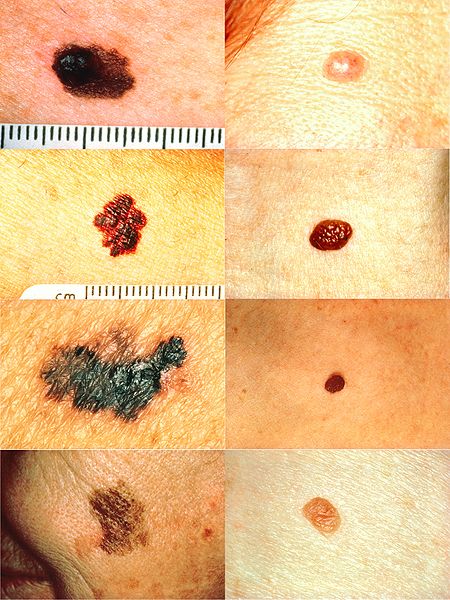
However, not all these features may be present and, if malignant melanoma cannot be excluded then excision biopsy is required.4
Change in size: naevi may change in size over years but any change over weeks or months is suspicious.
Change in colour:
Melanomas often show irregular pigment in a lesion, with shades of black, brown, grey and pink. In nodular melanoma (see below) the lesion is often black throughout.
Rarely, a melanoma can present as a non-pigmented red nodule (amelanotic melanoma), which is more likely on the hands and feet.
Change in outline: melanomas often show a geographical outline with a sharp cut-off from normal skin.
Itching may be a late sign and is often unreliable, as many benign naevi intermittently itch.
Bleeding is also a late sign and is often present in advanced melanoma.
Melanoma in women occurs more commonly on the extremities and in men on the trunk or head and neck but it can arise from any site on the skin surface.
Examination of suspicious lesions should include a thorough assessment for other suspicious skin lesions, palpation for regional lymph nodes and examination of the abdomen for enlarged liver and/or spleen.
Nodular melanoma
Important information |
|---|
Nodular melanoma tends to lack the typical ABCDE melanoma warning signs and therefore may be diagnosed late with a much worse prognosis. Nodular melanomas tend to occur on the heads and necks of elderly sun-damaged men.5 A nodular melanoma is usually uniform in colour with early ulceration and bleeding. |
Image: pigmented lesion on an exposed area. It looks highly suspicious - the patient should be referred urgently
Nodular melanoma on an ear
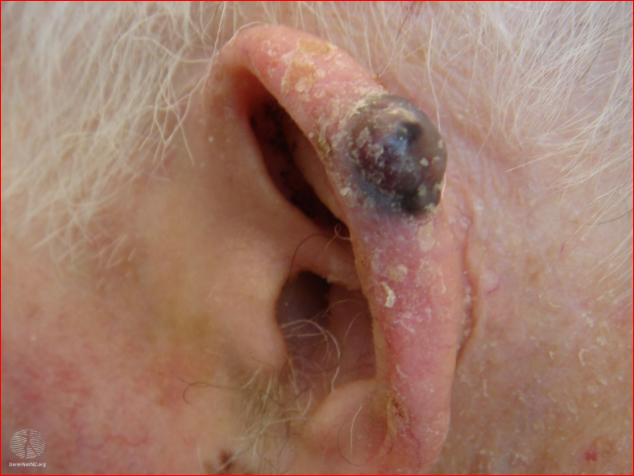
Nodular melanoma image above:
DermNet New Zealand. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 New Zealand License.
Multiple cutaneous melanomas
The incidence of multiple primary melanomas has been reported (depending on the study) from 1.1% to 20.4%.6The highest incidence of 20.4% was reported in Australia, while the highest incidence in Europe and North America was 18.1% in Austria and 8.6% in the US respectively.
The highest number of primary tumours in one individual was 13, and the mean number of primary tumours per individual ranged from 2.1 to 2.8.6
Lesions may be classified as synchronous if they present at the same time or within two months, or metachronous if the second melanoma presents later.
Continue reading below
Other types of pigmented skin lesions
Back to contentsIntradermal naevi (common moles)
Also called common naevi. See also the separate Intradermal and compound naevi article.
