Heart valve disease
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 13 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Mitral stenosisMitral regurgitationAortic stenosisAortic regurgitationInfective endocarditis
Heart valves sit in between the chambers of the heart and control the blood flow through the heart. There are four common types of heart valve problem - mitral stenosis, mitral regurgitation, aortic stenosis and aortic regurgitation. The leaflet called Anatomy of the heart includes details about the function of the heart and how the heart beats.
In this article:
Video picks for Heart disease
Continue reading below
What is heart valve disease?
A heart valve that is diseased or damaged can affect the flow of blood through the heart. There are two main types of heart valve problem:
Heart valve stenosis. This means that the opening of the heart valve is narrowed and the valve does not open fully. This leads to a restriction in blood flow through the valve.
Heart valve regurgitation (sometimes called heart valve incompetence, or a leaky valve). This means that the valve does not close properly and there is backflow of blood through the leaky valve.
Any of the heart valves can be affected by these problems. However, the mitral and aortic valves are the ones that most commonly become diseased. Read more in our separate leaflets on mitral stenosis, mitral regurgitation, aortic stenosis and aortic regurgitation.
Normal heart detail
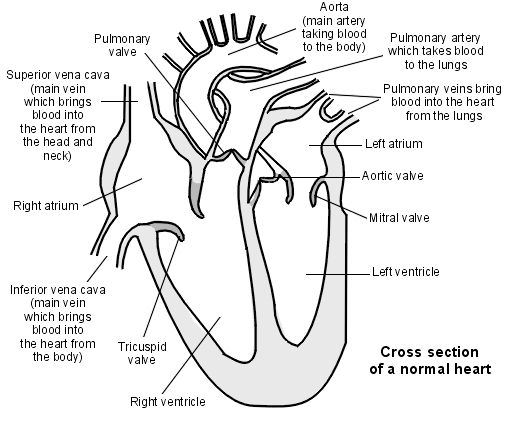
Symptoms of heart valve disease
Back to contentsThese symptoms are also common in other conditions and do not necessarily mean that there is heart valve disease. However, heart valve disease may need to be looked for with these symptoms.
Heart valve disease symptoms may include:
Shortness of breath. This tends to develop gradually, initially on exercise and then developing at rest if the stenosis becomes worse. This symptom is due to a build-up of fluid in the lungs.
Fainting, dizziness or tiredness. If the amount of blood getting through to the ventricle is reduced, the output of blood from the left ventricle to the body is then reduced.
Chest pains (angina). This may develop if there is a reduced blood flow to the arteries that take blood to the heart muscle (the coronary arteries).
Fast or irregular heartbeat which may be felt as the sensation of a 'thumping heart' (palpitations).
Chest infections may happen more often.
Coughing up bloodstained sputum. This may occur due to the build-up of fluid in the lungs.
The liver may be enlarged and not function as well; this may cause a build-up of fluid in the abdomen leading to an enlarged abdomen.
People with mitral stenosis may get flushed cheeks.
Continue reading below
Causes of heart valve disease
Back to contentsDegenerative changes
This is the most common cause of leaky heart valves (heart valve regurgitation). The structures supporting the heart valves weaken and stretch over time and this prevents the valves from closing properly.
Rheumatic heart disease
Rheumatic heart disease refers to any heart problem which develops after having an episode of rheumatic fever.
Rheumatic fever is a condition which sometimes follows an infection with a bacteria called streptococcus. The body makes antibodies to the bacteria to clear the infection but, in some people, the antibodies also attack various parts of the body - in particular, the heart valves. Inflammation of one or more valves may develop which can cause permanent damage and lead to thickening and scarring years later.
Rheumatic fever used to be common in the UK in the era before antibiotics but it is now rare. It is still quite common in some low and middle income countries.
If rheumatic fever is the cause then symptoms often start between the ages of 20 and 50 years, about 10-20 years after having had an episode of rheumatic fever as a child.
Other causes of heart valve disease
Other causes of heart valve disease include:
Deposits of calcium (calcification) in parts of the valve. This is the most common cause of aortic stenosis in older people.
Some heart problems present from birth (congenital). It is then usually part of a complex heart deformity.
A leaky heart valve may occasionally occur following heart valve surgery.
A complication of various uncommon diseases.
Diagnosing heart valve disease
Back to contentsA doctor may hear a heart murmur or other abnormal noises when listening with a stethoscope. Murmurs and noises are due to blood passing through abnormal heart valves, or to abnormal movement of valves. There are typical murmurs and noises which occur with each heart valve problem.
Initial tests usually include a chest X-ray and a heart tracing (an electrocardiogram, or ECG).
An ultrasound scan of the heart (an echocardiogram, or 'echo') can confirm the diagnosis.
Other heart tests, including computerised tomography (CT) scans and magnetic resonance imaging (MRI) scans can help to assess the severity of the condition.
Cardiac catheterisation may be done to assess the severity of the heart valve problem. In this test a thin tube called a catheter is inserted into either the main blood vessel in the top of the leg (femoral artery) or an artery in the wrist (radial artery). It is passed up to the heart. A small device on the tip of the catheter can measure the pressure on either side of the heart valve.
Continue reading below
Complications of heart valve disease
Back to contentsVarious complications may develop, depending on the valve affected and the severity of the problem.
The main possible complications that may develop include the following:
Atrial fibrillation develops in about 4 in 10 cases. In this condition, the heart beats in a fast and irregular way. This occurs because the electrical signals in the enlarged atrium become faulty. The irregular heart rhythm can cause the sensation of palpitations and breathlessness. See the separate leaflet called Atrial fibrillation.
Heart failure may develop and gradually become more severe. This causes worsening shortness of breath, tiredness, and fluid retention in various tissues of the body. See the separate leaflet called Congestive heart failure.
Stroke. A blood clot may form within the enlarged left atrium, which does not fully empty into the ventricle with each heartbeat. A blood clot is more likely to occur if you also develop atrial fibrillation. A blood clot may travel through the heart, be carried in the bloodstream and get stuck and block a blood vessel in another part of the body. For example, it may get stuck in a blood vessel going to the brain and cause a stroke. See the separate leaflet called Stroke.
Endocarditis sometimes develops. This is an infection of the valve. (Damaged valves are more prone than normal valves are to infection.) Unless promptly treated, endocarditis can cause serious illness. See the separate leaflet called Infective endocarditis.
Treatment for heart valve disease
Back to contentsAny treatment will depend on which valve is affected and the severity of the heart valve problem. Learn more about the treatments for mitral stenosis, mitral regurgitation, aortic stenosis and aortic regurgitation.
Medication
Mild cases may not require any regular medication. Some medicines may be prescribed to help ease symptoms, or to help prevent complications. For example:
Angiotensin-converting enzyme (ACE) inhibitors are medicines which help to reduce the amount of work the heart does. One may be prescribed to ease symptoms of heart failure.
'Water' tablets (diuretics) help to reduce the build-up of fluid caused by the heart working less efficiently. They make the kidneys produce more urine. This gets rid of the excess fluid built up in the lungs or other parts of the body with the back pressure from the heart.
In atrial fibrillation, several medicines can be used to slow the heart rate down. They include beta-blockers, calcium-channel blockers and digoxin. Shocking the heart with an electrical current (a procedure called cardioversion) is also an option in some people who develop atrial fibrillation as a complication.
Anticoagulation medication is usually advised in atrial fibrillation. This helps to prevent blood clots from forming.
Surgery
Surgery to stretch, repair or replace the heart valve may be needed. Surgical treatment has greatly improved the outlook for many cases of severe valve disease. Surgery has a very good success rate. Increasingly, minimal access surgery (via a catheter into the blood vessels rather than open heart surgery) is being used, particularly in people who are less fit for surgery. This is called transcatheter aortic valve implantation (TAVI).
Living with heart valve disease
Back to contentsMild heart valve disease is very common and rarely progresses to heart disease that needs treating. People with mild heart disease do not need to alter their lifestyle - as with everyone, exercise and a healthy diet are recommended. People with moderate to severe heart valve disease should be referred for consideration of surgery or medical management. Some specialists advise repeating an echocardiogram every 3 to 5 years in people with mild heart valve disease.
Patient picks for Heart disease

