Chest infection
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 6 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Acute bronchitisPneumoniaAspiration pneumoniaPost-operative chest infectionBronchoscopy
A chest infection is an infection that affects your lower large airways (bronchi) and your lungs. Pneumonia and bronchitis are the most common chest infections. Bronchitis is usually caused by a viral infection, with between 1% and 10% of cases being caused by bacteria. Pneumonia is usually due to bacterial infection. Pneumonia may be serious and need hospital admission.
In this article:
Video picks for Chest and lung infections
Continue reading below
Chest infection symptoms
The main chest infection symptoms are:
A chesty cough.
Breathing difficulties (including shortness of breath and wheezing).
Chest pain or tightness.
Muscle aches and pains.
Feeling very tired.
A rapid heartbeat.
A cold - often called an upper respiratory tract infection (URTI) - usually starts with a combination of blocked and/or runny nose and sneezing, sometimes with a mild high temperature (fever).
You will usually get a cough, which is often dry and harsh but it can also sound like you have a lot of phlegm (sputum), which you may bring up. You may also feel tired and achy, but with the help of over-the-counter medications you'll be able to keep going with everyday activities.
Chest infections can start with these symptoms too, but you don't need to see a doctor if these are the only symptoms you have. The only exceptions are people with long-term health conditions affecting the lungs, like chronic obstructive pulmonary disease (COPD) and bronchiectasis. People with these conditions are more likely to develop serious complications.
What causes a chest infection?
Back to contentsThe vast majority of URTIs are caused by viral infections. Your immune system will fight these off without any help within a few days. Because URTIs are caused by viruses rather than bacteria, antibiotics won't help in any way. See the separate leaflet called Antibiotics.
Respiratory tract infections
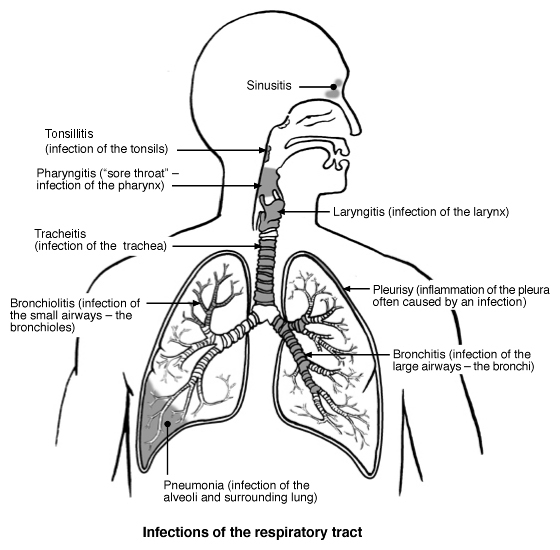
Read about sinusitis, tonsillitis, pharyngitis, laryngitis, tracheitis, pleurisy, bronchitis and pneumonia.
Sometimes an infection in the upper airways can spread deeper, causing a chest infection. Sometimes germs (bacteria) already living in your lungs can multiply, with the same result.
Types of a chest infection
There are two main types of chest infection - acute bronchitis and pneumonia.
Acute bronchitis
Bronchitis is inflammation due to infection of the bronchi. '-itis' is the medical term for inflammation. It can be acute or chronic. Acute means lasting a short time and chronic means lasting a long time.
Acute bronchitis is common and is often due to a viral infection. Infection with a germ (bacterium) is a less common cause. See the separate leaflet called Acute bronchitis for more details.
Pneumonia
This is usually a bacterial infection of the lung (bacterial chest infection) and may be serious. Treatment with antibiotics is usually needed. See the separate leaflet called Pneumonia for more details.
Continue reading below
Chest infection recovery time
Back to contentsA bout of infection of the large airways (bronchi) in the lungs (acute bronchitis) usually gets better on its own within 7-10 days without any medicines. If you suspect that you have a severe infection of the lung (pneumonia), you should see a GP.
Are chest infections contagious?
Back to contentsYou can pass a chest infection on to others through coughing and sneezing. So if you have a chest infection, it's important to cover your mouth when you cough or sneeze and to wash your hands regularly. You should throw away used tissues immediately.
Continue reading below
Chest infection treatment
Back to contentsAlthough most chest infections are mild and improve on their own, some cases can be very serious, even life-threatening.
When to see a doctor?
Infection of the large airways (bronchi) in the lungs (acute bronchitis) usually gets better by itself, so there is often no need to see a GP. However, you should contact a GP if you feel very unwell, particularly if you are feeling breathless.
If you have asthma or COPD you should take your doctor's advice.
They may have given you recommendations about increasing your inhaler medication or taking a 'rescue pack' of antibiotics and steroid tablets at the first sign of an infection (much more common for those with COPD than asthma).
If not, speak with them for advice if you develop chest infection symptoms.
You should also speak with a doctor or arrange a face-to-face consultation if you have a weakened immune system as it is more likely that you will need antibiotic treatment.
Warning signs of a chest infection
There are a number of chest infection symptoms that mean you should see a GP even if you do not have any other lung problems. If your symptoms get worse, you should look out for these warning signs. They include:
If a fever, wheezing or headache becomes worse or severe.
