Balanitis
Peer reviewed by Dr Caroline Wiggins, MRCGP Last updated by Dr Toni Hazell, MRCGPLast updated 5 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Penis problems, itchy penis, and penis painPremature ejaculationPeyronie's diseasePenile cancerCircumcisionPhimosis and paraphimosis
Balanitis is a condition that causes the head of the penis to become inflamed, causing redness, soreness, or irritation under the foreskin. It’s more common in uncircumcised men and is usually treatable.
In this article:
Video picks for Men's sexual health
Key points
Balanitis is inflammation of the head of the penis (glans), often causing redness, swelling, itching, or soreness. It is common and can happen at any age.
Common causes include poor hygiene, fungal or bacterial infections, allergies, or skin conditions.
Treatment depends on the cause and may involve antifungal or antibiotic creams, steroid creams for inflammation, and improved hygiene.
Prevention includes gently cleaning the head of the penis with water, avoiding harsh soaps, and drying thoroughly.
Continue reading below
What is balanitis?
Balanitis is when the tip (glans) of the penis becomes inflamed, causing redness, soreness, or irritation under the foreskin. It is more common in men who are uncircumcised and can be linked to hygiene issues, infections, or skin irritation. Inflammation of the foreskin is called posthitis, and inflammation of the glans and the foreskin is called balanoposthitis.
Balanitis is not a sexually transmitted infection (STI) and isn't contagious - meaning you cannot catch it from another person. However, balanitis can be caused by some STI's.
What is balanitis?
How common is balanitis?
Around 1 in 25 boys, and 1 in 30 uncircumcised men, will have balanitis at some point in their life. Men who have been circumcised are around two-thirds less likely to get balanitis.
Balanitis symptoms
Back to contentsThe most common symptoms of balanitis are as follows - they vary with the cause, so not every man with balanitis will have all of these symptoms:
Redness or inflammation of the head of the penis.
Itching or irritation.
Pain or tenderness.
Thick clumpy discharge under the foreskin.
Tight foreskin or difficulty pulling it back.
Pain or discomfort when peeing.
Lumps in your groin (enlarged lymph nodes).
Symptoms can range from a small patch of redness confined to part of the skin surface of the glans, to the whole glans becoming red, swollen and painful.
Balanitis
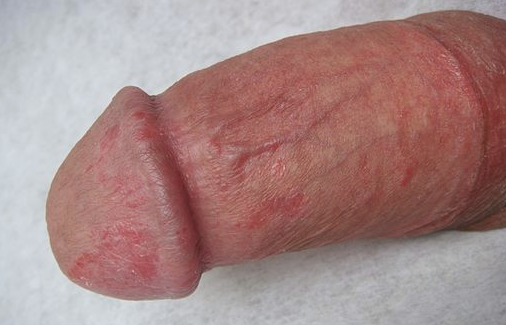
© By Pal1135 (Own work) assumed [based on copyright claims] via Wikimedia Commons
Continue reading below
What causes balanitis?
Back to contentsThe most common cause of balanitis is poor hygiene (not cleaning under the foreskin). A buildup of smegma (a thick, white, cheese-like substance) under the foreskin can irritate the head of the penis, causing inflammation.
Other causes of balanitis include:
Fungal infections - such as yeast infections caused by candida.
Bacterial infections - often caused by bacteria which are commonly found on the skin, such as staphylococcus and streptococcus.
Sexually transmitted infections - such as genital herpes, chlamydia, and gonorrhoea.
Irritants and allergies - from chemicals, condoms, soaps or washing powders.
Skin conditions - such as psoriasis, eczema, lichen sclerosus, lichen planus. or scabies.
Conditions in which there is oedema (fluid within the skin) - such as cirrhosis, heart failure, and nephrotic syndrome.
Obesity.
Zoon's balanitis
This affects middle-aged and older men, usually if they are not circumcised. The foreskin does not function properly and dead skin cells, urine, soap particles, and other debris are trapped under the foreskin. This leads to irritation of the foreskin and the head of the penis under it. There will be a clear patch on the glans which is red and shiny.
It is not caused by infection, and it can be difficult for a doctor just looking at it to be confident that there isn't a more serious cause - very occasionally a cancer of the penis can have a similar appearance. Treatment sometimes involves circumcision.
What increases the risk of balanitis?
Balanitis can affect any man, but it is more likely if you:
Have diabetes.
Use a device called a sheath to collect wee (urine) - this is like a condom which is worn permanently on the penis and collects your urine into a bag.
Never retract your foreskin.
Have an immune system which doesn't work properly - this may be because of a medical condition, or because you are taking a drug which suppresses the immune system to treat a medical condition.
Live in a nursing home.
Have severe obesity.
Have had trauma to the penis.
Wash your penis more often than is needed.
How is balanitis diagnosed?
Back to contentsA doctor can usually tell you have balanitis just by looking at the redness and swelling of the tip of the penis. Sometimes the cause is also obvious, for example, candida (yeast) infections often have a typical appearance.
If the cause isn’t clear, or if the balanitis doesn’t get better with treatment, the doctor may suggest some tests.
