Uveitis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 19 Dec 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Eye problemsInfective conjunctivitisAllergic conjunctivitisDry eyesEpiscleritis and scleritisSubconjunctival haemorrhage
Uveitis is a general term describing inflammation of the part of the eye called the uveal tract. This consists of the iris, ciliary body and choroid - although uveitis can additionally involve other parts of the eye.
In this article:
Video picks for Eye conditions
Key points
Uveitis is inflammation of the uveal tract, the middle layer of tissue inside the eye. It causes symptoms such as eye pain, redness, blurred vision, and sensitivity to light.
The exact cause of uveitis is unknown, however it has been linked to autoimmune conditions, infections, and eye injuries.
Treatment involves steroid eye drops and pupil dilators, which help to reduce inflammation. Untreated uveitis may lead to permanent vision loss.
Continue reading below
What is uveitis?
Uveitis is inflammation of the uveal tract. The uveal tract is the name given to the part of your eye that is made up of:
The iris: the part of your eye that gives it colour.
The ciliary body: a small ring-like muscle that sits behind your iris and which helps the eye to focus.
The choroid: the layer of tissue between your retina and your sclera, containing blood vessels and a pigment that absorbs excess light.
The uvea contains most of the eye's blood vessels. Parts of the eye next to the uveal tract can also be affected. These include:
The retina: the light-sensitive layer lining the interior of your eye.
The optic nerve: the nerve responsible for vision.
The vitreous humour: the jelly-like material that fills the chamber behind your lens.
The sclera: the white outer layer of your eyeball.
Human eye schematic
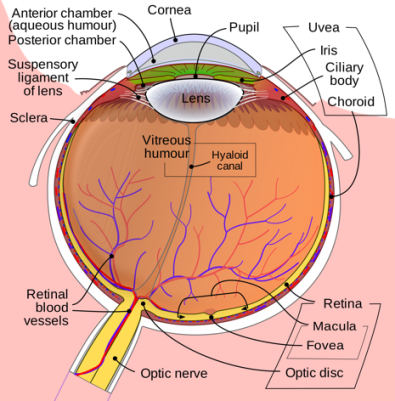
© By Rhcastilhos, via Wikimedia Commons
What are the different types of uveitis?
Back to contentsUveitis is classified according to the part of the uveal tract that the inflammation affects:
Anterior uveitis
Anterior uveitis is the term for inflammation which affects the eye's front (anterior) part of the uveal tract. This can include the iris (iritis) or the iris and the ciliary body (iridocyclitis). It is the most common type of uveitis and the most painful. It is most often caused by inflammatory diseases, infections or trauma.
Intermediate uveitis
Intermediate uveitis is the term for inflammation which affects the middle part of the uveal tract or eye, mainly the vitreous humour. It can also affect the underlying retina. It has been linked to several diseases, including sarcoidosis.
Posterior uveitis
Posterior uveitis is the term for inflammation which affects the back (posterior) part of the eye. It can affect the choroid, the head of the optic nerve, and the retina (or any combination of these structures). It includes chorioretinitis, retinitis and neuroretinitis. Posterior uveitis is the least common form of uveitis.
Panuveitis
Panuveitis is the term for inflammation affecting the whole of the uveal tract. This is the most serious form. Behçet's disease is one of the most common causes and it can severely damage the retina.
Intermediate, posterior and panuveitis are the most likely forms of uveitis to affect vision, and the most recurrent forms.
Uveitis can be:
Acute: the uveitis is of sudden onset and lasts less than three months (attacks in this form usually last around six weeks).
Chronic: this means it is persistent. The uveitis lasts for more than three months.
Recurrent: the disease can flare up (relapse) and, at other times, it settles down. Recurrence is very common, although the time between attacks is very variable.
The reason why some people develop chronic uveitis is not known. It is not thought to be due to inadequate treatment.
Continue reading below
Uveitis causes
Back to contentsUveitis is caused by inflammatory response inside the eye. Inflammation is the body's natural response to tissue damage. It produces swelling, redness and heat. Uveitis may be caused by:
An attack from the body's own immune system (autoimmunity).
Infections or tumours occurring within the eye or in other parts of the body.
Injury to the eye.