If you develop fast breathing, shortness of breath, or chest pains.
If you cough up blood or if your phlegm becomes dark or rusty-coloured.
If you become drowsy or confused.
If a cough lasts for longer than 3-4 weeks.
If you have repeated bouts of acute bronchitis.
If any other symptom develops that you are concerned about.
Antibiotics for a chest infection
Antibiotics are medicines used for infections caused by germs (bacteria) and don't work on viruses. Unless you have a long-term condition affecting your chest, your doctor is unlikely to prescribe antibiotics unless your symptoms and examination suggest you may have pneumonia.
Chest infection treatment at home
If you have a chest infection, you should:
Have plenty of rest.
Drink lots to prevent your body becoming lacking in fluids (dehydrated) and to help loosen the mucus in your lungs and make it easier to cough up.
Inhale steam vapour, perhaps with added menthol. Breathe in steam from a bowl of hot water - this can help to clear the mucus from your chest. Never use a bowl of hot water for a child's cough, in case they get scalded by accident; however, you could run a very hot bath to make the bathroom steamy and sit in the room with the child, safely away from the hot water.
Sleeping with an extra pillow to avoid lying flat at night to help keep your chest clear of mucus and make it easier to breathe.
Take paracetamol, ibuprofen or aspirin to reduce high temperature and to ease any aches, pains and headaches. (Note: children aged less than 16 years should not take aspirin.)
You should try to stop smoking for good if you smoke. Bronchitis, chest infections and serious lung diseases are more common in smokers as well as the long-term consequences such as lung disease, heart disease and cancer.
If your throat is sore from coughing, you can relieve the discomfort with a warm drink of honey and lemon.
What about cold and cough medicines for a chest infection?
You can buy many cold and flu remedies and cough medicines at pharmacies. These will help to make you feel better and help you to carry on with normal activities, but won't make the infection go away more quickly.
How is a chest infection diagnosed?
Your doctor will be able to make a diagnosis of a chest infection by listening to your story and examining you.
Often no tests are needed if you have infection of the large airways (bronchi) in the lungs (acute bronchitis) and your symptoms are mild. If your chest infection symptoms are more severe and you need to go to hospital then you may need to have the following tests:
A chest X-ray may be taken to be sure of the diagnosis and to see how bad the infection is.
Blood tests and phlegm (sputum) tests may be taken to find which germ (bacterium) is causing the serious lung infection (pneumonia). This helps to decide which antibiotic medicine is best to use. Sometimes the germ (bacterium) that is causing the pneumonia is resistant to the first antibiotic. A switch to another antibiotic is sometimes needed.
Are chest infections common?
Chest infections are very common, especially during the autumn and winter. They often occur after a cold or flu. Anyone can get a chest infection but they are more common in:
Young children and the elderly.
People who smoke.
Pregnant women.
People with long-term chest problems such as asthma, COPD, cystic fibrosis, heart disease, diabetes, kidney disease or liver disease.
People with an immune system that's weakened either by conditions such as some cancers (including lymphoma, myeloma and leukaemia) or AIDS; or by treatments such as high-dose steroids, chemotherapy or other medicines that can suppress your immune system.
How to prevent a chest infection
There are measures you can take to help prevent chest infections and to stop the spread of it to others. For instance, washing your hands regularly reduces the chance of germs getting into your system.
What is the outlook?
Infection of the large airways (bronchi) in the lungs (acute bronchitis) usually clears without any complications. Occasionally, the infection travels to the lung tissue to cause a serious lung infection (pneumonia).
If you have pneumonia and are well enough to be looked after at home, your outlook is very good. If you need to be looked after in hospital, the outlook is still usually good - but not quite as good. The outlook is also not as good for people who also have long-term illnesses such as lung disease, heart failure or diabetes.
Patient picks for Chest and lung infections

Chest and lungs
Aspiration pneumonia
Aspiration pneumonia is a lower respiratory tract (chest) infection caused by bacteria which have leaked into the lungs from fluid from the stomach or mouth. This can be as a result of vomiting or an inability to swallow properly. It causes symptoms of a lower respiratory tract infection (cough, fever, shortness of breath) and is usually treated with antibiotics.
by Dr Philippa Vincent, MRCGP

Chest and lungs
Legionnaires' disease
Legionnaires' disease is a serious lung infection (pneumonia) with chills, high temperature (fever) and muscle pains. You get the infection by breathing in droplets of water which contain legionella germs (bacteria) from contaminated water systems. The earlier the illness is treated with antibiotic medication, the better the likely outcome. The illness is serious and can be fatal. However, it cannot be passed from person to person (it is not contagious). Pontiac fever is a milder illness caused by the same bacterium.
by Dr Toni Hazell, MRCGP
Further reading and references
- Chest infections - adult; NICE CKS, May 2024 (UK access only)
- Antibiotic awareness resources: key messages on antibiotic use; Public Health England (now UK Health Security Agency)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Oct 2027
6 Oct 2024 | Latest version
7 May 2013 | Originally published
Authored by:
Dr Colin Tidy, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.