Most adults will have approximately 30 moles which they have been acquiring from infancy. Naevi remain static whereas melanoma change in size, shape or colour over weeks or months. New common moles rarely develop after the age of 40 years and any that do are suspicious.
Typical features of common naevi are:
Symmetrical in area.
Even, brown colouring (light or dark).
Sharp margin.
<5 mm in diameter.
Profile varying from flat to pedunculated.
While an increased number of naevi is a strong melanoma risk factor, each individual naevus has a low risk of melanoma transformation, and most melanomas are non-naevus associated.7 Patients need careful skin monitoring, including baseline skin photography. Any lesion that starts to change colour, bleed, itch, be painful or increase in size needs excisional biopsy.
Dysplastic naevi (atypical moles)
Also known as dysplastic naevi. They are found in approximately 1 in 12 white people and do not usually become evident until puberty. Unlike melanoma, atypical naevi are usually symmetrical and do not have a sharp edge with geographical border; asymmetry and sharp-edged borders are clear signs of malignant transformation.8
Atypical moles are easily mistaken for malignant melanoma because of their:
Lack of symmetry.
Lack of sharp margin.
Size >6 mm.
Variation in colour within the lesion.
Image: atypical naevus
Atypical naevus
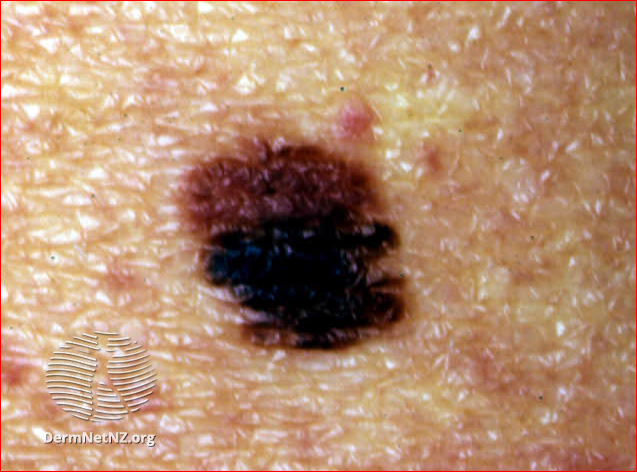
Atypical naevus image above:
DermNet New Zealand. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 New Zealand License.
Unlike common moles they continue to appear throughout life and occur in areas not often exposed to the sun - eg, buttocks. They are a strong, independent risk factor for malignant melanoma, conferring a 10-fold increased risk of malignant melanoma.8 This is especially the case when they are present in numbers (12% risk over ten years). Patients should be very careful with sunlight and undergo regular skin surveillance. Excision of dysplastic naevi is not performed routinely.
Congenital naevi (birth moles)9
See the separate Congenital pigmented naevus article.
Very large congenital naevi are known as giant naevi. Patients with large congenital naevi have an increased risk of developing malignant melanoma, often by the age of 10 years. These appear either within the lesion or as CNS melanoma. Treatment is either excision or close monitoring. Laser treatment is also available.
Blue naevus (blue moles)10
See the separate Blue naevus article.
A blue naevus is a small blue or grey lesion, with an appearance similar to a mole. The diagnosis of blue naevus is generally clinical, made grossly, or with a dermatoscope, though biopsy and pathological evaluation are the gold standard for definitive diagnosis.
Image: blue naevus
Blue naevus
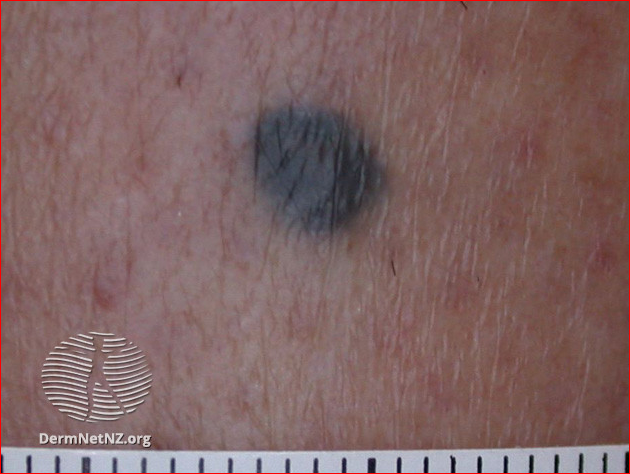
Blue naevus image above:
DermNet New Zealand. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 New Zealand License.