However, in up to half of cases, no specific cause is found. This is known as idiopathic uveitis.
The known causes and associations of uveitis include the following:
Autoimmune and inflammatory diseases
Our immune system normally makes small proteins (antibodies) to attack bacteria, viruses and other 'germs'. In people with autoimmune diseases, the immune system makes antibodies against the tissues of their body, causing damage and inflammation.
It is not clear why this happens. Some people have a tendency to develop autoimmune diseases. In such people, something might trigger the immune system to attack the body's own tissues. The 'trigger' is not known.
Autoimmune diseases that are associated with uveitis include rheumatoid arthritis and Behçet's disease. It is also thought that 'idiopathic' uveitis may, in fact, have an autoimmune basis.
People with some other inflammatory diseases are also more prone to uveitis. Such diseases include:
Inflammatory bowel disease (including Crohn's disease and ulcerative colitis).
Infection
Various types of infections caused by germs (bacterial, fungal and viral) can cause inflammation of your eye and uveitis. Infections include:
Toxoplasmosis (the most common infectious cause of anterior uveitis).
Cytomegalovirus.
HIV and syphilis are rare infectious causes.
Injury to the eye
Uveitis can occur after injury to your eye.
Iatrogenic causes
'Iatrogenic' refers either to an unforeseen or to an inevitable side-effect from a medical treatment. In this case, iatrogenic uveitis is usually uveitis that has resulted from eye surgery.
Rarely, uveitis can occur as a side-effect of some medicines. Examples include rifabutin (used to treat tuberculosis) and cidofovir (used to treat human cytomegalovirus infection).
Cancers
Some cancers are associated with inflammation and uveitis. These include leukaemia, lymphoma and ocular malignant melanoma - but all are rare causes of uveitis.
How common is uveitis?
Back to contentsIt is thought that between 17 and 52 per 100,000 people develop uveitis each year in the UK. It mostly affects people between the ages of 20 and 59 and is uncommon in children. However, uveitis can affect anyone of any age.
If you have one of the underlying conditions or problems mentioned above, you are at greater risk of developing uveitis. In countries of the developed world, such as the UK, uveitis is the cause of visual impairment in about 1 in 10 people.
Continue reading below
Uveitis symptoms
Back to contentsThe symptoms can vary depending on which type of uveitis you have.
Anterior uveitis symptoms
This usually affects one eye. The common symptoms are:
Eye pain (usually felt as a dull ache in and around the eye).
Redness of your eye.
Photophobia (which means you find bright light painful or uncomfortable).
You may develop blurred vision or even some visual loss. You may develop headaches. The pupil of the affected eye may change shape slightly and may not react to light properly (normally becomes smaller) or it may lose its smooth round shape. Your eye may become watery. The symptoms tend to develop over a few hours or days.
Intermediate uveitis symptoms
This usually causes painless blurred vision. It is unusual to experience photophobia and redness of your eye. You may notice floaters and these are a common symptom. Floaters are dark shapes that you see, especially when looking at a brightly illuminated background such as a blue sky. Both eyes are usually affected in intermediate uveitis.
Posterior uveitis symptoms
This commonly causes painless blurring of vision. In some people, it can cause severe visual loss. If you have posterior uveitis you may notice floaters, as described above.
You may also develop scotomata. These are small areas of less sensitive, or absent, vision in your visual field. These areas are surrounded by normal sight. It is usual for only one of your eyes to be affected in posterior uveitis and symptoms tend to take longer to develop.
How is uveitis diagnosed?
Back to contentsUveitis is usually suspected on the basis of the symptoms that you have. If your doctor suspects that you have uveitis, you will usually be referred to an eye specialist for further examination and confirmation. The doctor may start by testing your vision. This allows them to assess any differences in vision between your eyes. It also means that they can tell if the uveitis is causing your vision to worsen.
The doctor examining your eye will use a special microscope called a slit-lamp to examine your eye. If you have uveitis, the doctor will see some specific signs of inflammation in your eye that will allow them to make the diagnosis.
You may need further investigations, especially if the doctor thinks there may be an underlying problem. You may also need further investigations if you have had previous episodes of uveitis, or if this episode is severe or affects both eyes. These tests may include optical coherence tomography (OCT), which takes special pictures of your eye, blood tests and possibly also a chest X-ray.