These include:
Taking a sample with a small ball of cotton wool on the end of a thin stick (a swab). The sample is used to look for certain germs (bacteria) that can cause infection.
A test to check for diabetes, HIV, or other conditions which cause the immune system not to work properly, if this is suspected.
Referral to a genitourinary medicine (GUM) clinic if an STI is a suspected cause.
Referral to a skin specialist if a skin condition or allergy is thought to be the cause. Allergy testing may be advised if an allergy is suspected.
Rarely, if the inflammation persists, removing a small sample of the inflamed skin tissue (a biopsy) may be suggested. This would be done by a skin specialist. The sample can be taken to be looked at under the microscope. This can help to find the cause. It is particularly common to do a biopsy if Zoon's balanitis is suspected, to make sure that the appearance of the penis isn't caused by a cancer.
Continue reading below
Balanitis treatment
Back to contentsThe treatment for balanitis depends on the cause. A doctor will often prescribe:
An anti-fungal cream or a course of anti-yeast tablets if it is caused by candida. Anti-fungal cream can also be bought in a pharmacy.
Antibiotics to clear infection caused by germs (bacteria), including certain STIs. If an STI is the cause, your sexual partner will also need treating and you will need to avoid sex for a period of time after the second person finishes their antibiotics.
A mild steroid cream to reduce inflammation caused by allergies or irritants.
Sometimes a steroid cream is used in addition to anti-yeast or antibiotic medication to reduce inflammation caused by infection. (Note: if there is infection of the end of the penis then a steroid cream should not be used alone, as steroids can make infection worse.)
If you are an adult with a recurring problem and have a condition where the foreskin does not pull back over the glans (a phimosis), an option is to be circumcised to remove the foreskin.
It is unusual for a child to have recurring balanitis. Your doctor may ask a specialist to advise.
General care
There are things that you can do if you have balanitis, regardless of the cause:
Avoid soaps when inflammation is present. You can use a moisturising cream or ointment (an emollient) to clean instead of soap.
Use lukewarm water to clean your penis and then dry gently.
Take salt baths to help soothe the glans whilst treatment takes effect.
If the balanitis is mild, this might be enough to allow it to clear up.
How can you cure balanitis?
Can balanitis be prevented?
Back to contentsTips which may help to prevent balanitis include:
Washing the end of the penis each day.
Pull the foreskin back gently whilst in the bath or shower. Then gently clean the glans using just water, or water and a bland soap.
Make sure the penis including the glans is clean and dry before you put on underpants.
Using a condom which is designed for sensitive skin if symptoms are related to condom use.
Using a condom each and every time you have sex with a new sexual partner.
Washing your hands before going to the toilet if you work with chemicals as they can irritate delicate skin.
Frequently Asked Questions
Back to contentsHow long does balanitis last?
Balanitis usually lasts up to two weeks from starting treatment. It may be better after a few days but it is important to complete the full course of treatment recommended by your doctor.
How to tell if balanitis is fungal or bacterial?
If balanitis is caused by an infection, your doctor will often be able to tell from the appearance whether it is caused by a fungus (usually candida) or bacteria. For example, a significant amount of thick, clumpy discharge would be a clue that the cause is likely to be fungal. Other symptoms of an STI might point the doctor towards suggesting STI testing. Sometimes a swab is taken and sent to a lab to confirm what type of infection there is.
Is balanitis dangerous?
Balanitis is not usually dangerous, however, if it is left untreated it can cause complications such as a spreading infection or scarring of the penis.
Does balanitis go away on its own?
Mild balanitis may go away on its own. The penis should be carefully washed and dried and you should avoid any irritants. If it does not start to get better within a few days it is important to see a doctor.
Can you have sex if you have balanitis?
You should avoid having sex if the balanitis is caused by an infection of if you do not know the cause.
Patient picks for Men's sexual health

Sexual health
Erectile dysfunction
Erectile dysfunction (ED) means that you cannot get and/or maintain an erection. In some cases the penis becomes partly erect but not hard enough to have sex properly. In other cases, there is no swelling or fullness of the penis at all. Both can have a significant effect on your sex life. Erectile dysfunction is sometimes called impotence. ED is usually treatable, most commonly by a tablet taken before sex. You may also receive lifestyle advice and treatments to minimise your risk of heart disease.
by Dr Doug McKechnie, MRCGP
Sexual health
Low testosterone
Low testosterone in men (testosterone deficiency) is often part of the ageing process and therefore common in older men. It can also occur at any age as a result of conditions affecting the testicles or the pituitary gland in the brain. Low testosterone can be treated with testosterone replacement therapy. Any underlying cause for the testosterone deficiency will also need treatment. The outlook will depend on the underlying cause.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Balanitis; NICE CKS, May 2024 (UK access only)
- Lam K, Cook DK; Chronic balanitis: When should we be concerned? Aust J Gen Pract. 2020 Dec;49(12):839-841. doi: 10.31128/AJGP-03-20-5283.
- Wray AA, Velasquez J, Khetarpal S; Balanitis. StatPearls, Jan 2024.
Continue reading below
About the author

undefined undefined
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 4 Aug 2027
5 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.