Spitz naevus (pink or red moles)
Spitz naevi usually affect the face or limbs of young children. They initially grow rapidly but may then remain static for years. They often disappear spontaneously after a period of time.11
Epidermal naevus (birthmark)
See the separate Epidermal naevus and its syndromes article.
Epidermal naevi may be congenital lesions or develop during the early years of life. They tend to grow during childhood and then stabilise during the teenage years. They may be localised to a small area or occur in more diffuse forms.
Epidermal naevus syndromes are a heterogeneous group of disorders characterised by the presence of one or more congenital hamartomatous ectodermal naevi of the skin with other organ involvement, including brain, eye and the skeleton.
Becker's naevus: this is a form of epidermal naevus (birthmark). It usually appears around puberty as a hyperpigmented patch, most often found on the upper trunk or shoulders.
Halo naevus (halo moles)
See the separate Halo naevus article.
Usually, these consist of a central uniformly pigmented naevus, usually round or oval in shape, with a surrounding area of depigmentation of uniform width from the naevus's edge.
Junctional naevus (flat moles)
See the separate Junctional naevus article.
Junctional naevi are often quite darkly pigmented and are macular or very thinly papular with only minimal elevation above the level of the skin.
They are an acquired lesion and as they age they can change their characteristics to that of compound naevi.
Compound naevus (flat and raised moles)
See the separate Intradermal and compound naevi article.
Compound naevi arise from a flat (junctional) naevus that exists earlier in life. Pigmentation may be uneven within the naevus but is usually symmetrically distributed.
They are usually of a round/oval shape and roughly 2-7 mm in diameter. They may exist with a variable degree of pigmentation and even be the same colour as the surrounding skin.
Sebaceous naevus (birthmark)
See the separate Sebaceous naevus article.
Usually a single hairless patch (round or linear) is noted on the scalp at birth or shortly afterwards. The classic appearance is velvety tan or yellow-orange.
Seborrhoeic wart
See the separate Seborrhoeic wart article.
A flat-topped or warty-looking lesion that appears to be stuck on to the skin. They are usually pigmented, sometimes deeply. They may even be black.
Further reading and references
- Melanoma: assessment and management; NICE Guidance (July 2015 - last updated July 2022)
- Melanoma and pigmented lesions; NICE CKS, July 2022 (UK access only)
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated January 2026)
- Melanoma tests; Cancer Research UK
- Lu CT, Lin TL, Mukundan A, et al; Skin Cancer: Epidemiology, Screening and Clinical Features of Acral Lentiginous Melanoma (ALM), Melanoma In Situ (MIS), Nodular Melanoma (NM) and Superficial Spreading Melanoma (SSM). J Cancer. 2025 Sep 21;16(13):3972-3990. doi: 10.7150/jca.116362. eCollection 2025.
- Apostu AP, Ungureanu L, Halmagyi SR, et al; Multiple primary melanomas: A literature review. Medicine (Baltimore). 2023 Jul 28;102(30):e34378. doi: 10.1097/MD.0000000000034378.
- Zhang Y, Ostrowski SM, Fisher DE; Nevi and Melanoma. Hematol Oncol Clin North Am. 2024 Oct;38(5):939-952. doi: 10.1016/j.hoc.2024.05.005. Epub 2024 Jun 15.
- Baigrie D, Tanner LS; Dysplastic Nevi.
- Navarro-Fernandez IN, Mahabal GD; Congenital Nevus.
- Austad SS, Athalye L; Blue Nevus.
- Skin lesions, tumours and cancers; DermNet NZ
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Aug 2030
10 Feb 2026 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free