What is the treatment for uveitis?
Back to contentsTreatment for uveitis aims to help relieve pain and discomfort in the eye(s), treat any underlying cause (if possible) and reduce the inflammation. This may prevent permanent loss of vision or other complications. Treatment usually includes the following:
Steroid eye drops
Steroid eye drops are usually used to reduce the inflammation in uveitis. Steroid drops are the main treatment for uveitis and may be the only treatment for mild attacks. Examples of steroid drops include prednisolone and dexamethasone eye drops.
Although steroid eye drops usually work well, in some cases side-effects occur and these are sometimes serious. Therefore, steroid eye drops are usually only prescribed by an eye specialist (an ophthalmologist) who can monitor the situation. It is particularly important to be certain that you don't have herpes simplex virus (also called cold sore virus) infection of your eye before steroids are used.
Possible side-effects that sometimes occur include ulcers on the cornea of the eye, which can be very painful and affect your vision. If steroid eye drops are used for long periods of time, they can lead to clouding of your lenses (cataracts) or to raised pressure in your eye (glaucoma).
Treatment to relieve pain and discomfort
Cycloplegic eye drops: these are eye drops that relieve pain by causing the pupil in your eye to widen (dilate) by relaxing the muscle in the ciliary body. As a result, the inflamed iris is able to rest and recover. Examples include atropine and cyclopentolate eye drops. There are some side-effects. They can make your pupil appear large, and can cause temporary blurred vision and difficulty with focusing. When the effect of the drops wears off, these side-effects disappear. If these drops are not used, the inflammation in the iris may cause it to become 'stuck' to the lens, causing permanent scarring.
Dark glasses: if your symptoms include sensitivity to bright light (photophobia), wearing dark glasses may be helpful.
Painkillers: painkilling medication, such as paracetamol, may also help.
Steroids by mouth or injection
In severe uveitis, steroids are sometimes given by injection into or around your eye. They can also be given by mouth. These can have side-effects if used in the long term. The main side-effects from oral steroids occur when they are used for more than a few weeks.
These include:
'Thinning' of the bones (osteoporosis).
Thinning of the skin.
Weight gain.
Muscle wasting.
A generally increased risk of infection.
Immunosuppressive medicines
If steroid treatment is needed in the longer term to treat uveitis, a second medicine known as an immunosuppressive medicine may be used. This can help to reduce the amount of steroids needed and/or help to control the uveitis if steroids are not working.
Biological agents
There are a number of new treatments for uveitis that are currently being investigated. These include medicines called TNF alpha-blockers, such as etanercept and infliximab.
Treatment of underlying conditions and causes
If there is an underlying cause of your uveitis this also needs to be treated (if possible). This means treating any underlying infection, inflammatory disease or autoimmune disease.
Surgery
Occasionally, surgery is needed to treat uveitis - usually persistent (chronic) uveitis. Surgery is used in addition to the other treatments mentioned above. Uveitis cannot be treated by surgery alone.
If someone has persistent floaters that are affecting their ability to see, the vitreous humour in the eye can be removed. Floaters tend to develop because of inflammation causing damage to the vitreous humour.
Surgery may also be used to treat cataracts or glaucoma that can occur as a consequence of steroid treatment.
What are the complications of uveitis?
Back to contentsComplications that can sometimes occur with uveitis include:
Formation of synechiae: the name 'synechiae' is given to the 'bands' of tissue that can form between the iris and the lens due to inflammation. Eye drops which cause the pupils to widen (dilate) help to prevent synechiae.
Glaucoma: the inflammation in your eye may cause the pressure in your eye to increase and can cause glaucoma. Using steroids can also cause a sudden increase in pressure in your eye, especially if you already have glaucoma. If glaucoma is not treated, it can lead to loss of vision. See the separate leaflet called Chronic Open-angle Glaucoma for more details.
Macular oedema: this is the term for fluid building up in the back of your eye around your macula on your retina. It may cause permanent visual loss. In addition, holes may form in the macula, leading to areas of lost vision on the retina.