Heart health and blood vessels
Mitral stenosis
Mitral stenosis means that when the mitral valve opens, it does not open fully. The opening is therefore narrower than normal (stenosed).
by Dr Colin Tidy, MRCGP

Heart health and blood vessels
Angina
Angina is a pain that comes from the heart. It is usually caused by narrowing of the heart's blood vessels - the (coronary) arteries. Usual treatment includes a statin medicine to lower your cholesterol level, low-dose aspirin to help prevent a heart attack, and a beta-blocker medicine to help protect the heart and to prevent angina pains. An angiotensin-converting enzyme (ACE) inhibitor medicine is advised in some cases. Sometimes angioplasty or surgery are options to widen, or to bypass, narrowed arteries.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Prophylaxis against infective endocarditis: Antimicrobial prophylaxis against infective endocarditis in adults and children undergoing interventional procedures; NICE Clinical Guideline (March 2008 - last updated July 2016)
- 2023 ESC Guidelines for the management of infective endocarditis; European Society of Cardiology (Aug 2023)
- Heart valve disease presenting in adults: investigation and management; NICE guideline (November 2021)
- Guidelines for the management of valvular heart disease; European Society of Cardiology (2025)
- Otto CM, Nishimura RA, Bonow RO, et al; 2020 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2021 Feb 2;77(4):e25-e197. doi: 10.1016/j.jacc.2020.11.018. Epub 2020 Dec 17.
Continue reading below
About the author

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Jan 2028
13 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.