Cataract formation: eye inflammation can cause clouding of the lens (cataract formation). Cataracts may also be caused by long-term steroid treatment. If a cataract worsens and is not treated, it can lead to visual loss. See the separate leaflet called Cataracts for more details.
Retinal detachment: the inflammation can cause 'pulling' on your retina so that it 'comes away' or is detached from the blood vessels below. This can cause you to experience flashing lights, floaters and problems with your vision. If you suspect that you have a retinal detachment, contact your doctor immediately, as urgent treatment is often needed. See the separate leaflet called Retinal Detachment for more details.
If uveitis is not treated quickly, it can lead to permanent loss of vision. It may also lead to complications, such as raised pressure in your eye (glaucoma). These complications can themselves affect your eyesight. If complications are not detected early, they can sometimes have a more harmful (detrimental) effect on your eyesight than the underlying uveitis.
The complications of uveitis may be caused by the effects of the inflammation inside the eye. Some of them may also be caused by the steroid treatment used to control the inflammation. Despite this, as a general rule, using enough steroids to control the uveitis will generally give a better outcome than using too few steroids and not controlling the inflammation.
What is the outlook for uveitis?
Back to contentsIn general, the sooner treatment for front of eye (anterior) uveitis is started, the better the outlook (prognosis) and the quicker it goes away. However, anterior uveitis can come back (recur), especially if it is associated with an underlying illness such as autoimmune or inflammatory disease.
Anterior uveitis can sometimes become persistent (chronic) despite early and adequate treatment.
Intermediate uveitis and posterior uveitis are more likely to last for a longer time or to become chronically recurrent. Some people who have recurrent uveitis learn to recognise their symptoms. They are sometimes given steroid eye drops to keep in reserve and start when their usual symptoms reappear. People who have chronic or recurrent uveitis are usually under the long-term care of an eye specialist and have regular check-ups in the outpatient clinic.
Uveitis caused by infection generally clears up when the infection is treated, and does not recur.
Frequently asked questions
Back to contentsIs uveitis curable?
There is no cure for uveitis but it can usually be treated. With prompt treatment, inflammation can be controlled and vision preserved, though some people may experience recurrences or long-term complications.
What is the difference between conjunctivitis and uveitis?
Conjunctivitis affects the outer layer of the eye and causes redness, irritation, and discharge, while uveitis is inflammation deeper inside the eye that can lead to pain, light sensitivity, and blurred vision. Uveitis is generally more serious and requires quick medical treatment to prevent complications.
Can you live a normal life with uveitis?
Yes, many people with uveitis can live a normal life with the right treatment and regular eye checks. Managing inflammation early and following your treatment plan can help prevent vision problems and keep symptoms under control.
Is uveitis contagious?
Uveitis is not contagious, meaning you can’t catch it from someone else. It’s usually caused by inflammation inside the eye linked to autoimmune conditions, infections, or injuries rather than something that spreads between people.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Eye conditions

Eye health
Myopia
The medical name for short-sightedness is myopia. Eyesight problems, such as myopia, are also known as refractive errors. Short-sightedness leads to blurred vision when looking at things at a distance, whilst close vision is usually normal. Short-sightedness is a very common problem that can be corrected by glasses, contact lenses, or laser eye surgery.
by Dr Philippa Vincent, MRCGP

Eye health
Eye problems
Eye problems range from everyday irritations to serious internal conditions. This leaflet contains a list of conditions which affect the eye, grouped together by the part of the eye which is affected or involved.
by Dr Toni Hazell, MRCGP
Further reading and references
- Uveitis; NICE CKS, March 2025 (UK access only)
- Duplechain A, Conrady CD, Patel BC, et al; Uveitis. StatPearls, Aug 2023.
- Chang MH, Shantha JG, Fondriest JJ, et al; Uveitis in Children and Adolescents. Rheum Dis Clin North Am. 2021 Nov;47(4):619-641. doi: 10.1016/j.rdc.2021.07.005. Epub 2021 Aug 27.
- Gamalero L, Simonini G, Ferrara G, et al; Evidence-Based Treatment for Uveitis. Isr Med Assoc J. 2019 Jul;21(7):475-479.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Dec 2027
19 Dec 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.